概述
肝脏
肝脏
肝脏是人体内最大的器官,主要位于右上腹,在横膈膜下方、胃的上方。
血色病是一种由家族遗传的基因改变引起的铁过载疾病。铁过载疾病是指任何导致身体蓄积过多铁的状况。铁过载疾病包括以下几种:
血色病与含铁血黄素沉着症有所不同。含铁血黄素沉着症意味着铁已开始在身体组织中积聚,但尚未造成器官损害。这些状况也与单纯的铁水平较高不同。“铁水平高”这一术语通常是指血液检测显示铁含量高于正常水平。但这未必意味着铁已在器官中蓄积。
血色病的治疗通常包括定期从体内排血。由于体内很多铁都包含在红细胞中,因此这可降低铁水平。
症状
有些血色病患者从未出现过症状。他们可能通过常规血液检测被诊断出来,有时进行检测是因为有这种状况的家族史。
早期体征和症状
铁过载的早期体征和症状(包括遗传性血色病的症状)通常与其他常见状况的症状相似。其中或许包括:
任何血色病患者都可能出现这些症状。但根据出生指定性别,症状会存在一些差异。
男性血色病患者的症状:
- 性欲减退。
- 勃起不坚且维持时间不足,无法进行性活动,又称阳痿。
女性血色病患者的症状:
- 闭经。
- 症状通常在年龄较大时出现。这可能是因为铁会在经期和孕期流失。因此,体内储存的铁较少。在绝经或子宫切除术后,这种情况会发生改变。
其他体征和症状
铁过载的症状(包括遗传性血色病的症状)还可能包括:
- 糖尿病。
- 心脏问题和状况,例如心律改变和心力衰竭。
- 肝衰竭。
- 可见的皮肤变化,包括皮肤呈青铜色或灰色。当患者同时患有 2 型糖尿病且皮肤呈青铜色时,有时会使用“青铜色糖尿病”这一术语。
- 影响视力的眼部变化。
症状通常何时出现
最常见的一种血色病是先天性血色病。但大多数人要到年龄较大时才会出现症状。对于男性,症状通常在 40 岁以后开始出现。女性更有可能在绝经后或 60 岁以后出现症状。
何时就诊
如果出现血色病的任何症状,请到医务人员处就诊。如果您的父母一方、兄弟姐妹或子女患有血色病,请向医护团队咨询基因检测的相关事宜。基因检测可以检查您是否携带可能增加血色病患病风险的基因。
病因
健康肝脏与肝硬化
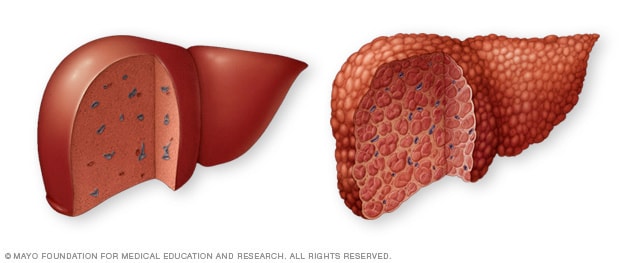
健康肝脏与肝硬化
健康肝脏(左图)没有瘢痕形成的迹象。出现肝硬化(右图)时,瘢痕组织会取代健康肝脏组织。
血色病又称遗传性血色病,是一种由基因改变(又称基因突变)引起的遗传性铁过载疾病。这种基因改变会在家族中遗传。它是迄今为止最常见的铁过载疾病类型。
其他类型的铁过载并非遗传性疾病。它们可能被称为继发性铁过载或获得性铁过载。
血色病的遗传原因
遗传性血色病可由不同基因发生突变引起,这些基因负责控制人体从食物中吸收铁的量。
- HFE 基因。 称为 HFE 的基因是导致遗传性血色病最常见的原因。这是一种主要影响中年成人的血色病类型。HFE 基因有两种常见突变:C282Y 和 H63D。
- HJV、HAMP 或 TFR2 基因。 这些基因中任何一个发生突变都可能引起一种称为青少年血色病的血色病。青少年血色病影响年轻人。它引起的症状与遗传性血色病在成人患者中引起的症状相同。但铁积聚开始得更早,因此通常会在 15 到 30 岁出现症状。
如果您从父母双方各遗传到一个基因突变,你可能会患上血色病。您也可能将突变基因传给您的孩子。但遗传了两种突变基因的人不一定会发生与血色病铁过载相关的症状。
如果您从父母一方遗传到一个基因突变,您不太可能患上血色病。但是,您会被认为是携带者,并且可能将突变基因遗传给您的孩子。只要孩子没有从父母另一方遗传获得另一种突变基因,就不会患病。
继发性或获得性铁过载的病因
有些铁过载并非由家族遗传的基因改变引起。示例包括:
- 新生儿血色病是一种严重疾病,指患儿在子宫内发育期间,铁在其肝脏中迅速积聚。其被视为一种自身免疫性疾病(即身体攻击自身)。
- 继发性铁过载可由导致肠道吸收过多铁的其他状况(例如肝病)引起,也可由过量饮酒引起。也可能由体内铁含量过多引起,例如为了治疗贫血或其他状况而接受了过多次输血。较少见的情况下,过量服用铁补充剂也可导致继发性铁过载。
单靠饮食通常不会导致铁过载。但在极少数情况下,部分非洲裔和非裔美国人血统的人群可能会因饮食中铁含量过高而导致风险增加。这很可能是由于家族遗传的基因改变所致。
铁过载如何累及器官
铁对多种身体功能起重要作用,包括帮助生成血液。但铁过多会导致中毒。
铁调素是一种由肝脏分泌的激素,可控制体内铁的使用和吸收,以及如何将多余的铁储存于不同器官中。血色病会影响铁调素发挥作用,导致身体吸收的铁量超过需要。
在其他铁过载疾病中,身体并不会从食物中吸收过多的铁,而通常是因多次输血所致。
在血色病和其他铁过载疾病中,多余的铁被储存在主要器官中,尤其是肝脏。经过数年时间,储存的铁可能会导致严重损伤,从而可能导致器官衰竭。它还可能导致长期疾病,例如肝硬化、糖尿病和心力衰竭。许多人都携带导致血色病的基因改变。但并非所有人都会发生足以造成组织和器官损伤的铁过载。
风险因素
增加患血色病风险的因素包括:
- 携带两个 HFE 突变基因。 这是导致遗传性血色病的最大风险因素。
- 家族史。 父母或兄弟姐妹有血色病者更有可能患病。
- 种族。 北欧血统的人群比其他种族背景的人群更易患遗传性血色病。
- 出生指定性别。 男性比女性更有可能在较为年轻时出现血色病的症状。因为女性经期和孕期都会流失铁,体内这种矿物质的储量往往更少。绝经后或子宫切除后的女性则有更高风险。
并发症
若不予治疗,血色病和铁过载可引发多种并发症。这些并发症尤其会累及关节和通常储存过量铁的器官(例如肝脏、胰腺和心脏)。并发症可能包括:
- 肝脏问题。 肝硬化是肝脏永久性瘢痕形成。其仅仅是可能出现的并发症之一。肝硬化会增加肝癌及其他危及生命并发症的风险。
- 糖尿病。胰腺损伤可能会引发糖尿病。
- 心脏状况。 心脏内铁过量会影响心脏循环足够的血液以满足身体需求的能力。这被称为充血性心力衰竭。血色病还可能会导致心律不齐(称为心律失常)。
- 生殖问题。 铁过量会导致男性勃起功能障碍和性欲减退,并导致女性停经。
- 皮肤颜色改变。 皮肤细胞中的铁沉积可能会使皮肤呈青铜色或发灰。