Diagnosis
To diagnose a brain arteriovenous malformation (AVM), your healthcare professional reviews your symptoms and conducts a physical exam.
One or more tests may be used to diagnose brain AVM. Imaging tests are usually done by radiologists trained in brain and nervous system imaging, known as neuroradiologists.
 Neurology consultation at Mayo Clinic
Neurology consultation at Mayo Clinic
Brain AVM angiogram
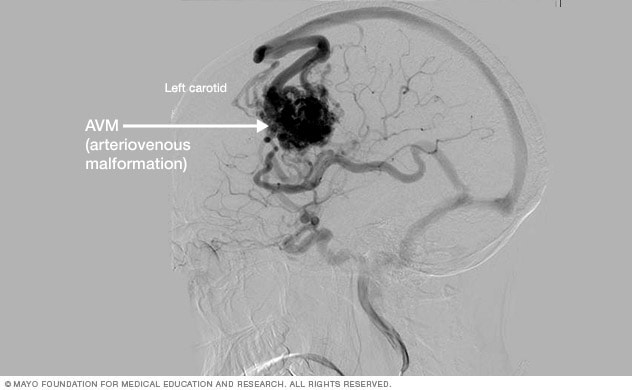
Brain AVM angiogram
This cerebral angiogram shows a brain AVM.
CT scan
CT scan
A CT scan can be used to visualize nearly all parts of the body. It is used to diagnose disease or injury as well as to plan medical, surgical or radiation treatment.
Brain MRI scan
Tests used to diagnose brain AVMs include:
-
Cerebral angiography. This is the most detailed test to diagnose a brain AVM. Cerebral angiography reveals the location of the feeding arteries and draining veins, which is critical to planning treatment. Cerebral angiography is also known as cerebral arteriography.
In this test, a long, thin tube called a catheter is inserted into an artery in the groin or wrist. The catheter is threaded to the brain using X-ray imaging. A dye is injected into the blood vessels of the brain to make them visible under X-ray imaging.
-
Computerized tomography (CT) scan. A CT scan uses a series of X-rays to create a detailed cross-sectional image of the brain.
Sometimes a dye is injected through a tube into a vein for the CT scan. This type of test is known as computerized tomography angiography. The dye allows the arteries feeding the AVM and the veins draining the AVM to be viewed in greater detail.
-
Magnetic resonance imaging (MRI). MRI uses powerful magnets and radio waves to create detailed images of the brain.
MRI is more sensitive than CT and can show subtle changes in brain tissue related to a brain AVM.
MRI also provides information about the exact location of the brain AVM and any related bleeding in the brain. The information is important for planning treatment.
A dye also may be injected to see the blood circulation in the brain. This type of test is known as magnetic resonance angiography.
More Information
Treatment
Endovascular embolization
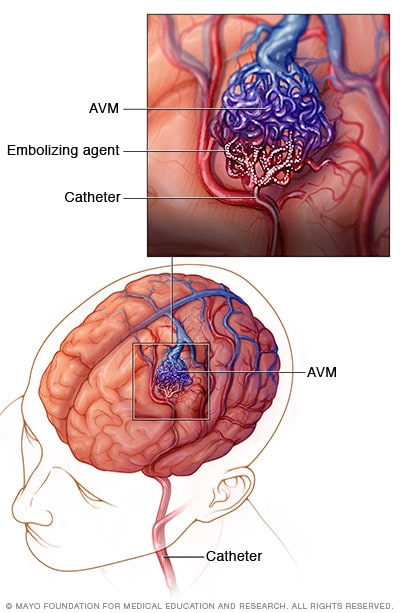
Endovascular embolization
In endovascular embolization, a long, thin tube called a catheter is inserted into a leg artery. The catheter is threaded through blood vessels to the brain using X-ray imaging. The surgeon positions the catheter in one of the arteries that feeds the AVM. An embolizing agent, such as small particles or a gluelike substance, is injected. The embolizing agent blocks the artery and reduces blood flow into the AVM.
Close-up of endovascular embolization
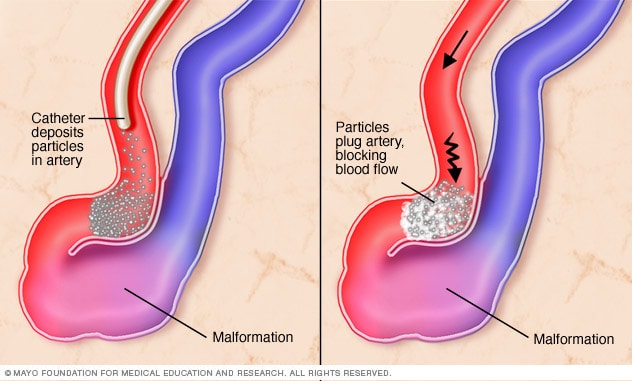
Close-up of endovascular embolization
In endovascular embolization for brain AVM, a catheter deposits particles or a gluelike substance in the affected artery to block blood flow.
Gamma Knife targeting
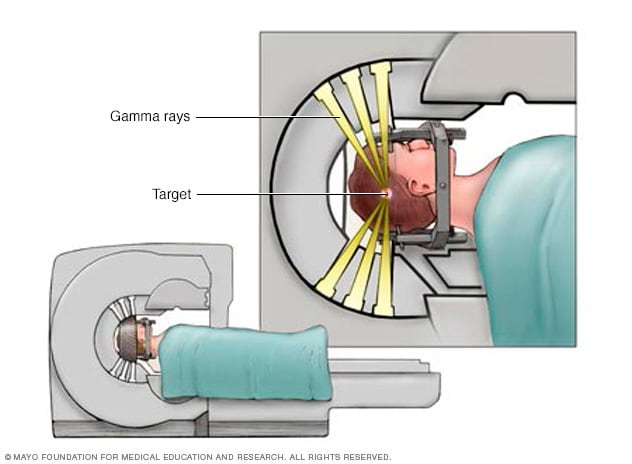
Gamma Knife targeting
Individual radiation beams are too weak to hurt the brain tissue they travel through on the way to the target. The radiation is most powerful where all the beams intersect.
There are several treatments for brain arteriovenous malformation (AVM). The main goal of treatment is to prevent bleeding, known as a hemorrhage. Treatment also can help control seizures or other brain symptoms.
The proper treatment depends on your age, health, and the size and location of the brain AVM.
Medicines may be used to treat symptoms caused by the AVM, such as headaches or seizures.
Treatment depends on the AVM and your health. Your care team may recommend surgery if the AVM has bled and surgery is likely to be safe for you. There are three surgical options:
-
Surgical removal, known as resection. Surgery may be recommended if the brain AVM has bled or is in an area that can easily be reached. In this procedure, the surgeon removes part of the skull to gain access to the AVM.
With the help of a high-powered microscope, the surgeon seals off the AVM with special clips and carefully removes it from surrounding brain tissue. The surgeon then reattaches the skull bone and closes the incision in the scalp.
Resection usually is done when the AVM can be removed with little risk of hemorrhage or seizure. AVMs that are in deep brain regions carry a higher risk of complications, and other treatments may be recommended.
-
Endovascular embolization. In this procedure, a catheter is inserted into an artery in the leg or wrist. The catheter is threaded through blood vessels to the brain using X-ray imaging.
The catheter is positioned in one of the arteries that feeds the brain AVM. The surgeon injects an embolizing agent. This may be small particles, a gluelike substance, microcoils or other materials. The embolizing agent blocks the artery and reduces blood flow into the AVM.
Endovascular embolization is less invasive than traditional surgery. It may be performed alone but it's often used before other surgical treatments to make them safer. It does this by reducing the size of the brain AVM or the likelihood of bleeding.
In some large brain AVMs, endovascular embolization may be used to reduce stroke-like symptoms by redirecting blood back to brain tissue.
-
Stereotactic radiosurgery (SRS). This treatment uses precisely focused radiation to destroy the AVM. This type of surgery doesn't require cuts in the body the way other surgeries do.
Instead, SRS directs many highly targeted radiation beams at the AVM to damage the blood vessels and cause scarring. The scarred AVM blood vessels then slowly close in 1 to 3 years.
This treatment may be done for small AVMs that are hard to remove with traditional surgery. It also may be done for AVMs that haven't caused dangerous hemorrhages.
Sometimes healthcare professionals decide to monitor a brain AVM rather than treating it. This may be recommended if you have few or no symptoms or if your AVM is in an area of your brain that's hard to treat. Monitoring includes regular medical checkups with your healthcare team.
Potential future treatments
Researchers are studying ways to better predict the risk of hemorrhage in people with brain AVM. This can help better guide treatment decisions. This may include looking at AVM features seen on imaging and whether a person has an inherited condition linked to AVMs, such as hereditary hemorrhagic telangiectasia (HHT).
Researchers are studying new imaging tools that may help doctors plan treatment for brain AVMs. Examples include advanced MRI techniques and 3D models that can help visualize the AVM and nearby brain tissue. These could help improve surgical precision and safety in removing brain AVMs and preserving surrounding blood vessels.
Ongoing advances in embolization, radiosurgery and microsurgery techniques also are making it possible to use surgery to treat brain AVMs that were hard to access in the past. Advances also are making it safer to remove brain AVMs during surgery.
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Coping and support
You can take steps to cope with the emotions that may come with a diagnosis of brain arteriovenous malformation (AVM) and the recovery process. Consider trying to:
- Learn about brain AVM to make informed decisions about your care. Ask your healthcare professional about the size and location of your brain AVM. Ask how that affects your treatment options. As you learn more about brain AVMs, you may become more confident in making treatment decisions.
- Accept your emotions. Complications of brain AVM, such as hemorrhage and stroke, can cause emotional concerns as well as physical ones. Recognize that experiencing emotions is common. Some emotional and mood changes may be caused by the injury itself, along with coming to terms with the diagnosis.
- Keep friends and family close. Keeping your close relationships strong helps during recovery. Friends and family can provide the practical support you need, such as coming with you to healthcare appointments and providing emotional support.
- Find someone to talk with. Find a good listener who is willing to listen to you talk about your hopes and fears. This may be a friend or family member. The concern and understanding of a counselor, medical social worker, clergy member or support group also may be helpful.
Ask your healthcare professional about support groups in your area. You also might look online or check the library. You may find a support group through a national organization, such as the American Stroke Association or the Aneurysm and AVM Foundation.
Preparing for your appointment
A brain arteriovenous malformation (AVM) may be diagnosed in an emergency right after bleeding has occurred. It also may be found after other symptoms prompt a brain scan.
But sometimes a brain AVM may be found during the diagnosis or treatment of an unrelated medical condition. You may then be referred to a specialist trained in brain and nervous system conditions, such as a neurologist or neurosurgeon.
Because there's often a lot to discuss, it's a good idea to arrive prepared for your appointment. Here are some tips to help you get ready and what to expect from your healthcare professional.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance.
- Write down any symptoms you're experiencing, including any that don't seem related to the reason for which you scheduled the appointment.
- Make a list of all medicines, vitamins and supplements that you're taking.
- Ask a family member or friend to come with you, if possible. Sometimes it can be hard to remember all the information provided to you during an appointment. Someone who comes with you may remember something that you forgot or missed.
- Write down questions to ask. Also, don't be afraid to ask questions that may come up during your appointment.
Your appointment time is limited, so preparing a list of questions ahead of time helps make the most of your time. For brain AVM, some basic questions to ask include:
- What are other possible causes of my symptoms?
- What tests will I need to confirm the diagnosis?
- What are my treatment options and the pluses and minuses for each?
- What results can I expect?
- What kind of follow-up should I expect?
What to expect from your doctor
Your neurologist is likely to ask about any symptoms you may be experiencing, do a physical exam and schedule tests to confirm the diagnosis.
The tests gather information about the size and location of the AVM to help direct your treatment options. Your neurologist may ask:
- When did your symptoms start?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
What you can do in the meantime
Avoid any activity that may raise your blood pressure and put stress on a brain AVM, such as heavy lifting or straining. Also avoid taking any blood-thinning medicines, such as warfarin (Jantovin).