Overview
Addison's disease is a rare condition that happens when the body doesn't make enough of some hormones. Another name for Addison's disease is primary adrenal insufficiency. With Addison's disease, the adrenal glands make too little of the hormone cortisol. Often, they also make too little of another hormone called aldosterone.
Damage to the adrenal glands causes Addison's disease. Symptoms can start slowly. Early symptoms may include extreme tiredness, salt cravings and weight loss.
Addison's disease can affect anyone. Without treatment, it can be life-threatening. Treatment involves taking lab-made hormones to replace those that are missing.
Products & Services
Symptoms
Addison's disease symptoms usually happen slowly, often over months. The disease may happen so slowly that people who have it might ignore the symptoms at first. Physical stress such as an illness or injury can make symptoms get worse fast.
Early symptoms of Addison's disease can affect you in various ways. Some early symptoms can cause discomfort or loss of energy, including:
- Extreme tiredness, also called fatigue.
- Dizziness or fainting when standing after sitting or lying down. This is due to a type of low blood pressure called postural hypotension.
- Sweating due to low blood sugar, also called hypoglycemia.
- Upset stomach, diarrhea or vomiting.
- Pain in the stomach area, also called the abdomen.
- Muscle cramps, weakness, widespread pain or joint pain.
Other early symptoms can cause changes in how you look, such as:
- Body hair loss.
- Areas of darkened skin, especially on scars and moles. These changes may be harder to see on Black or brown skin.
- Weight loss due to less hunger.
Early Addison's disease symptoms also can affect emotions, mental health and desires. These symptoms include:
- Depression.
- Irritable mood.
- Lower sex drive in women.
- Salt craving.
Emergency symptoms due to adrenal crisis
Sometimes the symptoms of Addison's disease become worse fast. If this happens, it's an emergency known as an adrenal crisis. You also may hear it called an addisonian crisis or acute adrenal failure. Call 911 or your local emergency number if you have Addison's disease with any the following symptoms:
- Serious weakness.
- Sudden, terrible pain in the lower back, stomach area or legs.
- Severe upset stomach, vomiting or diarrhea.
- Extreme loss of body water, also called dehydration.
- Fever.
- Confusion or much less awareness of the surroundings.
- Loss of consciousness.
- Low blood pressure and fainting.
Without fast treatment, an adrenal crisis can lead to death.
When to see a doctor
See a healthcare professional if you have common symptoms of Addison's disease, such as:
- Long-lasting fatigue.
- Muscle weakness.
- Loss of appetite.
- Darkened areas of skin.
- Weight loss that doesn't happen on purpose.
- Serious upset stomach, vomiting or stomach pain.
- Lightheadedness or fainting with standing.
- Salt cravings.
Get emergency care right away if you have any symptoms of an adrenal crisis.
Causes
Adrenal glands
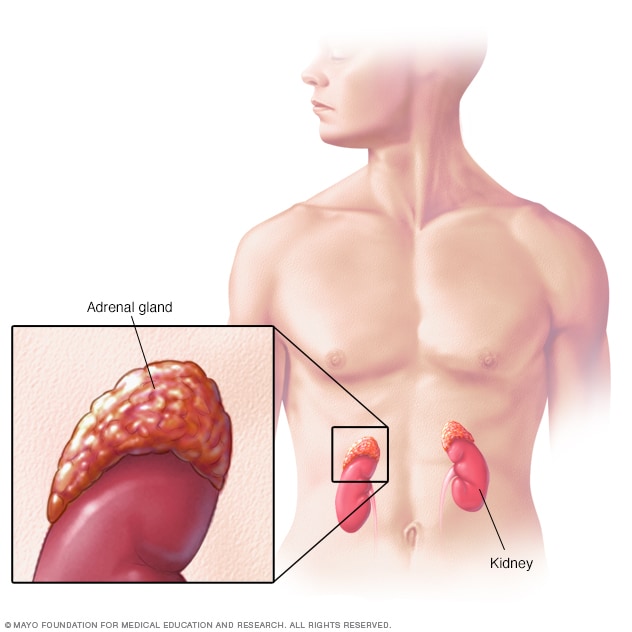
Adrenal glands
Located on top of the kidneys, the adrenal glands make hormones that help regulate metabolism, the immune system, blood pressure and other important functions. Although small, these glands control much of what happens in the body.
Damage to the adrenal glands causes Addison's disease. These glands sit just above the kidneys. The adrenal glands are part of the system of glands and organs that makes hormones, also called the endocrine system. The adrenal glands make hormones that affect almost every organ and tissue in the body.
The adrenal glands are made up of two layers. The inner layer, called the medulla, makes hormones such as adrenaline. Those hormones control the body's response to stress. The outer layer, called the cortex, makes a group of hormones called corticosteroids. Corticosteroids include:
- Glucocorticoids.These hormones include cortisol, and they affect the body's ability to turn food into energy. They also play a role in the immune system and help the body respond to stress.
- Mineralocorticoids. These hormones include aldosterone. They balance the body's sodium and potassium to keep blood pressure in a healthy range.
- Androgens. In all people, the adrenal glands make small amounts of these sex hormones. They cause male sexual development. And they affect muscle mass, body hair, sex drive, and a sense of well-being in all people.
Addison's disease also is known as primary adrenal insufficiency. A related condition is called secondary adrenal insufficiency. These conditions have different causes.
Addison's disease, also called primary adrenal insufficiency
This condition happens when the outer layer of the adrenal glands becomes damaged and can't make enough hormones. Most often, the damage is due to a disease in which the immune system attacks healthy tissues and organs by mistake. This is called an autoimmune disease. People with Addison's disease are more likely than are other people to have another autoimmune disease as well.
Other causes of Addison's disease can include:
- A serious infection called tuberculosis that mainly affects the lungs and also can destroy the adrenal glands.
- Other infections of the adrenal glands.
- Spread of cancer to the adrenal glands.
- Bleeding into the adrenal glands.
- A group of genetic conditions present at birth that affect the adrenal glands. This is called congenital adrenal hyperplasia.
- Medicines that block the body's ability to make glucocorticoid, such as ketoconazole (Ketozole), mitotane (Lysodren) and etomidate (Amidate). Or medicines that block the action of glucocorticoid in the body, such as mifepristone (Mifeprex, Korlym).
- Treatment for cancer with medicines called checkpoint inhibitors.
Secondary adrenal insufficiency
This type of adrenal insufficiency has many symptoms in common with Addison's disease. But it's more common than Addison's disease. Secondary adrenal insufficiency happens when the pituitary gland near the brain doesn't prompt the adrenal glands to make cortisol.
Typically, the pituitary gland makes a hormone called adrenocorticotropic hormone (ACTH). ACTH in turn causes the outer layer of the adrenal glands to make its hormones, including glucocorticoids and androgens. But with secondary adrenal insufficiency, too little ACTH causes the adrenal glands to make too little of these hormones.
Most symptoms of secondary adrenal insufficiency are like those of Addison's disease. But people with secondary adrenal insufficiency don't develop darkened skin. And they're less likely to have serious dehydration or low blood pressure. They're more likely to have low blood sugar.
Factors that can cause the pituitary gland to make too little ACTH include:
- Pituitary tumors that aren't cancer.
- Surgery or radiation therapy of the pituitary gland.
- Brain injury.
A short-term cause of secondary adrenal insufficiency can happen in people who suddenly stop taking medicines called corticosteroids. These medicines treat conditions such as asthma and arthritis. But stopping the medicine suddenly rather than tapering off can lead to secondary adrenal insufficiency.
Risk factors
Most people who get Addison's disease don't have any factors that put them at higher risk of developing the condition. But the following may raise the risk of adrenal insufficiency:
- A history of having a disease or surgery that affects the pituitary gland or the adrenal glands.
- Certain genetic changes that affect the pituitary or adrenal glands. These include gene changes that cause the inherited disease congenital adrenal hyperplasia.
- Other autoimmune endocrine conditions, such as hypothyroidism or type 1 diabetes.
- Traumatic brain injury.
Complications
Addison's disease can lead to other health conditions called complications. These include adrenal crisis, also called addisonian crisis. If you have Addison's disease and haven't started treatment, you may develop this life-threatening complication.
Stress on the body such as injury, infection or illness can trigger adrenal crisis. Typically, the adrenal glands make two or three times the usual amount of cortisol in response to physical stress. But with adrenal insufficiency, the adrenal glands don't make enough cortisol to meet this need. And that can lead to adrenal crisis.
Adrenal crisis results in low blood pressure, low blood levels of sugar and high blood levels of potassium. This complication needs treatment right away.
Prevention
Addison's disease can't be prevented. But you can take steps to lower the risk of adrenal crisis:
- Talk with your healthcare professional if you always feel tired or weak or are losing weight without trying. Ask if you should get tested for adrenal insufficiency.
- If you have Addison's disease, ask your healthcare professional what to do when you're sick. You'll likely need to learn how to adjust the amount of medicine that you take. You also may need to take the medicine as a shot.
- If you become very sick, go to an emergency room. This is crucial if you're vomiting and you can't take your medicine.
Some people with Addison's disease worry about serious side effects from corticosteroid medicines. But people with Addison's disease aren't likely to get the side effects of high-dose corticosteroids used to treat many other diseases. That's because the dose prescribed is much lower and only replaces the amount that's missing.
If you take corticosteroids, follow up with your healthcare professional regularly to make sure your dose is not too high.
Dec. 21, 2024