Overview
Skin anatomy
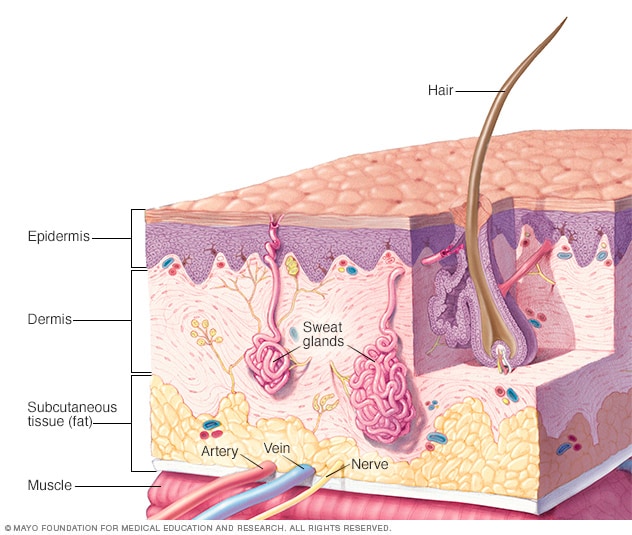
Skin anatomy
Your skin has three layers that house your sweat and oil glands, hair follicles, melanocytes, and blood vessels.
Shave biopsy
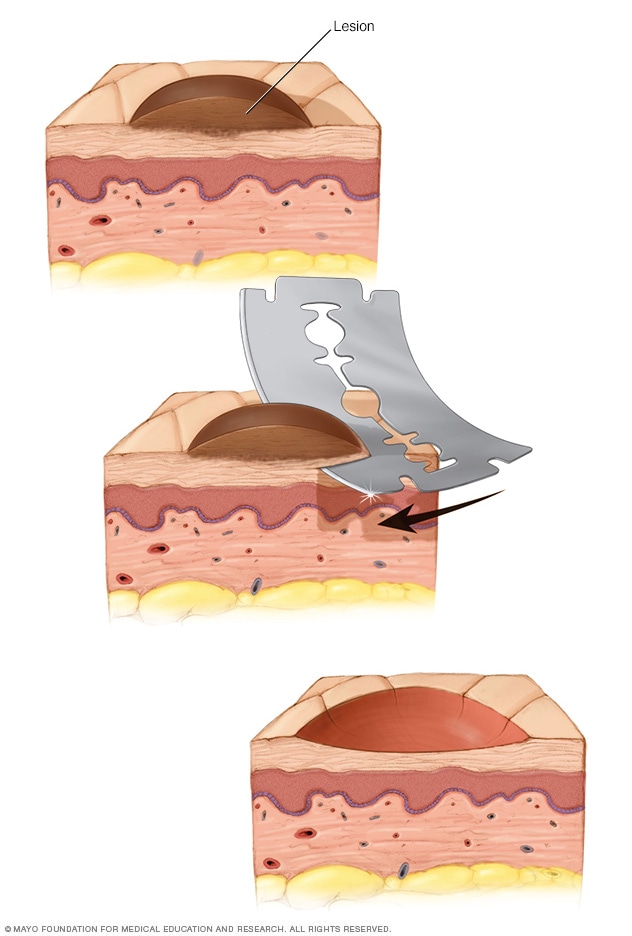
Shave biopsy
During a shave biopsy, a scalpel or a razor blade is used to scrape the surface of the skin. The goal is to remove irregular tissue to send to the lab. Stitches usually aren't needed after this procedure.
Punch biopsy
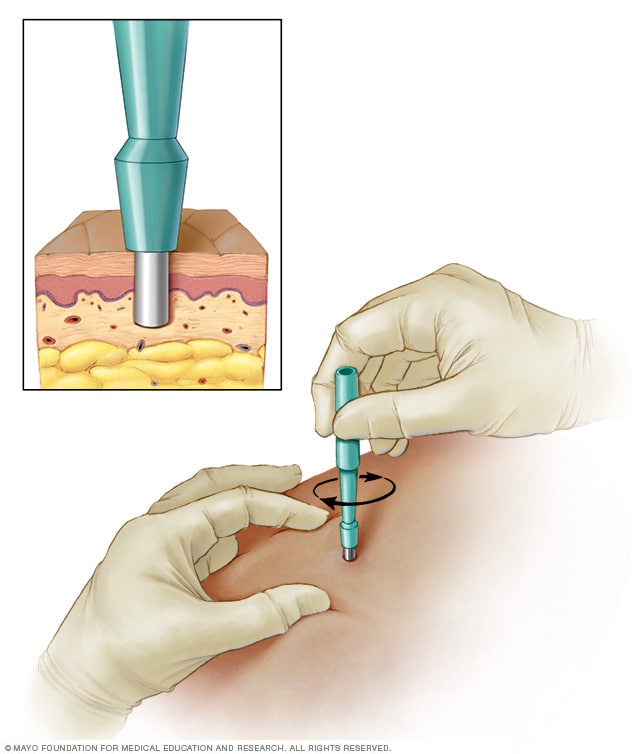
Punch biopsy
During a punch biopsy, a round-tipped cutting tool is used to remove deeper layers of skin for testing. Depending on the size, stitches may be needed to close the wound.
Excisional biopsy
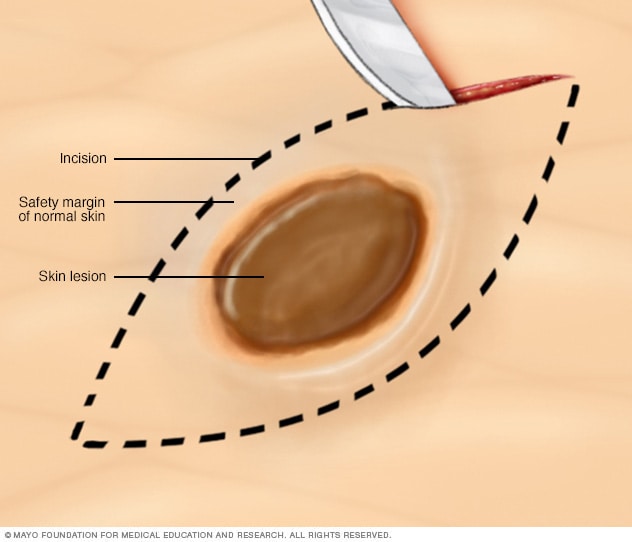
Excisional biopsy
During an excisional biopsy, a scalpel is used to cut out a lump or an area of irregular skin and some surrounding healthy skin. As a rule, stitches are needed to close the wound.
A skin biopsy is a procedure to remove cells or skin samples from your body so that they can be tested in a lab. A skin biopsy is often used to diagnose or rule out certain skin conditions and diseases.
Common skin biopsy procedures include:
- Shave biopsy. Shave biopsy may be used to remove a small section of the top layers of skin. These layers are called the epidermis and the dermis. Stitches usually aren't needed after this procedure.
- Punch biopsy. Punch biopsy may be used to remove a small section of skin, including deeper layers. The sample might include tissue from layers called the epidermis, the dermis and the top layer of fat under the skin. You may need stitches to close the wound.
- Excisional biopsy. Excisional biopsy may be used to remove an entire lump or an area of irregular skin. The sample of removed tissue might include a border of healthy skin and your skin's deeper layers. You may need stitches to close the wound.
The type of skin biopsy you have depends on your symptoms and where on your body the procedure is to be done.
Products & Services
Why it's done
Your healthcare professional may suggest a skin biopsy to help diagnose or treat a disease or condition. Examples include:
- Actinic keratosis.
- Blistering skin disorders.
- Skin cancer.
- Skin tags.
- Irregular moles or other growths.
More Information
Risks
Skin biopsy carries a small risk of bleeding, bruising and infection at the site where the skin sample was removed. Some mild pain can be expected after a skin biopsy, though it is usually controlled with pain relievers. Sometimes an antibiotic ointment is put on the area after biopsy. This may cause an allergic reaction in some people.
After the wound heals, you may have a scar. Some people develop a thick, raised scar. This type of scar, also called a keloid scar, is more common in people with brown or Black skin. The risk of a keloid scar also is higher when a biopsy is done on the neck, back or chest.
How you prepare
Most skin biopsy procedures don't require any preparation on your part.
Your healthcare professional may ask whether you:
- Have a bleeding disorder.
- Have had heavy bleeding after other medical procedures.
- Take any supplements or medicines that thin your blood.
- Have a history of skin infections.
- Have had reactions to tape, creams or gels applied to your skin.
What you can expect
During the skin biopsy
Depending on the location of the skin biopsy, you may be asked to undress and change into a clean gown.
Your healthcare team will clean the site of the biopsy and mark the outline of the site. An anesthetic may be injected into the skin around the area to numb it. The numbing medicine can cause a burning feeling in the skin for a few seconds. After that, you shouldn't feel any pain during the skin biopsy. To make sure the numbing medicine is working, your healthcare professional may prick your skin with a needle and ask you if you feel anything.
What you can expect during your skin biopsy depends on the type of biopsy you'll undergo.
- For a shave biopsy, the healthcare professional may use a razor blade or scalpel to scrape the tissue. The depth of the cut varies. A shave biopsy causes bleeding. Pressure and a medicine might be applied to stop the bleeding.
- For a punch biopsy or an excisional biopsy, the healthcare professional cuts into the top layer of fat beneath the skin. Stitches may be needed and a bandage is applied.
A skin biopsy takes about 15 minutes. At any point in the process, tell your healthcare team if you're feeling uncomfortable.
After the skin biopsy
Once your healthcare team has collected enough cells or tissue for analysis, your skin biopsy procedure is complete. Your biopsy sample is sent to a lab for analysis. The results may be available in a few days, though more-technical tests may require more time. Ask your healthcare professional how long you can expect to wait.
Your healthcare team applies a bandage over the area of the biopsy. You may be asked to apply pressure to the bandage for several minutes to ensure there is minimal bleeding. In most cases, you can leave when the procedure is completed and you've been told how to care for the wound.
Sometimes the biopsy site bleeds after you leave the clinic. This is more likely in people taking blood-thinning medicine. If this occurs, apply direct pressure to the covered biopsy site for 20 minutes, then look at it. If bleeding continues, apply pressure for another 20 minutes. If bleeding still continues after that, contact your healthcare professional.
Biopsies usually cause a small scar. They tend to fade with time. The scar's permanent color will be set 1 to 2 years after the biopsy.
Avoid bumping the biopsy site or doing activities that stretch the skin. Stretching the skin could lead to bleeding or a bigger scar. Don't soak in a bathtub, swimming pool or hot tub until your healthcare professional says it's OK — usually about seven days after the procedure.
Healing can take several weeks. Wounds on the legs and feet tend to heal slower than those on other areas of the body.
Clean the biopsy site two times a day unless it's on your scalp. Scalp wounds can be cleaned once a day. Follow these steps:
- Wash your hands with soap and water before touching the biopsy site.
- Wash the biopsy site with soap and water. If the biopsy site is on your scalp, use shampoo.
- Rinse well and pat dry with a clean towel.
- Apply a thin layer of petroleum jelly. Use a new container of petroleum jelly the first time you do wound care. Use a new cotton swab each time you apply the product.
- Cover the site with a bandage (Band-Aid, Curad, others) for 2 to 3 days after the procedure.
If you have stitches, continue wound care until they're removed. If you don't have stitches, take these wound care steps until the skin is healed.
If your wound is sore, ask your healthcare professional if you can apply ice wrapped in a thin towel. If your wound shows signs of infection, contact your healthcare team. Signs of infection include fever, chills, increased pain, and swelling or pain at the biopsy site.
Results
Doctors who specialize in studying cells and tissue samples for signs of disease study the biopsy sample in a laboratory. These specialists, called pathologists, create a pathology report for your healthcare professional, who may schedule an appointment with you to discuss the results. You might want to bring along a family member or friend to help you absorb all the information.
List questions that you want to ask your healthcare professional, such as:
- Based on the results, what are my next steps?
- What kind of follow-up, if any, should I expect?
- Is there anything that might have affected or altered the test results?
- Will I need to repeat the test?
- If the skin biopsy showed skin cancer, was all of the cancer removed?
- Will I need more treatment?
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.