Overview
Patent ductus arteriosus
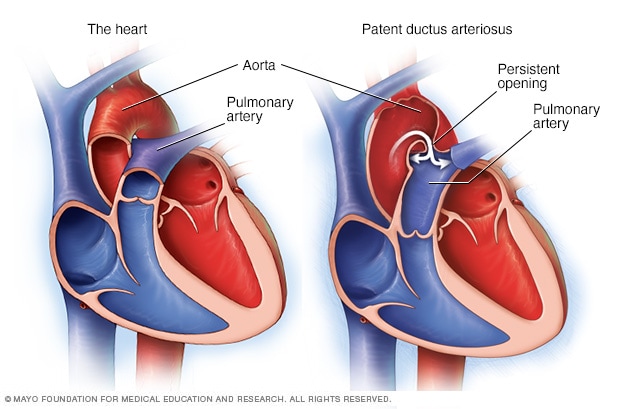
Patent ductus arteriosus
Patent ductus arteriosus is a persistent opening between the two main blood vessels leaving the heart. Those vessels are the aorta and the pulmonary artery. The condition is present at birth, which means it is a congenital heart defect.
Patent ductus arteriosus (PDA) is a persistent opening between the two major blood vessels leading from the heart.
An opening called the ductus arteriosus is part of the blood flow system in the womb for an unborn baby, also called a fetus. It usually closes shortly after birth. If the opening remains open, it's called a patent ductus arteriosus. A PDA is a type of congenital heart defect.
A small PDA might never need treatment. But a large, untreated patent ductus arteriosus can let oxygen-poor blood move the wrong way. This can make the heart muscle weak, causing heart failure and other complications.
Treatments for patent ductus arteriosus may include regular health checkups, medicines, and a procedure or surgery to close the opening.
Products & Services
Symptoms
Patent ductus arteriosus symptoms (PDA) depend on the size of the opening and the person's age. A small PDA might not cause symptoms. Some people don't notice symptoms until adulthood. A large PDA can cause symptoms of heart failure soon after birth.
A large PDA found during infancy or childhood might cause:
- Poor eating, which leads to poor growth.
- Sweating with crying or eating.
- Constant fast breathing or being out of breath.
- Easy tiring.
- Rapid heart rate.
When to see a doctor
Contact a healthcare professional if your baby or older child:
- Tires easily when eating or playing.
- Isn't gaining weight.
- Becomes breathless when eating or crying.
- Always breathes fast or is short of breath.
Causes
The exact causes of patent ductus arteriosus and other congenital heart defects are not clear. During the first six weeks of pregnancy, an unborn baby's heart starts to form and beat. The major blood vessels to and from the heart grow. It's during this time that certain congenital heart defects may begin to develop.
Before birth, there is a temporary opening called the ductus arteriosus between the two main blood vessels leaving a baby's heart. Those vessels are the aorta and the pulmonary artery. The opening is needed for a baby's blood flow before birth. It moves blood away from a baby's lungs while they develop. The baby gets oxygen from the mother's blood.
After birth, the ductus arteriosus is no longer needed. It usually closes within 2 to 3 days. But in some infants, the opening doesn't close. When it stays open, it's called a patent ductus arteriosus.
The constant opening causes too much blood to flow to the baby's lungs and heart. Untreated, the blood pressure in the baby's lungs might increase. The baby's heart might grow larger and get weak.
Risk factors
Risk factors for patent ductus arteriosus (PDA) include:
- Premature birth. Patent ductus arteriosus occurs more commonly in babies who are born too early than in babies who are born full term.
- Family history and other genetic conditions. A family history of heart conditions present at birth may increase the risk of PDA. Babies born with an extra chromosome 21, a condition called Down syndrome, also are more likely to have patent ductus arteriosus.
- German measles during pregnancy. Having German measles, also called rubella, during pregnancy can cause changes in an unborn baby's heart. A blood test done before pregnancy can tell if you're immune to rubella. A vaccine is available for those who aren't immune.
- Being born at a high altitude. Babies born above 8,200 feet (2,499 meters) have a greater risk of PDA than babies born at lower altitudes.
- Female sex assigned at birth. Patent ductus arteriosus is twice as common in girls.
Complications
A small patent ductus arteriosus might not cause complications. Larger, untreated PDAs could cause:
- High blood pressure in the lungs, also called pulmonary hypertension. A large PDA causes irregular blood flow in the heart and lungs. As a result, pressure goes up in the pulmonary artery. Over time, the increased pressure damages the smaller blood vessels in the lungs. A life-threatening and lasting type of lung damage called Eisenmenger syndrome may occur.
- Heart failure. Symptoms of this serious complication include rapid breathing, often with gasping breaths, and poor weight gain.
- Heart infection, called endocarditis. Patent ductus arteriosus can increase the risk of germs attaching to areas in the heart. Without quick treatment, endocarditis can damage or destroy the heart valves.
Patent ductus arteriosus and pregnancy
It may be possible to have a successful pregnancy with a small patent ductus arteriosus. However, having a large PDA or a complication such as heart failure, lung damage or irregular heartbeats increases the risk of serious complications during pregnancy.
Before becoming pregnant, talk with your healthcare professional about possible pregnancy risks and complications. Some heart medicines can be dangerous for an unborn baby. Your healthcare professional may stop or change your medicines before you become pregnant.
Together you can plan for any special care needed during pregnancy. If you are at high risk of having a baby with a heart condition present at birth, genetic testing and screening may be done during pregnancy.
Prevention
There is no known prevention for patent ductus arteriosus. However, it's important to do everything possible to have a healthy pregnancy. Here are some of the basics:
- Get early prenatal care, even before you're pregnant. If you're thinking about pregnancy, talk with your healthcare team to develop a prenatal care plan. Also tell your healthcare professional about all the medicines you take, including those bought without a prescription.
- Start taking folic acid. Taking 400 micrograms of folic acid daily before and during pregnancy has been shown to reduce brain and spinal cord conditions in the baby. It also may help reduce the risk of heart conditions.
- Exercise and stay active. Work with your healthcare professional to develop an exercise plan that's right for you.
- Do not drink alcohol or smoke. These lifestyle habits can harm a baby's health. Also avoid secondhand smoke.
- Get recommended vaccines. Update your vaccinations before becoming pregnant. Certain types of infections can be harmful to a developing baby.
- Control blood sugar. If you have diabetes, good control of your blood sugar may reduce the risk of certain heart conditions present at birth in your baby.
Jan. 29, 2025