Overview
Neurodermatitis
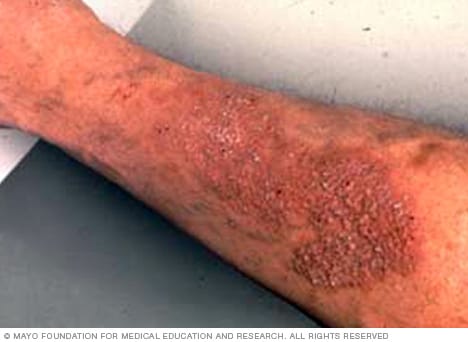
Neurodermatitis
Neurodermatitis is a skin condition characterized by chronic itching or scaling. You'll notice raised, rough, itchy areas of skin — typically on the neck, wrists, forearms, legs or groin area.
Neurodermatitis is a skin condition that starts with an itchy patch of skin. Scratching makes it itch more. With more scratching, the skin becomes thick and leathery. You may develop several itchy spots, typically on the neck, wrists, forearms, legs or groin area.
Neurodermatitis — also known as lichen simplex chronicus — is not life-threatening or contagious. But the itching can be so intense it disrupts your sleep, sexual function and quality of life.
Breaking the itch-scratch cycle of neurodermatitis is challenging, and neurodermatitis is usually a long-term condition. It may clear up with treatment but often returns. Treatment focuses on controlling the itching and preventing scratching. It also may help to identify and eliminate factors that worsen your symptoms, such as dry skin.
Products & Services
Symptoms
Symptoms of neurodermatitis include:
- An itchy, scaly skin patch or patches
- Open sores that bleed
- Thick, leathery skin
- Discolored, wrinkled genital skin
- Raised, rough patches that are inflamed or darker than the rest of the skin
The condition involves areas that can be reached for scratching — the scalp, neck, wrists, forearms, ankles, vulva, scrotum and anus. The itchiness, which can be intense, may come and go or be nonstop. You may scratch your skin out of habit and while sleeping.
When to see a doctor
See your health care provider if home remedies haven't helped after two days and:
- You catch yourself repeatedly scratching the same patch of skin
- The itch prevents you from sleeping or focusing on your daily routines
Seek immediate medical care if your skin becomes painful or looks infected and you have a fever
Causes
The exact cause of neurodermatitis isn't known. It can be triggered by something that irritates the skin, such as tight clothing or a bug bite. The more you scratch, the more it itches.
Sometimes, neurodermatitis goes along with other skin conditions, such as dry skin, atopic dermatitis or psoriasis. Stress and anxiety also can trigger itching.
Risk factors
Factors that can increase the risk of neurodermatitis include:
- Age. The condition is most common among people between 30 and 50 years of age.
- Other skin conditions. People who have or had other skin conditions, such as atopic dermatitis or psoriasis, are more likely to develop neurodermatitis.
- Family history. People whose blood relatives have or had hay fever, childhood eczema or asthma may be more likely to develop neurodermatitis.
- Anxiety disorders. Anxiety and emotional stress can trigger neurodermatitis.
Complications
Persistent scratching can lead to a wound, a bacterial skin infection, or permanent scars and changes in skin color (postinflammatory hyperpigmentation or hypopigmentation). The itch of neurodermatitis can affect your sleep, sexual function and quality of life.
Sept. 18, 2024