Overview
Heart failure occurs when the heart muscle doesn't pump blood as well as it should. When this happens, blood often backs up and fluid can build up in the lungs, causing shortness of breath.
Some heart conditions slowly leave the heart too weak or stiff to fill and pump blood properly. These conditions include narrowed arteries in the heart and high blood pressure.
Proper treatment may improve the symptoms of heart failure and may help some people live longer. Lifestyle changes can improve quality of life. Try to lose weight, exercise, use less salt and manage stress.
But heart failure can be life-threatening. People with heart failure may have severe symptoms. Some may need a heart transplant or a device to help the heart pump blood.
Heart failure also may be called congestive heart failure.
Symptoms
Heart failure
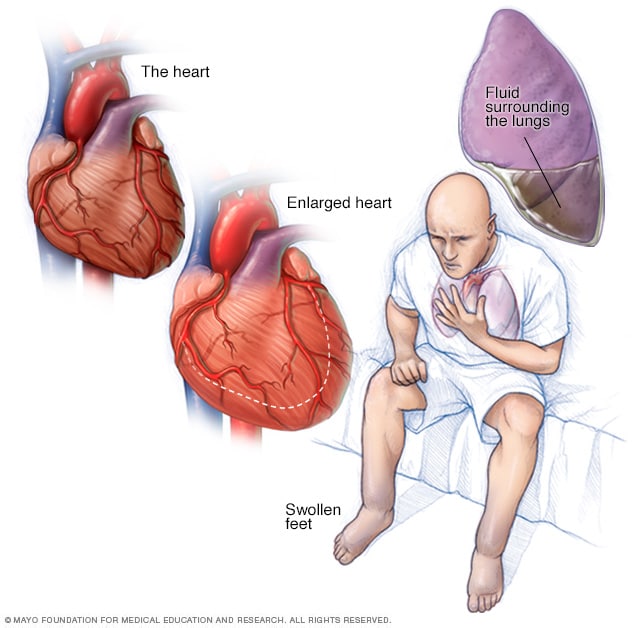
Heart failure
Heart failure occurs when the heart muscle doesn't pump blood as well as it should. Blood often backs up and causes fluid to build up in the lungs and in the legs. The fluid buildup can cause shortness of breath and swelling of the legs and feet. Poor blood flow may cause the skin to look blue or gray. Depending on your skin color, these color changes may be harder or easier to see. Some types of heart failure can lead to an enlarged heart.
If you have heart failure, your heart can't supply enough blood to meet your body's needs.
Symptoms may develop slowly. Sometimes, heart failure symptoms start suddenly. Heart failure symptoms may include:
- Shortness of breath with activity or when lying down.
- Fatigue and weakness.
- Swelling in the legs, ankles and feet.
- Rapid or irregular heartbeat.
- Reduced ability to exercise.
- Wheezing.
- A cough that doesn't go away or a cough that brings up white or pink mucus with spots of blood.
- Swelling of the belly area.
- Very rapid weight gain from fluid buildup.
- Nausea and lack of appetite.
- Difficulty concentrating or decreased alertness.
- Chest pain if heart failure is caused by a heart attack.
When to see a doctor
See your healthcare professional if you think you might have symptoms of heart failure. Call 911 or emergency medical help if you have any of the following:
- Chest pain.
- Fainting or severe weakness.
- Rapid or irregular heartbeat with shortness of breath, chest pain or fainting.
- Sudden, severe shortness of breath and coughing up white or pink, foamy mucus.
These symptoms may be due to heart failure. But there are many other possible causes. Don't try to diagnose yourself.
At the emergency room, healthcare professionals do tests to learn if your symptoms are due to heart failure or something else.
Call your healthcare professional right away if you have heart failure and:
- Your symptoms suddenly get worse.
- You develop a new symptom.
- You gain 5 pounds (2.3 kilograms) or more within a few days.
Such changes could mean that existing heart failure is getting worse or that treatment isn't working.
Causes
Chambers and valves of the heart
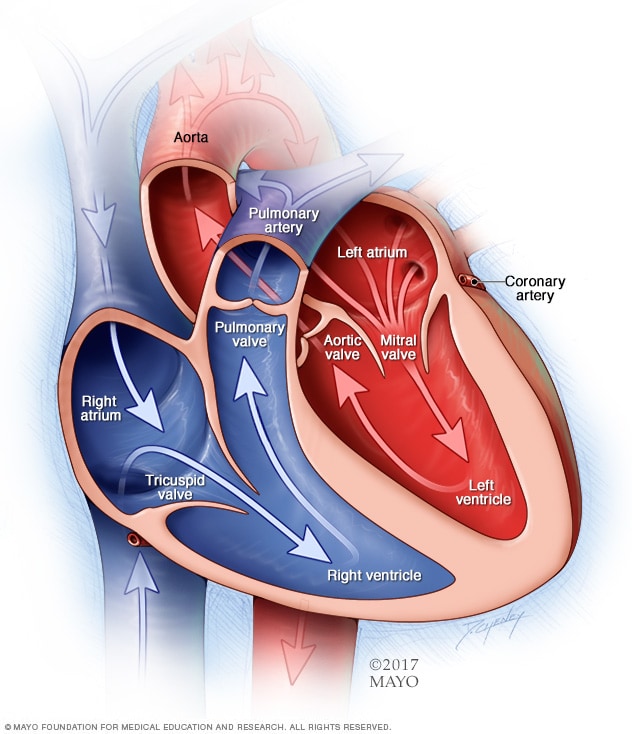
Chambers and valves of the heart
A typical heart has two upper and two lower chambers. The upper chambers, the right and left atria, receive incoming blood. The lower chambers, the more muscular right and left ventricles, pump blood out of the heart. The heart valves, which keep blood flowing in the right direction, are gates at the chamber openings.
Enlarged heart, in heart failure
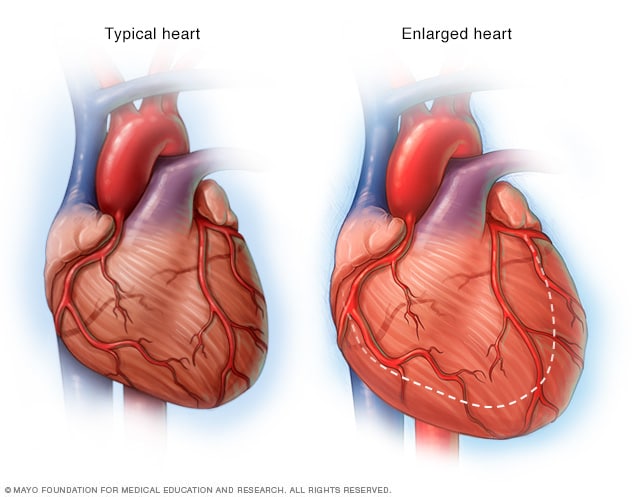
Enlarged heart, in heart failure
If the heart weakens, as it can with heart failure, it begins to enlarge. This forces the heart to work harder to pump blood to the rest of the body.
Heart failure can be caused by a weakened, damaged or stiff heart.
- If the heart is damaged or weakened, the heart chambers may stretch and get bigger. The heart can't pump out the needed amount of blood.
- If the main pumping chambers of the heart, called the ventricles, are stiff, they can't fill with enough blood between beats.
The heart muscle can be damaged by certain infections, heavy alcohol use, recreational drug use and some chemotherapy medicines. Your genes also can play a role.
Any of the following conditions also can damage or weaken the heart and cause heart failure.
-
Coronary artery disease and heart attack. Coronary artery disease is the most common cause of heart failure. The disease results from the buildup of fatty deposits in the arteries. The deposits narrow the arteries. This reduces blood flow and can lead to heart attack.
A heart attack occurs suddenly when an artery feeding the heart becomes completely blocked. Damage to the heart muscle from a heart attack may mean that the heart can no longer pump as well as it should.
- High blood pressure. Also called hypertension, this condition forces the heart to work harder than it should to pump blood through the body. Over time, the extra work can make the heart muscle too stiff or too weak to properly pump blood.
- Heart valve disease. The valves of the heart keep blood flowing the right way. If a valve isn't working properly, the heart must work harder to pump blood. This can weaken the heart over time. Treating some types of heart valve disease may reverse heart failure.
- Inflammation of the heart muscle, also called myocarditis. Myocarditis is most commonly caused by a virus, including the COVID-19 virus, and can lead to left-sided heart failure.
- A heart condition that you're born with, also called a congenital heart defect. If the heart and its chambers or valves haven't formed correctly, the other parts of the heart have to work harder to pump blood. This may lead to heart failure.
- Irregular heart rhythms, called arrhythmias. Irregular heart rhythms may cause the heart to beat too fast, creating extra work for the heart. A slow heartbeat also may lead to heart failure. Treating an irregular heart rhythm may reverse heart failure in some people.
- Other diseases. Some long-term diseases may contribute to chronic heart failure. Examples are diabetes, HIV infection, an overactive or underactive thyroid, or a buildup of iron or protein.
Causes of sudden heart failure also include:
- Allergic reactions.
- Any illness that affects the whole body.
- Blood clots in the lungs.
- Severe infections.
- Use of certain medicines.
- Viruses that attack the heart muscle.
Heart failure usually begins with the lower left heart chamber, called the left ventricle. This is the heart's main pumping chamber. But heart failure also can affect the right side. The lower right heart chamber is called the right ventricle. Sometimes heart failure affects both sides of the heart.
| Type of heart failure |
Description |
| Source: American Heart Association |
| Right-sided heart failure |
This type affects the lower right heart chamber, called the right ventricle. Fluid may back up into the belly, legs and feet, causing swelling. |
| Left-sided heart failure |
This type affects the lower left heart chamber, called the left ventricle. Fluid may back up in the lungs, causing shortness of breath. |
| Heart failure with reduced ejection fraction (HFrEF), also called systolic heart failure |
This is a type of left-sided heart failure. The left ventricle can't squeeze as strong as it should. The heart isn't strong enough to pump enough blood to the body. |
| Heart failure with preserved ejection fraction (HFpEF), also called diastolic heart failure |
This is a type of left-sided heart failure. The left ventricle can't relax or fill fully. The heart has trouble filling with blood. |
Risk factors
Diseases and conditions that increase the risk of heart failure include:
- Coronary artery disease. Narrowed arteries may limit the heart's supply of oxygen-rich blood, resulting in weakened heart muscle.
- Heart attack. A heart attack is a form of coronary artery disease that occurs suddenly. Damage to the heart muscle from a heart attack may mean the heart can no longer pump as well as it should.
- Heart valve disease. Having a heart valve that doesn't work properly raises the risk of heart failure.
- High blood pressure. The heart works harder than it has to when blood pressure is high.
- Irregular heartbeats. Irregular heartbeats, especially if they are very frequent and fast, can weaken the heart muscle and cause heart failure.
- Congenital heart disease. Some people who develop heart failure were born with changes in the structure or function of their heart.
- Diabetes. Having diabetes increases the risk of high blood pressure and coronary artery disease.
- Sleep apnea. This inability to breathe properly during sleep results in low blood-oxygen levels and an increased risk of irregular heartbeats. These things can lead to a weakened heart.
- Obesity. People who have obesity have a higher risk of developing heart failure.
- Viral infections. Some viral infections can damage to the heart muscle.
Medicines that may increase the risk of heart failure include:
- Some diabetes medicines. The diabetes medicines rosiglitazone (Avandia) and pioglitazone (Actos) have been found to increase the risk of heart failure in some people. Don't stop taking these medicines without first talking to your healthcare professional.
- Some other medicines. Other medicines that may lead to heart failure or heart conditions include nonsteroidal anti-inflammatory drugs (NSAIDs) and some medicines used to treat high blood pressure, cancer, blood conditions, irregular heartbeats, nervous system diseases, mental health conditions, lung and urinary conditions, and infections.
Other risk factors for heart failure include:
- Aging. The heart's ability to work decreases with age, even in healthy people.
- Alcohol use. Drinking too much alcohol may weaken the heart muscle and lead to heart failure.
- Smoking or using tobacco. If you smoke, quit. Using tobacco increases the risk of heart disease and heart failure.
Complications
If you have heart failure, it's important to have regular health checkups, even if symptoms improve. Your healthcare professional can examine you and run tests to check for complications.
Complications of heart failure depend on your age, overall health and the severity of heart disease. They may include:
- Kidney damage or failure. Heart failure can reduce the blood flow to the kidneys. Untreated, this can cause kidney failure. Kidney damage from heart failure can require dialysis for treatment.
- Other heart changes. Heart failure can cause changes in the heart's size and function. These changes may damage heart valves and cause irregular heartbeats.
- Liver damage. Heart failure can cause fluid buildup that puts too much pressure on the liver. This fluid backup can lead to scarring, which makes it more difficult for the liver to work properly.
- Sudden cardiac death. If the heart is weak, there is a risk of dying suddenly due to a dangerous irregular heart rhythm.
Prevention
One way to prevent heart failure is to treat and control the conditions that can cause it. These conditions include coronary artery disease, high blood pressure, diabetes and obesity.
Some of the same lifestyle changes used to manage heart failure also may help prevent it. Try these heart-healthy tips:
- Don't smoke.
- Get plenty of exercise.
- Eat healthy foods.
- Maintain a healthy weight.
- Reduce and manage stress.
- Take medicines as directed.
Jan. 21, 2025