Overview
Hidradenitis suppurativa
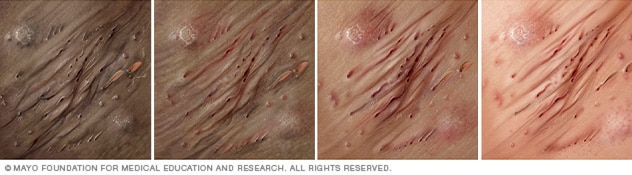
Hidradenitis suppurativa
Illustration of hidradenitis suppurativa on different skin colors. This condition usually appears as one or more tender bumps that fill with pus. It often occurs in the armpits.
Hidradenitis suppurativa (hi-drad-uh-NIE-tis sup-yoo-ruh-TIE-vuh), also known as acne inversa, is a condition that causes small, painful lumps to form under the skin. The lumps usually develop in areas where your skin rubs together, such as the armpits, groin, buttocks and breasts. The lumps heal slowly, recur, and can lead to tunnels under the skin and scarring.
Hidradenitis suppurativa tends to start after puberty, usually before age 40. It can persist for many years and worsen over time. It can affect your daily life and emotional well-being. Combined medical and surgical therapy can help manage the disease and prevent complications.
Women are three times more likely to develop hidradenitis suppurativa, though this ratio can differ by location around the world. Also, Black people are more likely to develop this disease than people of other races. This could be attributed to genetic factors.
Products & Services
Symptoms
Hidradenitis suppurativa can affect one or several areas of the body. Signs and symptoms of the condition include:
- Blackheads. Blackheads appear in small, pitted areas of skin, often appearing in pairs.
- Painful pea-sized lumps. The condition usually starts with a single, painful lump under the skin that persists for weeks or months. More bumps may form later, usually in areas where you have more sweat and oil glands or where the skin rubs together, such as the armpits, groin, buttocks and breasts.
- Leaking bumps or sores. Some bumps or sores get bigger, break open and drain pus with an odor.
- Tunnels. Over time, tunnels might form under the skin, connecting the lumps. These wounds heal slowly, if at all, and drain blood and pus.
Some people with this condition experience only mild symptoms. The course of the disease is highly variable. Excess weight and being a smoker are associated with worse symptoms, but people who are thin and don't smoke can experience severe disease.
When to see a doctor
Early diagnosis of hidradenitis suppurativa is key to effective treatment. See your dermatologist if your condition:
- Is painful.
- Makes it difficult to move.
- Doesn't improve in a few weeks.
- Returns within weeks of treatment.
- Appears in several locations.
- Flares often.
Your dermatologist can create a treatment plan for you.
Hidradenitis suppurativa is not just a boil, and many people with this condition also have related conditions. People with hidradenitis suppurativa benefit from a health care team with medical and surgical dermatologists at the core. Other specialists are involved as needed.
Causes
Hidradenitis suppurativa develops when hair follicles become blocked, but why this blockage occurs isn't known. Experts think it could be connected to hormones, genetic predisposition, cigarette smoking or excess weight.
An infection or being unclean does not cause hidradenitis suppurativa, and it can't be spread to other people.
Risk factors
Factors that increase your chance of developing hidradenitis suppurativa include:
- Age. The risk of hidradenitis suppurativa is higher for people in their teens and 20s.
- Sex. Females are more likely to develop hidradenitis suppurativa than males.
- Race. Ethnicity or race might affect risk level. The condition occurs most in Black people, possibly due to genetic factors.
- Family history. A tendency to develop hidradenitis suppurativa can be inherited.
- Certain conditions. Hidradenitis suppurativa is more common and severe in people who are overweight. It also has an association with severe acne, arthritis, diabetes, metabolic syndrome and inflammatory bowel disease.
- Smoking. Smoking tobacco has been linked to hidradenitis suppurativa.
Complications
Persistent and severe hidradenitis suppurativa can cause complications, including:
- Infection. Secondary infection is possible in the affected area, but the presence of pus is common in hidradenitis suppurativa and doesn't necessarily mean infection.
- Scars and skin changes. The wounds may heal but leave ropelike scars or pitted skin.
- Restricted movement. Sores and scar tissue can cause limited or painful movement, especially when the disease affects the armpits or thighs.
- Skin cancer. Squamous cell carcinoma has been reported with long-term hidradenitis suppurativa, particularly in people whose condition involves the perianal area. This area consists of the tissues around the anus.
- Swelling in the arms, legs or genitals. The most common sites for hidradenitis suppurativa also contain many lymph nodes. Scar tissue can interfere with the lymph drainage system, which can cause the arms, legs or genitals to swell.
- Psychological effects and social isolation. The location, drainage and odor of the sores can cause embarrassment and reluctance to go out in public, leading to anxiety or depression.
- Lifelong pain. This pain is much worse than diseases such as psoriasis.