Overview
Sudden cardiac arrest (SCA) is the sudden loss of all heart activity due to an irregular heart rhythm. Breathing stops. The person becomes unconscious. Without immediate treatment, sudden cardiac arrest can lead to death.
Emergency treatment for sudden cardiac arrest includes cardiopulmonary resuscitation (CPR) and shocks to the heart with a device called an automated external defibrillator (AED). Survival is possible with fast, appropriate medical care.
Sudden cardiac arrest isn't the same as a heart attack. A heart attack happens when blood flow to a part of the heart is blocked. Sudden cardiac arrest is not due to a blockage. However, a heart attack can cause a change in the heart's electrical activity that leads to sudden cardiac arrest.
Symptoms
Symptoms of sudden cardiac arrest are immediate and severe and include:
- Sudden collapse.
- No pulse.
- No breathing.
- Loss of consciousness.
Sometimes other symptoms occur before sudden cardiac arrest. These might include:
- Chest discomfort.
- Shortness of breath.
- Weakness.
- Fast-beating, fluttering or pounding heartbeat called palpitations.
But sudden cardiac arrest often occurs with no warning.
When to see a doctor
When the heart stops, the lack of oxygen-rich blood can quickly cause death or permanent brain damage.
Call 911 or emergency medical services for these symptoms:
- Chest pain or discomfort.
- Feeling of a pounding heartbeat.
- Rapid or irregular heartbeats.
- Unexplained wheezing.
- Shortness of breath.
- Fainting or near fainting.
- Lightheadedness or dizziness.
If you see someone who's unconscious and not breathing, call 911 or local emergency services. Then start CPR. The American Heart Association recommends doing CPR with hard and fast chest compressions. Use an automated external defibrillator, called an AED, if one is available.
How to do CPR
Do CPR if the person isn't breathing. Push hard and fast on the person's chest — about 100 to 120 pushes a minute. The pushes are called compressions. If you've been trained in CPR, check the person's airway. Then deliver rescue breaths after every 30 compressions.
If you haven't been trained, just continue chest compressions. Allow the chest to rise completely between each push. Keep doing this until an AED is available or emergency workers arrive.
Portable automated external defibrillators, called AEDs, are available in many public places, including airports and shopping malls. You also can buy one for home use. AEDs come with voice instructions for their use. They're programmed to allow a shock only when appropriate.
Causes
A change in the heart's electrical activity causes sudden cardiac arrest. The change makes the heart stop pumping blood. No blood flow goes to the body.
How the heart beats
Chambers and valves of the heart
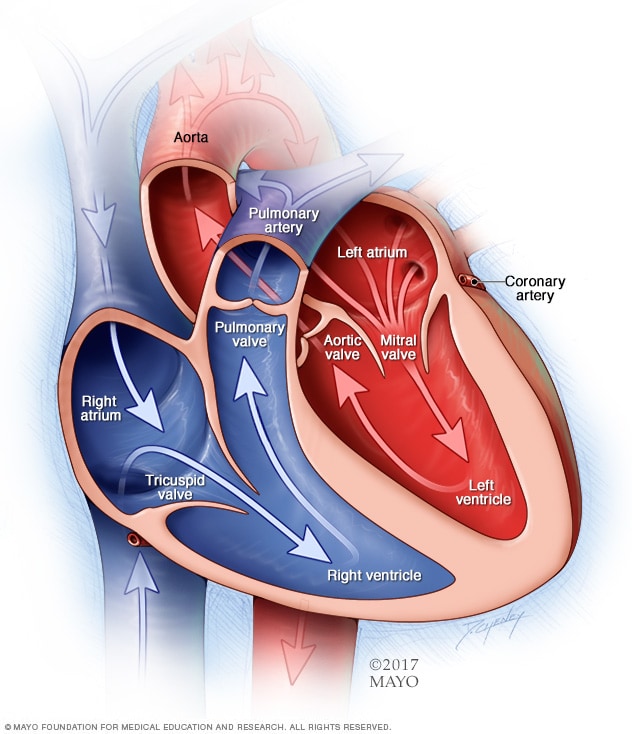
Chambers and valves of the heart
A typical heart has two upper and two lower chambers. The upper chambers, the right and left atria, receive incoming blood. The lower chambers, the more muscular right and left ventricles, pump blood out of the heart. The heart valves, which keep blood flowing in the right direction, are gates at the chamber openings.
To understand sudden cardiac arrest, it may help to know more about the heart's signaling system.
Electric signals in the heart control the rate and rhythm of the heartbeat. Faulty or extra electrical signals can make the heart beat too fast, too slowly or in an uncoordinated way. Changes in the heartbeat are called arrhythmias. Some arrhythmias are brief and harmless. Others can lead to sudden cardiac arrest.
Heart conditions that can lead to sudden cardiac arrest
The most common cause of sudden cardiac arrest is an irregular heart rhythm called ventricular fibrillation. Rapid, erratic heart signals cause the lower heart chambers to quiver uselessly instead of pumping blood. Some heart conditions can make you more likely to have this type of irregular heartbeat.
However, sudden cardiac arrest can happen in people who have no known heart disease.
Heart conditions that can cause sudden cardiac arrest include:
- Coronary artery disease. Sudden cardiac arrest may occur if the heart arteries become clogged with cholesterol and other deposits, reducing blood flow to the heart.
- Heart attack. If a heart attack occurs, often as a result of severe coronary artery disease, it can trigger ventricular fibrillation and sudden cardiac arrest. Also, a heart attack can leave scar tissue in the heart. The scar tissue can cause changes in the heartbeat.
- Enlarged heart called cardiomyopathy. This condition usually happens when the walls in the heart muscle stretch. The heart muscle gets bigger or thicker.
- Heart valve disease. Leaking or narrowing of the heart valves can lead to stretching or thickening of the heart muscle. When the chambers get larger or weak because of stress caused by a tight or leaking valve, there's an increased risk of developing an irregular heartbeat.
- Heart condition present at birth, called a congenital heart defect. Sudden cardiac arrest in children or adolescents is often due to a heart condition that they're born with. Adults who've had repair surgery for a congenital heart defect also have an increased risk of sudden cardiac arrest.
- Long QT syndrome (LQTS) and other heart signaling conditions. Conditions such as long QT syndrome and Brugada syndrome cause the heart to beat in an unorganized way. If the heart rhythm isn't quickly restored, sudden death can occur. Young people with LQTS are especially at risk of sudden death.
Risk factors
The same things that increase the risk of heart disease can raise the risk of sudden cardiac arrest. These include:
- A family history of coronary artery disease.
- Smoking.
- High blood pressure.
- High blood cholesterol.
- Obesity.
- Diabetes.
- An inactive lifestyle.
Other things that might increase the risk of sudden cardiac arrest include:
- A previous episode of sudden cardiac arrest or a family history of it.
- A previous heart attack.
- A personal or family history of other forms of heart disease such as heart rhythm disease, heart failure and heart conditions present at birth.
- Growing older.
- Being male.
- Using illicit drugs such as cocaine or amphetamines.
- Low potassium or magnesium levels.
- A sleep disorder called obstructive sleep apnea.
- Chronic kidney disease.
Complications
When sudden cardiac arrest occurs, less blood flows to the brain. If the heart rhythm isn't rapidly restored, complications may include brain damage and death.
Prevention
Keeping the heart healthy may help prevent sudden cardiac arrest. Take these steps:
- Eat healthy.
- Stay active and get regular exercise.
- Do not smoke or use tobacco.
- Have regular checkups.
- Get screened for heart disease.
- Control blood pressure and cholesterol.
Genetic tests can be done to see if you have long QT syndrome, a common cause of sudden cardiac death. Check with your insurer to see if it is covered. If you have the long QT gene, your healthcare professional may recommend that other family members also be tested.
If you have a known risk of cardiac arrest, your healthcare professional might recommend a heart device called an implantable cardioverter-defibrillator (ICD). The device is placed under your collarbone.
You also might consider purchasing an automated external defibrillator (AED) for home use. Discuss this with your healthcare team. AEDs help reset the heart's rhythm when a person has sudden cardiac arrest. But they can be expensive and aren't always covered by health insurance.
Dec. 07, 2024