Overview
Advanced pyoderma gangrenosum
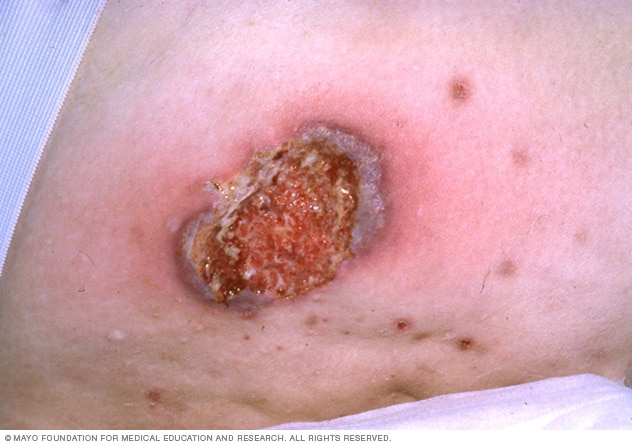
Advanced pyoderma gangrenosum
Pyoderma gangrenosum can cause painful, open sores that have blue or purple edges.
Pyoderma gangrenosum (pie-o-DUR-muh gang-ruh-NO-sum) is a rare condition that causes large, painful sores on the skin. The sores can develop quickly. Most often they appear on the legs.
The exact causes of pyoderma gangrenosum are unknown, but it appears to be a disorder of the immune system. People who have certain other conditions are at higher risk of pyoderma gangrenosum.
The condition usually clears up with treatment. But the sores often leave scars and can show up in new spots.
Products & Services
Symptoms
Pyoderma gangrenosum usually starts with a small bump on the skin. It might look like a spider bite. Within days it can turn into a large and painful open sore.
The sore usually appears on the legs but may develop anywhere on the body. Sometimes it appears around surgical sites. If you have two or more sores, they may grow and merge into one.
When to see a doctor
Talk with a healthcare professional if you develop a painful, rapidly growing skin wound.
Causes
No one knows the exact cause of pyoderma gangrenosum. It's often seen in people who have autoimmune diseases, such as ulcerative colitis, Crohn's disease and arthritis. And some studies suggest that it may be passed down through families.
If you have pyoderma gangrenosum, getting a cut or other skin wound can bring on new sores. The condition isn't an infection and it isn't contagious.
Risk factors
Certain factors may increase your risk of pyoderma gangrenosum, including:
- Being a woman between 20 and 50 years of age.
- Having an inflammatory bowel disease, such as ulcerative colitis or Crohn's disease.
- Having rheumatoid arthritis.
- Having a blood disorder, such as acute myelogenous leukemia or myelodysplasia.
Complications
Possible complications of pyoderma gangrenosum include infection, uncontrolled pain, scarring and and changes in skin color after the affected skin heals. This change in skin color is called postinflammatory hyperpigmentation when the skin darkens and postinflammatory hypopigmentation when the skin loses color. People with brown or Black skin have a higher risk of long-term skin color changes.
Prevention
You can't prevent the first instance of pyoderma gangrenosum. If you have the condition, you can help prevent new sores by protecting your skin from injury. Injury or trauma to the skin, including from surgery, can cause new sores to form.
It also may help to control any other condition you have that's related to pyoderma gangrenosum.
Dec. 05, 2024