AV node ablation
AV node ablation is a treatment for an irregular and often very rapid heartbeat called atrial fibrillation (AFib). The treatment uses heat energy, called radiofrequency energy, to destroy a small amount of tissue between the upper and lower chambers of the heart. This area is called the atrioventricular node, also called the AV node.
If you have AV node ablation, you need a permanent device called a pacemaker. The device is placed under the skin by the collarbone. It prevents the heart from beating too slowly.
Why it's done
AV node ablation may be done if you have atrial fibrillation (AFib) that doesn't get better with medicine or other treatments. It's generally considered the last treatment option for AFib because it requires the placement of a pacemaker.
What you can expect
Before the procedure
AV node ablation
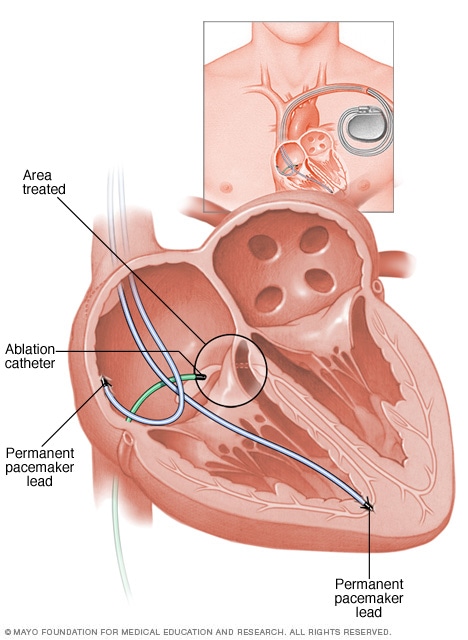
AV node ablation
Atrioventricular (AV) node ablation uses heat energy, called radiofrequency energy, to destroy the area between the upper and lower heart chambers. This area is called the AV node. The heart's electrical signals can't pass through the damaged area. So this treatment blocks the faulty heart signals that cause atrial fibrillation (AFib). Once the AV node is destroyed, a pacemaker is needed to control the heart rhythm.
Before AV node ablation, several tests are done to check your heart health.
Anyone who has AV node ablation needs a pacemaker for life to help the heart beat correctly. It's placed under the skin by the collarbone. You might have this device placed several weeks before AV node ablation to make sure it works well. But some people receive the pacemaker the day of the ablation.
During the procedure
Cardiac ablation is done in the hospital. A member of your care team places an IV into your forearm or hand. You get medicine to help you relax.
During the procedure, you may be awake or lightly sedated. Some people get a combination of medicines to put them in a sleep-like state. This is called general anesthesia. The type of sedation you receive depends on your type of irregular heartbeat and overall health.
The doctor inserts a thin, flexible tube called a catheter through a blood vessel, usually in your groin. The doctor guides the tube to the area of the heart being treated.
Sensors on the tip of the catheter apply heat to the heart tissue at the AV node. The heat energy is called radiofrequency energy. It damages the tissue, which destroys the heart's signaling connection causing irregular heartbeats.
Once the AV node is destroyed, your doctor places a pacemaker under the skin near your collarbone, unless you already have one. The device helps the heart beat properly.
After
After AV node ablation, you usually are taken to a recovery area where your care team closely checks on you. Depending on your condition, you may go home the same day or you may spend at least a night in the hospital.
Results
After AV node ablation, atrial fibrillation (AFib) symptoms and quality of life often improve. You may need to take blood-thinning medicines to reduce your risk of stroke.