Overview
Melanoma
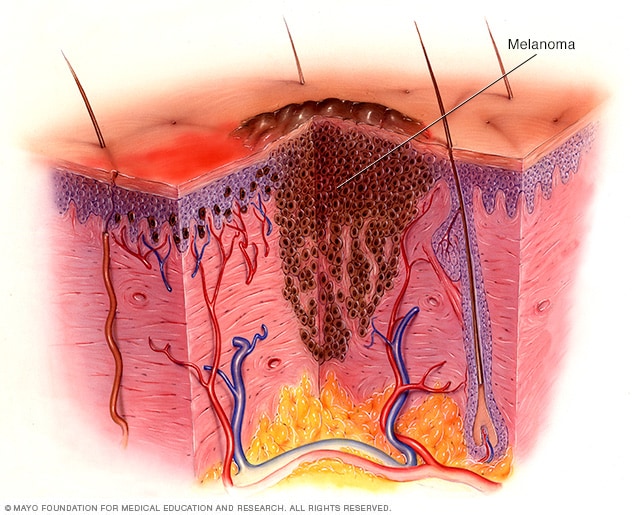
Melanoma
Melanoma is a kind of skin cancer that starts in the melanocytes. Melanocytes are cells that make the pigment that gives skin its color. The pigment is called melanin. This illustration shows melanoma cells extending from the surface of the skin into the deeper skin layers.
Melanoma is a kind of skin cancer that starts in the melanocytes. Melanocytes are cells that make the pigment that gives skin its color. The pigment is called melanin.
Melanoma typically starts on skin that's often exposed to the sun. This includes the skin on the arms, back, face and legs. Melanoma also can form in the eyes. Rarely, it can happen inside the body, such as in the nose or throat.
The exact cause of all melanomas isn't clear. Most melanomas are caused by exposure to ultraviolet light. Ultraviolet light, also called UV light, comes from sunlight or tanning lamps and beds. Limiting exposure to UV light can help reduce the risk of melanoma.
The risk of melanoma seems to be increasing in people under 40, especially women. Knowing the symptoms of skin cancer can help ensure that cancerous changes are detected and treated before the cancer has spread. Melanoma can be treated successfully if it is found early.
Products & Services
Symptoms
Moles
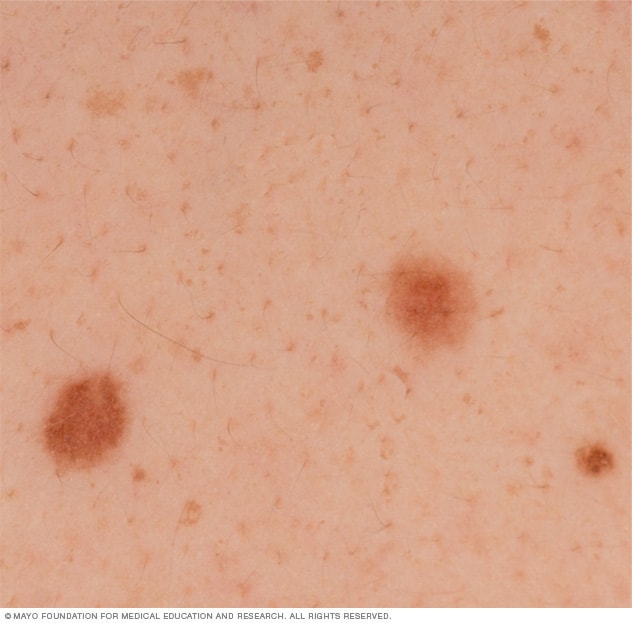
Moles
Moles are usually harmless. They may contain hairs or become raised or wrinkled. Talk to your doctor about any change in the color or size of a mole or if itching, pain, bleeding or inflammation develops.
Melanoma
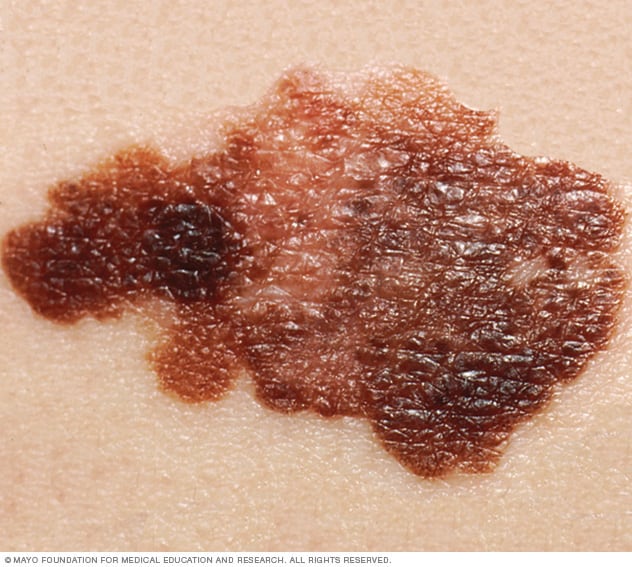
Melanoma
The first sign of melanoma is often a mole that changes size, shape or color. This melanoma shows color variations and an irregular border, both of which are melanoma warning signs.
The first melanoma signs and symptoms often are:
- A change in an existing mole.
- The development of a new pigmented or unusual-looking growth on the skin.
Melanoma doesn't always begin as a mole. It also can happen on otherwise healthy skin.
Melanomas symptoms can happen anywhere on the body. Melanomas most often develop in areas that have had exposure to the sun. This includes the arms, back, face and legs.
Melanomas also can happen in areas that aren't as exposed to the sun. This includes the soles of the feet, palms of the hands and fingernail beds. Melanoma also can happen inside the body. These hidden melanomas are more common in people with brown or Black skin.
Typical moles
Typical moles are generally a uniform color. They might look pink, tan, brown or black. In people with brown and Black skin, typical moles are more likely to be dark brown or black. Typical moles have a distinct border separating the mole from the surrounding skin. They're oval or round and usually smaller than 1/4 inch (about 6 millimeters) in diameter.
Most moles begin appearing in childhood and new moles may form until about age 40. By the time they are adults, most people have between 10 and 40 moles. Moles may change in appearance over time and some may even go away with age.
Signs that may indicate melanoma
Some moles aren't typical. They may have certain characteristics that indicate melanomas or other skin cancers. Characteristics may include:
- Asymmetrical shape. Look for moles with unusual shapes, such as two very different-looking halves.
- Changes in color. Look for growths that have many colors or unusual color patterns.
- Changes in size. Look for new growth in a mole larger than 1/4 inch (about 6 millimeters).
- Changes in symptoms. Look for changes in symptoms, such as new itchiness or bleeding.
- Unusual border. Look for moles with unusual, notched or scalloped borders.
Moles that become cancers can all look very different. Some may show all of the changes listed above, while others may have only one or two unusual characteristics.
Hidden melanomas
Melanomas also can develop in areas of the body that have little or no exposure to the sun. These areas may include the spaces between the toes and on the palms, soles, scalp or genitals. These are sometimes referred to as hidden melanomas because they occur in places most people wouldn't think to check. When melanoma occurs in people with brown or Black skin, it's more likely to occur in a hidden area.
Hidden melanomas include:
- Melanoma inside the body. Mucosal melanoma develops in the mucous membrane. This tissue lines the nose, mouth, esophagus, anus, urinary tract and vagina. Mucosal melanomas are especially difficult to detect because they can easily be mistaken for other far more common conditions.
- Melanoma in the eye. Eye melanoma also is called ocular melanoma. It most often occurs in the layer of tissue beneath the white of the eye. This layer is called the uvea. An eye melanoma may cause vision changes and may be diagnosed during an eye exam.
- Melanoma under a nail. Acral-lentiginous melanoma is a rare form of melanoma that can occur under a fingernail or toenail. It also can be found on the palms of the hands or the soles of the feet. Acral-lentiginous melanoma tends to be very dark, flat and have very unusual borders. It's more common in people of Asian descent and people with brown or Black skin.
When to see a doctor
Make an appointment with your doctor or other healthcare professional if you notice any skin changes that worry you.
Causes
Where skin cancer develops
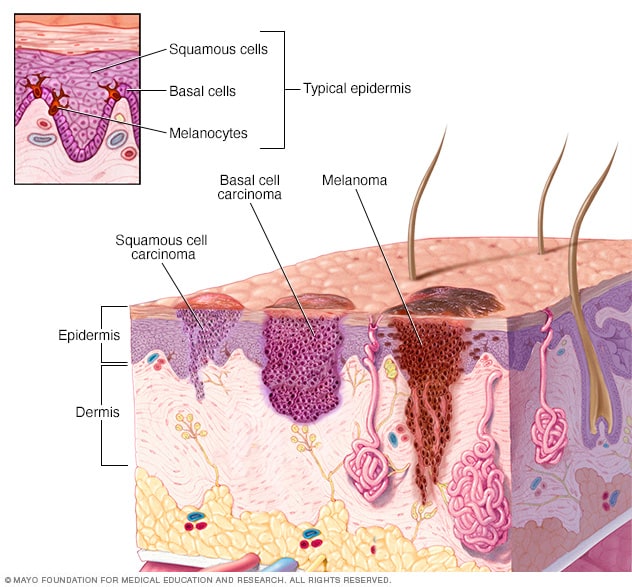
Where skin cancer develops
Skin cancer begins in the cells that make up the outer layer of the skin, called the epidermis. One type of skin cancer called basal cell carcinoma begins in the basal cells. Basal cells make skin cells that keep pushing older cells toward the surface. As new cells move up, they become squamous cells. Skin cancer that starts in the squamous cells is called squamous cell carcinoma of the skin. Melanoma, another type of skin cancer, happens in the pigment cells, called melanocytes.
Melanoma happens when something changes healthy melanocytes into cancer cells. Melanocytes are skin cells that make pigment that gives skin its color. The pigment is called melanin.
Melanoma starts when melanocytes develop changes in their DNA. A cell's DNA holds the instructions that tell a cell what to do. In healthy cells, DNA gives instructions to grow and multiply at a set rate. The instructions tell the cells to die at a set time. In cancer cells, the DNA changes give different instructions. The changes tell the cancer cells to make many more cells quickly. Cancer cells can keep living when healthy cells would die. This causes too many cells.
The cancer cells might form a mass called a tumor. The tumor can grow to invade and destroy healthy body tissue. In time, cancer cells can break away and spread to other parts of the body. When cancer spreads, it's called metastatic cancer.
It isn't clear what changes the DNA in skin cells and how it leads to melanoma. It's likely a combination of factors, including environmental and genetic factors. Still, healthcare professionals believe exposure to ultraviolet light is the leading cause of melanoma. Ultraviolet light, also called UV light, comes from the sun and from tanning lamps and beds.
UV light doesn't cause all melanomas, especially those that occur in places on your body that don't receive exposure to sunlight. This means that other factors may contribute to your risk of melanoma.
Risk factors
Factors that may increase the risk of melanoma include:
- A family history of melanoma. If a close relative has had melanoma, you have a greater chance of developing a melanoma, too. Close relatives may include a parent, child or sibling.
- A history of sunburn. One or more severe, blistering sunburns can increase your risk of melanoma.
- Exposure to UV light. The ultraviolet light, also called UV light, that comes from the sun and from tanning lights and beds increases the risk of skin cancer, including melanoma.
- Having many moles or moles that aren't typical. Having more than 50 typical moles on your body indicates an increased risk of melanoma. Also, having a type of mole that isn't typical increases the risk of melanoma. Known medically as dysplastic nevi, these moles tend to be larger than typical moles. They may have unusual borders and a mixture of colors.
- Living closer to the equator or at a higher elevation. People living closer to the earth's equator experience more direct sun rays. Therefore, they experience higher amounts of UV light from the sun than people living farther north or south. Also, people who live at a higher elevation are more exposed to UV light.
- Skin that sunburns easily. Anyone can get melanoma, but it's most common in people with white skin. If you have blond or red hair, light-colored eyes, and freckle or sunburn easily, you're more likely to develop melanoma.
- Weakened immune system. If the body's germ-fighting immune system is weakened by medications or illness, there might be a higher risk of melanoma and other skin cancers. People with a weakened immune system include those taking medicines to control the immune system, such as after an organ transplant. Certain medical conditions, such as infection with HIV, can weaken the immune system.
Prevention
You can reduce your risk of melanoma and other types of skin cancer if you:
- Avoid tanning lamps and beds. Tanning lamps and beds give off ultraviolet light, also called UV light. Exposure to this kind of light can increase your risk of skin cancer.
- Avoid the sun during the middle of the day. For many people in North America, the sun's rays are strongest between about 10 a.m. and 4 p.m. Schedule outdoor activities for other times of the day, even in winter or when the sky is cloudy.
-
Become familiar with your skin so that you'll notice changes. Check your skin often for new skin growths. Look for changes in existing moles, freckles, bumps and birthmarks. With the help of mirrors, check your face, neck, ears and scalp.
Look at your chest and trunk and the tops and undersides of your arms and hands. Check both the front and back of your legs and your feet, including the soles and the spaces between your toes. Also check your genital area and between your buttocks.
-
Wear protective clothing. When you go outside during the day, wear clothes that help protect your skin from the sun's rays. Cover your skin with dark, tightly woven clothing that covers your arms and legs. Wear a broad-brimmed hat, which provides more protection than does a baseball cap or visor. Some companies also sell protective clothing. A dermatologist can recommend an appropriate brand.
Don't forget sunglasses. Look for those that block both types of UV light that come from the sun, called UVA and UVB.
- Wear sunscreen year-round. Use a broad-spectrum sunscreen with an SPF of at least 30, even on cloudy days. Apply sunscreen generously. Reapply every two hours, or more often if you're swimming or sweating.
Dec. 30, 2023