Overview
Aortic valve regurgitation
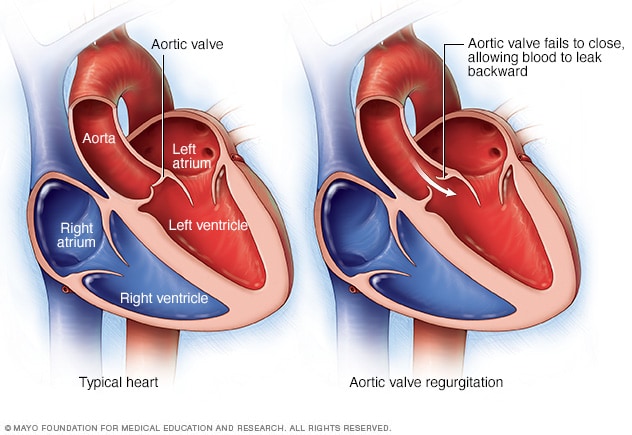
Aortic valve regurgitation
In aortic valve regurgitation, the aortic valve doesn't close as it should. This causes blood to flow backward from the body's main artery, called the aorta, into the lower left heart chamber, called the left ventricle.
Aortic valve regurgitation — also called aortic regurgitation — is a type of heart valve disease. The valve between the lower left heart chamber and the body's main artery doesn't close tightly. As a result, some of the blood pumped out of the heart's main pumping chamber, called the left ventricle, leaks backward.
The leakage may prevent the heart from doing a good enough job of pumping blood to the rest of the body. You may feel tired and short of breath.
Aortic valve regurgitation can develop suddenly or over many years. Once the condition becomes severe, surgery often is needed to repair or replace the valve.
Symptoms
Most often, aortic valve regurgitation develops over time. You may have no symptoms for years. You might not realize that you have the condition. But sometimes, aortic valve regurgitation happens suddenly. Usually, this is caused by an infection of the valve.
As aortic valve regurgitation becomes worse, symptoms may include:
- Shortness of breath with exercise or when lying down.
- Tiredness and weakness, especially when being more active than usual.
- Irregular heartbeat.
- Lightheaded feeling or fainting.
- Pain, discomfort or tightness in the chest that often gets worse during exercise.
- Feelings of a rapid, fluttering heartbeat, called palpitations.
- Swollen ankles and feet.
When to see a doctor
Call a member of your healthcare team right away if you have symptoms of aortic valve regurgitation.
Sometimes the first symptoms of aortic valve regurgitation are related to heart failure. Heart failure is a condition in which the heart can't pump blood as well as it should. Make an appointment with your healthcare team if you have:
- Tiredness, also called fatigue, that doesn't get better with rest.
- Shortness of breath.
- Swollen ankles and feet.
These are common symptoms of heart failure.
Causes
Chambers and valves of the heart
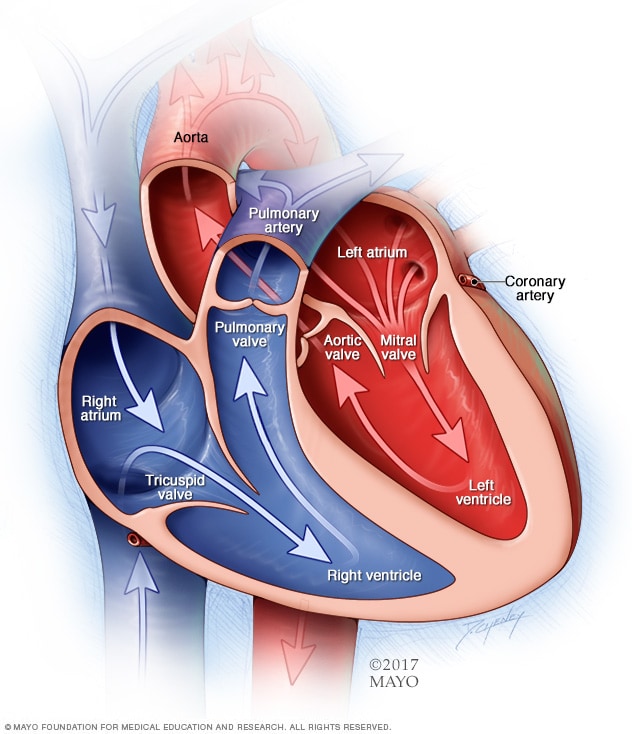
Chambers and valves of the heart
A typical heart has two upper and two lower chambers. The upper chambers, the right and left atria, receive incoming blood. The lower chambers, the more muscular right and left ventricles, pump blood out of the heart. The heart valves are gates at the chamber openings. They keep blood flowing in the right direction.
The aortic valve is one of four valves that control blood flow through the heart. It separates the heart's main pumping chamber, called the left ventricle, and the body's main artery, called the aorta. The aortic valve has flaps, also called cusps or leaflets, that open and close once during each heartbeat.
In aortic valve regurgitation, the valve doesn't close properly. This causes blood to leak back into the lower left heart chamber, called the left ventricle. As a result, the chamber holds more blood. This could cause it to get larger and thicken.
At first, the larger left ventricle helps maintain good blood flow with more force. But over time, the heart becomes weak.
Any condition that damages the aortic valve can cause aortic valve regurgitation. Causes may include:
-
Heart valve disease present at birth. Some people are born with an aortic valve that has only two cusps or with connected cusps, rather than the typical three separate ones. In either situation, the condition is called a bicuspid valve. Sometimes the valve may have only one cusp, called a unicuspid valve. Other times, there are four cusps, called a quadricuspid valve.
Having a parent or sibling with a bicuspid valve raises your risk of the condition. But you can have a bicuspid valve even if you don't have a family history of the condition.
- Narrowing of the aortic valve, called aortic stenosis. Calcium deposits can build up on the aortic valve as you age. The buildup causes the aortic valve to stiffen and become narrow. It prevents the valve from opening properly. Aortic stenosis also may prevent the valve from closing properly.
- Inflammation of the inner lining of the heart's chambers and valves. This life-threatening condition also is called endocarditis. It's usually caused by an infection. It can damage the aortic valve.
- Rheumatic fever. This condition was once a common childhood illness in the United States. Strep throat can cause it. Rheumatic fever can cause the aortic valve to become stiff and narrow. That in turn causes blood to leak. If you have an irregular heart valve due to rheumatic fever, it's called rheumatic heart disease.
- Other health conditions. Other rare conditions can cause the aorta to get bigger and damage the aortic valve. These include a connective tissue disease called Marfan syndrome that is present at birth. Some immune system conditions, such as lupus, also can lead to aortic valve regurgitation.
- Tear or injury of the body's main artery. The body's main artery is the aorta. A traumatic chest injury may damage the aorta and cause aortic regurgitation. So might a tear in the inner layer of the aorta, called an aortic dissection.
Risk factors
Things that raise the risk of aortic valve regurgitation include:
- Older age.
- Heart conditions present at birth, also called congenital heart defects.
- History of infections that can affect the heart.
- Some conditions passed down through families that can affect the heart, such as Marfan syndrome.
- Other types of heart valve disease, such as aortic valve stenosis.
- High blood pressure.
Aortic valve regurgitation also can happen without any known risk factors.
Complications
Complications of aortic valve regurgitation can include:
- Fainting or feeling lightheaded.
- Heart failure.
- Some heart infections, such as endocarditis.
- Heart rhythm conditions, called arrhythmias.
- Death.
Prevention
If you have any type of heart disease, get regular health checkups to help prevent complications.
If you have a parent, child or sibling with a bicuspid aortic valve, you should have an imaging test called an echocardiogram. This can check for bicuspid aortic valve or valve regurgitation. It's important for healthcare professionals to find heart valve disease, such as aortic valve regurgitation, as early as possible. Doing so may make the condition easier to treat.
Also, take steps to prevent conditions that can raise the risk of aortic valve regurgitation. For example:
- Get a health checkup if you have a severe sore throat. Strep throat that is not treated can lead to rheumatic fever. Strep throat is treated with medicines that fight bacteria, called antibiotics.
- Check your blood pressure regularly. Have your blood pressure checked at least every two years starting at age 18. Some people need more-frequent checks.