Diagnosis

Sometimes a 3D printer is used to create an exact model of a patient's body to help plan complex operations for Wilms tumor.
To diagnose Wilms tumor, a health care provider might take a family history and do the following:
- A physical exam. The provider will look for possible signs of Wilms tumor.
- Blood and urine tests. These lab tests can show how well the kidneys are working.
- Imaging tests. Tests that create images of the kidneys help find whether a child has a kidney tumor. Imaging tests may include ultrasound, CT scans or MRI and chest X-rays.
Staging the cancer
After finding Wilms tumor, the health care team might recommend other tests to see if the cancer has spread. This is called the cancer's stage. A chest X-ray or chest CT scan and bone scan can show whether the cancer has spread past the kidneys.
The stage of the cancer helps with deciding treatment. In the United States, the stages for Wilms tumor are:
- Stage 1. The cancer is found only in one kidney. Surgery can remove it all.
- Stage 2. The cancer has spread beyond the kidney, such as to nearby fat or blood vessels. But surgery can still remove it all.
- Stage 3. The cancer has spread beyond the kidneys to nearby small organs that fight infection, also known as lymph nodes. It might also have spread to other places within the abdomen. The cancer cells might spill within the abdomen before or during surgery, or surgery might not be able to remove all the cancer.
- Stage 4. The cancer has spread outside the kidney to other places in the body, such as the lungs, liver, bones or brain.
- Stage 5. Cancer cells are found in both kidneys. The tumor in each kidney is staged by itself.
More Information
Treatment
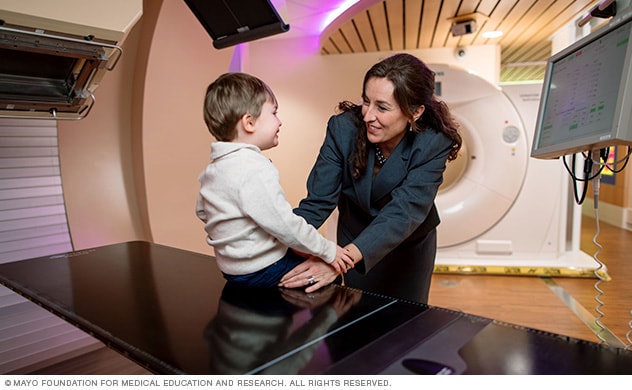
Some children with Wilms tumor may be candidates for Mayo Clinic's proton beam therapy. This highly advanced technology targets and destroys cancer while sparing healthy tissue.
Treatment for Wilms tumor usually involves surgery and chemotherapy. It sometimes includes radiation therapy. Treatments depend on the stage of the cancer. Because this type of cancer is rare, a children's cancer center that has treated this type of cancer might be a good choice.
Surgery
Treatment for Wilms tumor may begin with surgery to remove all or part of a kidney. Surgery also confirms the diagnosis. The tissue removed during surgery is sent to a lab to learn whether it's cancerous and what type of cancer is in the tumor.
Surgery for Wilms tumor may include:
- Removing part of the kidney. Known as a partial nephrectomy, this involves removing the tumor and a small part of the kidney around it. This might be done if the cancer is very small or for a child who has only one working kidney.
- Removing the kidney and surrounding tissue. Known as a radical nephrectomy, this type of surgery also involves removing nearby lymph nodes, part of the ureter and sometimes the adrenal gland. The kidney that's left can take on the work of both kidneys.
- Removing all or part of both kidneys. If the cancer affects both kidneys, surgery involves removing as much cancer as possible from both. Sometimes, this means removing both kidneys. The child would then need kidney dialysis or a kidney transplant.
Chemotherapy
Chemotherapy uses strong medicines to kill cancer cells throughout the body. Treatment for Wilms tumor usually involves using more than one medicine to kill cancer cells. The medicine is given through a vein.
Side effects of chemotherapy depend on the medicines used. Common side effects include nausea, vomiting, loss of appetite, hair loss and higher risk of infections. Ask your child's health care team what side effects might happen during treatment. Ask if there might be long-term problems as a result of treatment.
If given before surgery, chemotherapy can shrink tumors and make them easier to remove. After surgery, it can kill cancer cells that are left in the body. Chemotherapy may also be an option for children whose cancers are too far along to be removed completely with surgery.
For children who have cancer in both kidneys, chemotherapy is given before surgery. This may make it more likely that one kidney might be saved.
Radiation therapy
Some children might have radiation therapy. Radiation therapy uses high-powered energy beams to kill cancer cells. The energy can come from X-rays, protons and other sources.
During radiation therapy, the child is placed on a table. A large machine moves around the child, pointing energy beams at the cancer. Possible side effects include nausea, diarrhea, tiredness and sunburn-like skin irritation.
Some children will have radiation therapy after surgery to kill any cancer cells that are left. It also might be used to control cancer that has spread to other areas of the body. Ask if there might be long-term problems as a result of radiation therapy.
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Coping and support
Here are some suggestions to help you guide your family through cancer treatment.
At the hospital
When your child has medical appointments or stays in the hospital:
- Bring a favorite toy or book to office or clinic visits, to keep your child busy while waiting.
- Stay with your child during a test or treatment, if possible. Describe what will happen using words the child knows.
- Include play time in your child's schedule. Major hospitals usually have a playroom for children being treated. Often playroom staff members have training in child development, recreation, psychology or social work. For children who must stay in their rooms, a child life specialist or recreational therapist might be able to visit.
- Ask for support from clinic or hospital staff members. Look for organizations for parents of children with cancer. Parents who have been through this can provide support, hope and good advice. Ask your child's health care team about local support groups.
At home
After leaving the hospital:
- Monitor your child's energy level outside of the hospital. If your child feels well enough, gently encourage taking part in regular activities. Also make time for rest, especially after chemotherapy or radiation.
- Keep a daily record of your child's body temperature, energy level, sleep, medicines used and side effects. Share this information with your child's health care provider.
- Plan a typical diet unless your child's provider suggests otherwise. Make favorite foods. Chemotherapy can affect wanting to eat. Increase fluids.
- Encourage mouth care. A mouth rinse can be helpful for sores or areas that are bleeding. Use lip balm to soothe cracked lips. Ideally, your child should have needed dental care before treatment begins. Afterward check with your child's provider before scheduling visits to the dentist.
- Check with the provider before vaccinations. Cancer treatment affects the immune system.
- Talk with your other children about the illness. Tell them about changes they might see in the child who has cancer, such as hair loss and low energy. Listen to their concerns.
Preparing for your appointment
If your child is diagnosed with Wilms tumor, you may be referred to specialists. This might be a doctor who treats cancer, which is called an oncologist, or a surgeon who specializes in kidney surgery, which is called a urologist.
What you can do
To prepare for the appointment:
- Make a list of all medicines, vitamins, herbs, oils and other supplements that your child is taking, including doses.
- Ask a family member or friend to come with you to help you remember the information you get during the appointment.
- Write a list of questions to ask your child's health care provider.
For Wilms tumor, some questions to ask include:
- What tests does my child need?
- What stage is my child's cancer?
- What treatments are available, and which do you recommend?
- What types of side effects can these treatments cause?
- Will I need to restrict my child's activity or change the diet during treatment?
- What's my child's outlook?
- What is the likelihood that the cancer will come back?
- Are there brochures or other printed material I can have? What websites do you recommend?
Don't hesitate to ask other questions you have.
What to expect from your doctor
Your child's health care provider is likely to ask you a questions, such as:
- When did you notice your child's symptoms?
- Is there a history of cancer, including childhood cancer, in your family?
- Does your child have any family history of birth defects, especially of the genitals or urinary tract?