Diagnosis
To diagnose scoliosis, your child's healthcare professional may take a medical history and ask about recent growth. During the physical exam, the healthcare professional may have your child stand and bend forward from the waist, with arms hanging loosely. This is to see if one side of the rib cage stands out more than the other.
The healthcare professional also may do an exam to check the nervous system, called a neurological exam. The exam checks for:
- Muscle weakness.
- Numbness.
- Reflexes.
Imaging tests
X-rays can confirm the diagnosis of scoliosis and measure the spinal curve. Children who are growing most often get X-rays every six months to see if the curve is getting worse. This might make the radiation from the X-rays a worry.
To reduce this risk, your healthcare professional may suggest a special type of X-ray imaging that uses much lower doses of radiation. Most medical centers that specialize in scoliosis care offer this type of imaging.
Some children get an X-ray of the hand to show how much more they'll grow. The X-ray of the hand shows whether the growth plates are open and still growing.
You might have an MRI if your healthcare professional suspects that an underlying condition, such as a spinal cord issue, is causing the scoliosis. MRI scans don't use radiation.
More Information
Treatment
Scoliosis treatment depends on the size of the curve and how much more the child is likely to grow. Even children with small curves may need regular checkups to see if the curve is getting worse as they grow. Older teenagers who have mild curves often don't need treatment.
A moderate or large spinal curve might need bracing or surgery. That may depend on:
- How mature the child is. If a child's bones have stopped growing, the risk of the curve getting worse is low. Braces have the most effect in children whose bones are still growing. A healthcare professional can check how mature the bones are with hand X-rays.
- Size of curve. Larger curves are more likely to get worse with time.
- People assigned female at birth. They have a higher risk of the curve getting worse than do people assigned male at birth.
Braces
Scoliosis brace
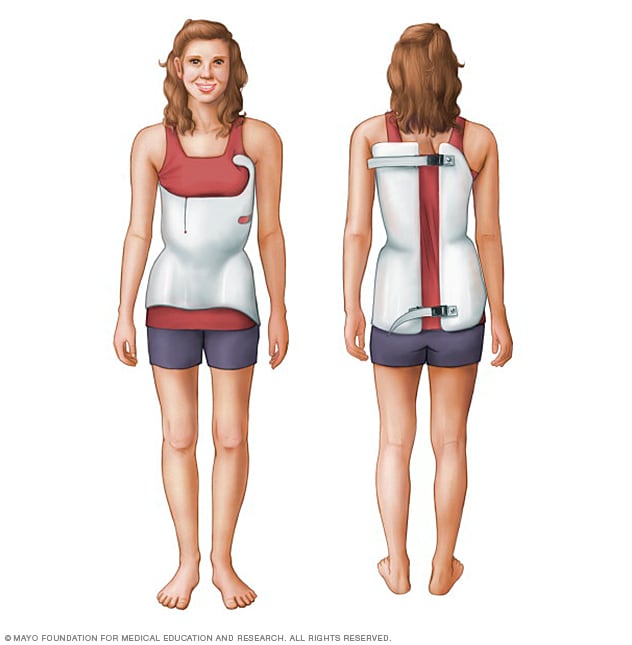
Scoliosis brace
This low-profile brace is made of plastic materials. It forms to the body.
Children with moderate scoliosis whose bones are still growing may wear a brace. The brace most often won't cure scoliosis or reverse the curve. But it may keep a moderate curve from getting worse.
The most common type of brace is made of plastic. It forms to the body. This brace fits under the arms and around the rib cage, lower back and hips. It's hard to see under clothes.
Most children who have a brace wear it from 13 to 18 hours a day. A brace works better the more it's worn. Children who wear braces can take part in most activities. If they need to, children can take off the brace to play sports or do other physical activities.
Some braces are designed to be worn only at night. They may work for some types of scoliosis.
Children who have stopped growing may no longer need the brace. People assigned female at birth most often stop growing at age 14. People assigned male at birth most often stop growing at age 16. But the age varies from person to person.
Surgery
Scoliosis can get worse over time. This is most likely in children who are still growing. For large curves, your healthcare professional might suggest scoliosis surgery to help straighten the curve and keep it from getting worse.
Surgical options include:
-
Spinal fusion. In this procedure, surgeons join 6 to 12 of the bones in the spine, called vertebrae. Then they can't move by themselves. The surgeon puts pieces of bone or a bonelike material between the vertebrae.
Surgeons do this procedure through a cut in the back of the spine, called an incision. The fused area of the spine where the scoliosis was treated gets stiff. Most people can return to sports in 3 to 6 months after surgery.
The surgeon puts metal rods and special screws in the vertebrae to hold that part of the spine straight and still. That lets the old and new bone material fuse.
- Vertebral body tethering. Surgeons do this procedure through small cuts, called incisions. A surgeon puts screws along the outside edge of the spinal curve and threads a strong cord through the screws. Tightening the cord straightens the spine. As the child grows, the spine may straighten even more. This procedure lets the spine move as usual.
-
Expanding or growing rods. If the scoliosis gets worse fast at a young age, surgeons can attach one or two rods along the spine. The rods expand, so they get longer as the child grows.
Some rods expand on their own. For other rods, a healthcare professional makes the rods longer every 3 to 6 months using a magnetic remote control in a clinic. Rods used more rarely need to be made longer with surgery twice a year.
Complications of spinal surgery may include infection or, rarely, nerve damage. The spine may keep curving above or below the site of the surgery.
More Information
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
No activities are known to cause or fix scoliosis. Most people with scoliosis don't have to restrict what they do. Carrying a heavy backpack does not cause scoliosis.
Exercise or playing sports may improve overall health and well-being. A healthy diet with enough calcium and vitamin D also may help bone health. Physical therapy can help strengthen the back, ease pain and improve posture.
Alternative medicine
Studies don't show that the following treatments for scoliosis help fix the curve:
- A procedure that uses controlled force to move a joint past its range of motion, called spinal manipulation.
- Soft braces.
- Electrical stimulation of muscles.
- Dietary supplements.
Coping and support
Coping with scoliosis can be tough for teenagers. They are dealing with many physical changes and emotional and social challenges. A diagnosis of scoliosis can add distress.
Having caring friends can help a child or teen cope with scoliosis, bracing or surgical treatment. Urge your child to talk to friends and ask for their support.
You might try a support group for parents and kids with scoliosis. People in the group can share advice and help you connect with others who have challenges like those of you and your child.
Preparing for your appointment
Your child's healthcare team may check for scoliosis at a well-child visit. Many schools also have screening programs for scoliosis. A physical exam before joining a sport may show scoliosis.
If someone tells you your child might have scoliosis, see your healthcare professional to confirm the condition. Your healthcare professional may send you to a specialist in treating children with scoliosis, called a pediatric orthopedic surgeon.
What you can do
Before the appointment, write a list that includes:
- Details of any symptoms your child has and when they began.
- Your child's medical history.
- Your family's medical history.
- Questions you want to ask the healthcare team.
What to expect from your doctor
Your healthcare team may ask some questions such as:
- Are your child's symptom causing pain?
- Does your child have trouble breathing?
- Has anyone in the family been treated for scoliosis?
- Has your child's growth been fast over the past six months?
- Does your child get periods? When did they start?