概述
Typical liver blood flow versus portal hypertension

Typical liver blood flow versus portal hypertension
In a healthy liver (top), blood flows in and is filtered, then is sent to the heart. With portal hypertension (bottom), blood gets blocked from flowing through the liver, often due to scarring called cirrhosis. That blood is forced into other veins that become enlarged (varices).
Portal hypertension means high blood pressure in the system of veins that carry blood from your digestive organs to your liver. This system, called the portal venous system, includes the large portal vein and smaller veins connected to it. Portal hypertension happens when blood gets blocked from or has trouble flowing through the liver.
A healthy liver filters blood, then returns it to the heart. But increased pressure in the portal venous system can force blood into other veins. This can lead to serious complications.
Portal hypertension can range from mild to severe. How severe it is depends on pressure levels in the portal venous system and the health of the liver. Mild portal hypertension may cause few or no symptoms and may be found during testing for another reason. Severe portal hypertension raises the risk of complications, such as bleeding in the digestive system, fluid buildup in the belly, and changes in thinking or alertness.
Some portal hypertension can be reversed, depending on the cause and how early it's found and treated. But most portal hypertension is caused by cirrhosis and cannot be cured or fully reversed. Ongoing treatment is needed to lower pressure and prevent and manage complications as well as treat the underlying cause.
Types
Healthcare professionals may describe portal hypertension based on where blood flow slows down or is blocked.
- Prehepatic portal hypertension. This is when blood flow slows or gets blocked before it reaches the liver. A common cause is a blood clot in the portal vein, called portal vein thrombosis.
- Intrahepatic portal hypertension. This is when blood has trouble moving through the liver itself.
- Posthepatic portal hypertension. In this type, blood flow slows down after leaving the liver.
A less common type is left-sided portal hypertension, also called sinistral portal hypertension. This rare type is high pressure that's mainly in the vein that drains the spleen, called the splenic vein. Left-sided portal hypertension is different from other portal hypertension in that the blockage usually happens because of pancreatic disease, such as pancreatitis, or surgery on the pancreas, not liver disease or cirrhosis. If left-sided portal hypertension is causing bleeding, the main treatment is to remove the spleen, called splenectomy, which usually cures the condition.
症状
瘀点
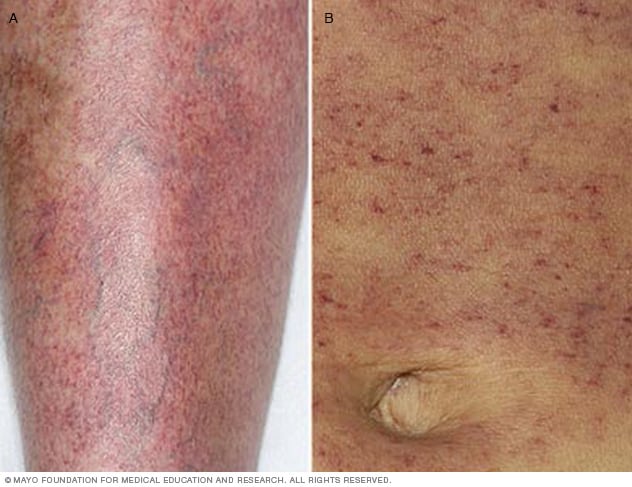
瘀点
瘀点是皮下出血形成的小点,外观可能类似皮疹。在较白皙的皮肤上,瘀点可能呈现红色或紫红色。在深色皮肤上,则可能呈褐色或难以察觉。此处图例中瘀点分别位于腿部(A)和腹部(B)。
Portal hypertension causes no symptoms at first. Symptoms usually start when the condition leads to complications. This often is a result of blood being forced out of the portal venous system into other veins and organs.
Symptoms and visible signs that may suggest portal hypertension complications include:
- Swelling in the belly or legs. Fluid buildup in the belly, called ascites, can cause the abdomen to look or feel swollen. Fluid also can build up and cause swelling in the legs, called edema.
- Blood in vomit or bloody stool. Blood in vomit may look like blood or coffee grounds. Blood in stool can be red or darker, even black. Bloody stool or vomit can happen if you have bleeding in your digestive system.
- Bleeding that is not typical; easy or a lot of bruising; or tiny dots on the skin that may look red, purple or brown. The tiny dots are called petechiae. All are possible symptoms of thrombocytopenia, which can happen if blood builds up in the spleen causing an enlarged spleen. A healthcare professional may feel an enlarged spleen during an exam or see it on an imaging test. The condition also can cause low white blood cell counts.
- Blood vessels visible on the skin of the belly. This can happen when blood that isn't able to move through the portal venous system in the liver finds other paths to travel.
- Changes in thinking or alertness. Trouble focusing, confusion or changes in sleep may happen when the brain is affected by toxins that the liver hasn't been able to filter out. This is called hepatic encephalopathy.
It's important to watch at home for these symptoms of portal hypertension complications and seek medical care when needed.
When to seek care
Contact your healthcare professional right away for:
- New or worsening symptoms mentioned earlier.
- Weight gain or loss outside the limits of what your health professional has said is OK.
- Trouble breathing.
When to seek emergency care
Call your healthcare professional or go to the nearest emergency medical care facility right away for:
- Vomiting blood.
- Bloody, black or dark-colored stool.
- Swelling of the belly, along with a fever, belly pain or confusion. This can mean there's fluid in the belly that's infected.
病因
Portal hypertension is high blood pressure in the portal vein, which carries blood from your digestive organs to your liver. It happens when blood flow is blocked or slowed down.
The two most common causes of portal hypertension worldwide are scarring of the liver, called cirrhosis, and a parasitic infection of the liver called schistosomiasis. In Western countries, more than 90% of portal hypertension is caused by cirrhosis. Cirrhosis makes it hard for blood to flow through the liver.
The causes of portal hypertension can be grouped by where the blockage or slowing of blood flow happens. This could be in an area before blood reaches the liver, inside the liver or after blood leaves the liver.
Before blood reaches the liver, also called prehepatic
Some causes of a blockage in the portal vein, before blood reaches the liver include:
- A blood clot in the portal vein, called portal vein thrombosis.
- A blood clot in the vein that carries blood from the spleen to the liver.
In children, blood clots can happen from:
- Infections, such as sepsis or an infection in a newborn's umbilical cord stump.
- Dehydration.
- Changes in the anatomy of the portal vein that are found at birth, such as the vein being too narrow.
Inside the liver, also called intrahepatic
This is the most common area where blockages happen, most often caused by cirrhosis.
Some causes of intrahepatic portal hypertension include:
- Cirrhosis. In children, cirrhosis can be caused by autoimmune hepatitis, biliary atresia, chronic viral hepatitis and metabolic liver diseases. In adults, causes can include long-term alcohol use disorder, hepatitis B, hepatitis C and liver diseases, such as hemochromatosis, metabolic dysfunction-associated steatotic liver disease — formerly known as nonalcoholic fatty liver disease — primary biliary cholangitis and Wilson's disease.
- Conditions such as sarcoidosis and amyloidosis, which can cause cirrhosis.
- Infections such as schistosomiasis, which can cause cirrhosis.
- Other conditions that may not cause cirrhosis but can lead to portal hypertension.
You may hear intrahepatic portal hypertension described as:
- Presinusoidal portal hypertension. This means the blood flow is blocked before blood reaches certain small blood channels inside the liver called the sinusoids. This is typically not caused by cirrhosis but by other liver conditions or infections.
- Sinusoidal portal hypertension. This means the blood flow is blocked at the point of the sinusoids in the liver. Cirrhosis is a sinusoidal cause of portal hypertension.
- Postsinusoidal portal hypertension. This means the blood flow is blocked after blood has reached the sinusoids in the liver.
After the liver, also called posthepatic
Some causes of blockages after blood leaves the liver can include:
- Budd-Chiari syndrome.
- A condition that affects the sac around the heart, called constrictive pericarditis.
- Serious heart conditions, such as cardiomyopathy.
- A blockage, such as a blood clot, in the vein that carries blood to the heart.
If a cause cannot be found, you may hear that referred to as idiopathic.
风险因素
Different factors can increase the risk of portal hypertension. Some you may be able to change, whereas others you cannot.
Factors you can change
- Heavy drinking. This can contribute to liver damage and cirrhosis, the main cause of portal hypertension.
- Infections. Ongoing infections with hepatitis B or hepatitis C can damage the liver and lead to cirrhosis and portal hypertension.
- Conditions that contribute to liver damage. When combined, conditions such as diabetes, steatotic liver disease — formerly called fatty liver disease — high cholesterol and high blood pressure can increase the risk of liver damage and portal hypertension.
Factors you cannot change
- Inherited conditions. Liver conditions passed down in families, such as hemochromatosis and Wilson's disease, increase the risk of liver damage and portal hypertension.
- Changes in the portal vein that are found at birth. Sometimes, a person is born with portal vein anatomy that increases the risk of portal hypertension. For example, the portal vein may be too narrow.
并发症
Portal hypertension often is noticed only after complications start.
Complications can include:
- Fluid buildup in the belly, also called ascites. When the liver is damaged, such as with portal hypertension, the kidneys hold excess salt. The salt causes the body to hold onto water, and fluid builds up in the belly. This complication called ascites. With portal hypertension, fluid also may leak out of blood vessels into the belly. This happens because of the increased pressure in the portal vein system, Sometimes, ascites can become infected, called spontaneous bacterial peritonitis.
-
Enlarged veins, also called varices, and bleeding. Increased blood pressure in the liver's portal vein system can force blood to seek other routes. This includes the veins of the esophagus, stomach and intestines. When pressure in those veins increases, it can cause the veins to enlarge, a condition called varices. Varices in the esophagus are called esophageal varices. Varices in the stomach are called gastric or stomach varices.
Varices are fragile due to their thin walls. This increases the risk of bleeding. When varices bleed, blood can build up in the stomach. Larger varices are more likely to bleed. Spots on the skin over varices also suggest a higher risk of bleeding. Sometimes varices form in the rectum, where they can bleed. This is not the same as hemorrhoids.
- Changes in thinking or alertness. When the liver can't filter toxins from the blood, such as ammonia from the intestines, the toxins can build up and affect how the brain works. This is called hepatic encephalopathy. The condition can lead to confusion, changes in personality, trouble concentrating and, when severe, coma.
- Stomach and colon changes and bleeding. Pressure from portal hypertension can lead to more blood in blood vessels in the lining of the stomach and large intestine, also called the colon. This buildup of blood can cause those blood vessels to swell and bleed. The bleeding may be slow and ongoing. It's not usually a cause of a large amount of bleeding, but the bleeding can cause anemia. In the stomach, this is called portal hypertensive gastropathy. In the colon, it's called portal hypertensive colopathy.
- Enlarged spleen and low platelet count. The spleen acts as a filter for blood. When portal hypertension causes blood to back up and pool in the spleen, the spleen can swell in size, called splenomegaly. As the spleen enlarges, it can trap and destroy more blood cells, including platelets. This leads to a low platelet count, called thrombocytopenia. This condition can limit how well the blood clots and increase the risk of bleeding.
- Kidney failure. Portal hypertension is not the same as kidney failure. But high blood pressure in your liver from portal hypertension, along with fluid in the belly, called ascites, can contribute to kidney failure. This is called hepatorenal syndrome. Portal hypertension causes the blood vessels in your belly to widen. This can affect blood flow and mean your kidneys don't get enough blood. In addition, if portal hypertension leads to ascites, that fluid can become infected and trigger kidney failure.
- Low oxygen in the blood. High blood pressure in your liver from portal hypertension sometimes leads to the blood vessels in your lungs enlarging. These changes in the lungs make it hard for red blood cells to take in oxygen. Then the lungs can't send enough oxygen to the body. This condition is called hepatopulmonary syndrome.
预防
Taking steps to prevent or manage liver disease can help prevent complications such as portal hypertension.
- Limit or avoid alcohol. This can reduce the risk of liver disease, cirrhosis and other complications such as portal hypertension.
- Prevent infections such as hepatitis B or hepatitis C. This can reduce the risk of liver disease and cirrhosis, which can lead to portal hypertension.
- Manage existing conditions. These include liver conditions, such as hepatitis B, hepatitis C and steatotic liver disease — formerly called fatty liver disease — as well as high cholesterol and high blood pressure. Managing these conditions with lifestyle changes and medicines may help prevent complications, such as portal hypertension.
临床试验
探索 Mayo Clinic 的研究 测试新的治疗、干预与检查方法,旨在预防、检测、治疗或控制这种疾病。