概述
髓母细胞瘤是一种始于脑的后下部的癌性脑肿瘤。这部分脑称为小脑。小脑参与肌肉协调、平衡和运动。
髓母细胞瘤始于细胞生长物(肿瘤)。这些细胞生长迅速,并可扩散到脑的其他部位。髓母细胞瘤一般通过围绕和保护脑和脊髓的液体而扩散。这种液体称为脑脊液。髓母细胞瘤通常不会扩散至身体其他部位。
髓母细胞瘤可能发生在任何年龄段,但在幼童中最为常见。虽然髓母细胞瘤较为罕见,但却是儿童中最常见的癌性脑肿瘤。髓母细胞瘤更常发生于有特定状况病史的家庭,而这些状况会增加癌症风险。如 Gorlin 综合征或特科特综合征。
Types
The type of medulloblastoma is based on how the tumor cells look under a microscope and on lab tests that look at changes in the tumor's genes. The type of medulloblastoma helps guide treatment and can affect survival.
All medulloblastomas are considered grade 4 tumors. The subtypes below describe the tumor's molecular features, not its grade.
Molecular types
Most medulloblastomas can be grouped into four main types based on changes in their genes. These tumor types include:
- WNT-activated (wingless/integrated). WNT is the name of a cell signaling pathway involved in brain development. WNT-activated tumors are one of the less common medulloblastoma types. They often respond very well to treatment and are linked to the best survival rates. They are most often seen in older children and teens.
- SHH-activated (sonic hedgehog). Sonic hedgehog is the name of a cell growth signaling pathway involved in brain development. SHH medulloblastoma can occur in infants, children and adults. Survival varies depending on other tumor features and gene changes. Some SHH tumors, known as SHH-activated TP53-wildtype, behave less aggressively. Other SHH tumors, called SHH-activated TP53-mutant, may be harder to treat.
- Group 3. Group 3 medulloblastoma is more common in young children. These tumors are non-SHH and non-WNT molecular types. It tends to grow and spread more quickly than other types. It may be harder to treat and is often linked to lower survival rates compared with WNT tumors.
- Group 4. Group 4 medulloblastoma is the most common type. These tumors are non-SHH and non-WNT molecular types. It can occur in children and adults. Its behavior varies. Some tumors respond well to treatment, while others may spread at diagnosis.
The numbering starts at 3 and 4 because the first two groups were named WNT-activated and SHH-activated based on specific gene patterns.
Cell appearance types
Medulloblastoma also can be described based on how the cells look under a microscope although genetic and molecular features are increasingly used for diagnosis and understanding outcomes. These include:
- Classic.
- Desmoplastic or nodular.
- Large cell or anaplastic.
These features also help healthcare professionals understand how the tumor may behave.
How is medulloblastoma different from other brain tumors?
Medulloblastoma is different from many other types of brain tumors. These tumors differ in where they start, who they affect and how they are treated.
Here's how they compare:
- Medulloblastoma versus glioma. Medulloblastoma is not a glioma. Gliomas form from support cells in the brain called glial cells. Medulloblastoma forms from developing nerve cells in the cerebellum.
- Medulloblastoma versus glioblastoma. Glioblastoma is an aggressive brain tumor that usually affects adults and starts in the upper parts of the brain. Medulloblastoma is more common in children and often responds better to treatment.
- Medulloblastoma versus ependymoma. Ependymomas begin in cells that line the fluid-filled spaces of the brain and spinal cord. Medulloblastoma tends to grow in the cerebellum and is more likely to spread through cerebrospinal fluid.
症状
髓母细胞瘤
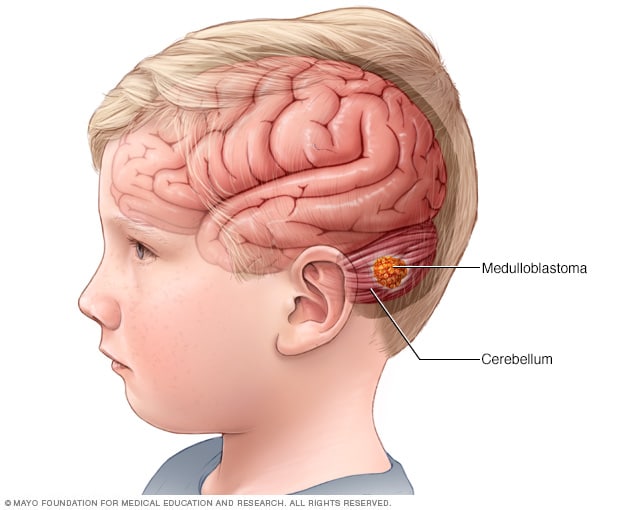
髓母细胞瘤
髓母细胞瘤是一种脑癌,始于脑部称为小脑的部位。髓母细胞瘤是儿童最常见的癌性脑肿瘤类型。
髓母细胞瘤随着癌变部位生长或导致脑内压力积聚而出现症状。髓母细胞瘤的体征和症状可能包括:
- 头晕。
- 复视。
- 头痛。
- 恶心。
- 协调性差。
- 疲倦。
- 步态不稳。
- 呕吐。
Symptoms in young children and infants
In young children, symptoms may develop over several weeks. Children may have trouble walking, seem clumsy or lose balance. Infants may have an increase in head size, unusual sleepiness or feeding difficulties.
Symptoms in children and adults
Symptoms of medulloblastoma are generally similar in adults and children because the tumor usually starts in the same part of the brain. Both may have headaches, balance difficulties and nausea.
Can you feel a medulloblastoma tumor?
Medulloblastoma grows deep inside the brain. It does not usually cause a lump or bump that you can feel on the outside of the head.
何时就医
如果任何症状令您担心,请与医生或其他医疗护理专业人员约诊。
病因
髓母细胞瘤的病因尚不明确。这种癌症最开始是位于脑内的细胞生长物。
髓母细胞瘤是由脑内细胞的 DNA 发生变化所致。细胞的 DNA 含有指示细胞工作的指令。在健康细胞中,DNA 会发出指令让细胞以一定的速度生长和增殖。这些指令会指示细胞在设定的时间死亡。而在癌细胞中,DNA 的变化给出了不同的指令。这些变化指示癌细胞快速生长和增殖。在正常细胞应该死亡时,癌细胞仍继续存活。这会导致细胞过多。
癌细胞形成肿块(肿瘤),可能生长并压迫邻近结构。癌细胞可以侵入并破坏健康的身体组织。它们还可能扩散到其他部位。
风险因素
可能增加髓母细胞瘤风险的因素包括:
- 年幼。 髓母细胞瘤炎可能发生在任何年龄段。但最常见于儿童。
- 遗传综合征。 髓母细胞瘤更常发生于有特定状况病史的家庭,而这些状况会增加癌症风险。这类状况包括范科尼贫血、Gorlin 综合征、利-弗劳梅尼综合征、鲁宾斯坦-泰比综合征和特科特综合征。