Overview
A nuclear stress test is an imaging test that shows how blood goes to the heart at rest and during exercise. It uses a small amount of radioactive material, called a tracer or radiotracer. The substance is given through a vein. An imaging machine takes pictures of how the tracer moves through the heart arteries. This helps find areas of poor blood flow or damage in the heart.
A nuclear stress test is one of several types of stress tests. It may be done after a regular exercise stress test. Sometimes it is the first stress test used. If you have coronary artery disease, a nuclear stress test can help your healthcare team learn your risk of a heart attack or other heart event.
The test uses a positron emission technology (PET) scanner or single-photon emission computed tomography (SPECT) scanner.
Other names for a nuclear stress test are:
- Cardiac PET study.
- Cardiac SPECT study.
- Myocardial perfusion imaging (MPI) study.
Products & Services
Why it's done
This test may be done if you are being treated for heart disease or you have symptoms such as chest pain or shortness of breath.
A nuclear stress test is often done to:
- Diagnose coronary artery disease. The coronary arteries are the major blood vessels that supply the heart with blood, oxygen and nutrients. Coronary artery disease happens when these arteries are damaged or diseased. A nuclear stress test can diagnose coronary artery disease and show how severe the condition is.
- Create a treatment plan. If you have coronary artery disease, a nuclear stress test can tell your healthcare team how well treatment is working. The test also shows how much exercise your heart can handle. This information helps your healthcare team choose the best treatment for you.
More Information
Risks
A nuclear stress test is generally safe. Complications are rare, but there is some risk. Complications might include:
- Irregular heartbeats, also called arrhythmias. Those that occur during a stress test usually go away shortly after exercising ends or the medicine wears off. Life-threatening ones are rare.
- Low blood pressure. Blood pressure may drop during or right after exercise. This might cause dizziness or fainting. The problem generally goes away after the exercise ends.
- Heart attack. Although extremely rare, it's possible that a nuclear stress test could cause a heart attack.
Some people may have other symptoms during the test, including:
- Anxiety.
- Flushing.
- Headache.
- Nausea.
- Shakiness.
- Shortness of breath.
These symptoms are usually mild and go away quickly. Tell your healthcare team if you have any of these symptoms during a nuclear stress test.
How you prepare
Your healthcare professional tells you how to prepare for your nuclear stress test.
Food and medications
You may be asked not to eat, drink or smoke for a time before a nuclear stress test. You may need to avoid caffeine the day before and the day of the test.
Ask your healthcare team if you need to stop taking any medicines before the test. Some medicines can interfere with some test results. Never change or stop your medicines without first talking with your healthcare professional.
If you use an inhaler for asthma or other breathing difficulties, bring it to the test. Make sure your healthcare professional knows that you use one.
Clothing and personal items
Wear or bring comfortable clothes and walking shoes. Don't apply oil, lotion or cream to your skin on the day of your nuclear stress test.
What you can expect
A nuclear stress test uses a substance called a radioactive tracer. It's given by IV. Then the healthcare professional takes two sets of pictures of the heart — one at rest and another after exercise.
A nuclear stress test can take two or more hours. It depends on the radioactive tracer and imaging tests used.
Before
Before you have a nuclear stress tests, your healthcare professional asks questions about your medical history and how often and actively you exercise. This helps set safe limits for your exercise. Your healthcare professional also listens to your heart and lungs for anything that might affect your test results.
During
Exercise stress test
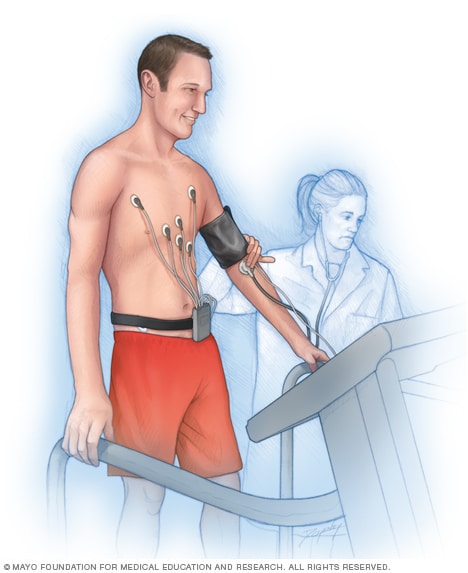
Exercise stress test
In an exercise stress test, sensors called electrodes are placed on the chest and sometimes the arms and legs. The sensors record information about the heartbeat. A healthcare professional checks the heart while the person walks on a treadmill or pedals a stationary bike.
During a nuclear stress test:
- A cuff on your arm measures your blood pressure.
- Sticky patches on your chest, and sometimes your legs and arms, record your heartbeat.
A healthcare professional inserts a needle into one of your veins in your arm, called an IV, and injects a substance called a radiotracer. The substance also is called a radiopharmaceutical.
The substance may feel cold when it goes into your arm. It takes a few minutes for your heart cells to absorb it. Then you lie still on a table. The healthcare professional takes the first set of images of your heart.
The next part of the test often involves walking on a treadmill or riding a stationary bike. If you can't exercise, you might get medicine that increases blood flow to the heart, just as exercise does.
When your heart rate peaks from exercising, the healthcare professional gives more radiotracer thru the IV. Then the second set of images of your heart are taken. On the images, the radiotracer lights up areas of the heart that don't get enough blood flow.
You may be asked to breathe into a tube during the test. This helps determine how well you breathe during exercise.
You can stop exercising anytime you're too uncomfortable. Usually, you keep exercising until your heart rate reaches a specific goal or you get concerning symptoms. These symptoms might include:
- An irregular heartbeat or other changes in your heartbeat.
- Dizziness.
- Moderate to severe chest pain.
- Severe shortness of breath.
- Unusually high or low blood pressure.
After
After the exercise is done, you might be asked to stand still for a few seconds and then lie down for a short while. Your healthcare professional continues to watch your heartbeat and breathing during this time.
After the test you can usually return to your usual activities unless your healthcare team tells you not to do so.
The radioactive tracer leaves the body in the urine or stool. Drink plenty of water to help flush it out of your system.
Results
Your healthcare professional compares the two sets of pictures taken during your nuclear stress test. The pictures show how blood flows through your heart while at rest and during physical activity.
Your healthcare professional talks with you about your test results. The results could show:
- Typical blood flow during exercise and rest. You might not need any more tests.
- Typical blood flow during rest, but not during exercise. Part of the heart doesn't get enough blood during exercise. This might mean there are one or more blocked arteries, which is coronary artery disease.
- Low blood flow during rest and exercise. Part of the heart doesn't get enough blood at all times. This could be due to severe coronary artery disease or an earlier heart attack.
- Lack of blood flow in parts of the heart. Areas of the heart that don't show the radioactive tracer have damage from a heart attack.
If you don't have enough blood flow through your heart, you may need a test called coronary angiography. This test helps show any blockages in the heart arteries.
If you have a severe blockage in a heart artery, you may need a heart treatment called angioplasty with stenting. Or you might need coronary artery bypass graft surgery, also called CABG. CABG is a type of open-heart surgery that creates a new path for blood to flow around a blockage.
Dec. 03, 2024