Overview
Colon cancer
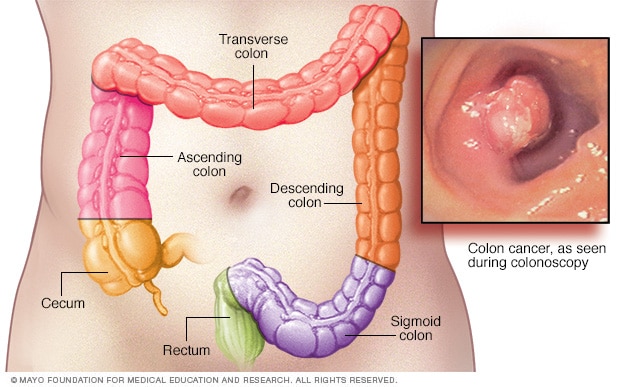
Colon cancer
Colon cancer can happen in any part of the colon. An exam of the whole colon using a long, flexible tube with a camera is one way to detect colon cancer and polyps. This exam is called a colonoscopy.
Colon cancer is a growth of cells that begins in a part of the large intestine called the colon. The colon is the first and longest part of the large intestine. The large intestine is the last part of the digestive system. The digestive system breaks down food for the body to use.
Colon cancer typically affects older adults, though it can happen at any age. It usually begins as small clumps of cells called polyps that form inside the colon. Polyps generally aren't cancerous, but some can turn into colon cancers over time.
Polyps often don't cause symptoms. For this reason, doctors recommend regular screening tests to look for polyps in the colon. Finding and removing polyps helps prevent colon cancer.
If colon cancer develops, many treatments can help control it. Treatments include surgery, radiation therapy and medicines, such as chemotherapy, targeted therapy and immunotherapy.
Colon cancer is sometimes called colorectal cancer. This term combines colon cancer and rectal cancer, which begins in the rectum.
Products & Services
Symptoms
Many people with colon cancer don't have symptoms at first. When symptoms appear, they'll likely depend on the cancer's size and where it is in the large intestine.
Symptoms of colon cancer can include:
- A change in bowel habits, such as more frequent diarrhea or constipation.
- Rectal bleeding or blood in the stool.
- Ongoing discomfort in the belly area, such as cramps, gas or pain.
- A feeling that the bowel doesn't empty all the way during a bowel movement.
- Weakness or tiredness.
- Losing weight without trying.
When to see a doctor
If you notice lasting symptoms that worry you, make an appointment with a health care professional.
Causes
Doctors aren't certain what causes most colon cancers.
Colon cancer happens when cells in the colon develop changes in their DNA. A cells' DNA holds the instructions that tell the cell what to do. The changes tell the cells to multiply quickly. The changes let the cells continue living when healthy cells die as part of their natural lifecycle.
This causes too many cells. The cells might form a mass called a tumor. The cells can invade and destroy healthy body tissue. In time, the cells can break away and spread to other parts of the body. When cancer spreads, it's called metastatic cancer.
Risk factors
Factors that may increase the risk of colon cancer include:
- Older age. Colon cancer can happen at any age. But most people with colon cancer are older than 50. The numbers of people younger than 50 who have colon cancer has been growing. Doctors don't know why.
- Black race. Black people in the United States have a greater risk of colon cancer than do people of other races.
- A personal history of colorectal cancer or polyps. Having had colon cancer or colon polyps increases the risk of colon cancer.
- Inflammatory bowel diseases. Conditions that cause pain and swelling of the intestines, called inflammatory bowel diseases, can increase the risk of colon cancer. These conditions include ulcerative colitis and Crohn's disease.
- Inherited syndromes that increase colon cancer risk. Some DNA changes that increase the risk of colon cancer run in families. The most common inherited syndromes that increase colon cancer risk are familial adenomatous polyposis and Lynch syndrome.
- Family history of colon cancer. Having a blood relative who has colon cancer increases the risk of getting colon cancer. Having more than one family member who has colon cancer or rectal cancer increases the risk more.
- Low-fiber, high-fat diet. Colon cancer and rectal cancer might be linked with a typical Western diet. This type of diet tends to be low in fiber and high in fat and calories. Research in this area has had mixed results. Some studies have found an increased risk of colon cancer in people who eat a lot of red meat and processed meat.
- Not exercising regularly. People who are not active are more likely to develop colon cancer. Getting regular physical activity might help lower the risk.
- Diabetes. People with diabetes or insulin resistance have an increased risk of colon cancer.
- Obesity. People who are obese have an increased risk of colon cancer. Obesity also increases the risk of dying of colon cancer.
- Smoking. People who smoke can have an increased risk of colon cancer.
- Drinking alcohol. Drinking too much alcohol can increase the risk of colon cancer.
- Radiation therapy for cancer. Radiation therapy directed at the abdomen to treat previous cancers increases the risk of colon cancer.
Prevention
Screening for colon cancer
Doctors recommend that people with an average risk of colon cancer consider starting colon cancer screening around age 45. But people with an increased risk should think about starting screening sooner. People with an increased risk include those with a family history of colon cancer.
There are several different tests that are used for colon cancer screening. Talk about your options with your health care team.
Lifestyle changes to reduce the risk of colon cancer
Making changes in everyday life can reduce the risk of colon cancer. To lower the risk of colon cancer:
- Eat a variety of fruits, vegetables and whole grains. Fruits, vegetables and whole grains have vitamins, minerals, fiber and antioxidants, which may help prevent cancer. Choose a variety of fruits and vegetables so that you get a range of vitamins and nutrients.
- Drink alcohol in moderation, if at all. If you choose to drink alcohol, limit the amount you drink to no more than one drink a day for women and two for men.
- Stop smoking. Talk to your health care team about ways to quit.
- Exercise most days of the week. Try to get at least 30 minutes of exercise on most days. If you've been inactive, start slowly and build up gradually to 30 minutes. Also, talk with a health care professional before starting an exercise program.
- Maintain a healthy weight. If you are at a healthy weight, work to maintain your weight by combining a healthy diet with daily exercise. If you need to lose weight, ask your health care team about healthy ways to achieve your goal. Aim to lose weight slowly by eating fewer calories and moving more.
Colon cancer prevention for people with a high risk
Some medicines can reduce the risk of colon polyps or colon cancer. For instance, some evidence links a reduced risk of polyps and colon cancer to regular use of aspirin or aspirin-like medicines. But it's not clear what dose and what length of time would be needed to reduce the risk of colon cancer. Taking aspirin daily has some risks, including ulcers and bleeding in the digestive system.
These options are generally reserved for people with a high risk of colon cancer. There isn't enough evidence to recommend these medicines to people who have an average risk of colon cancer.
If you have an increased risk of colon cancer, discuss your risk factors with your health care team to see if preventive medicines are safe for you.
Dec. 19, 2024