Diagnosis
To diagnose aortic valve stenosis, a healthcare professional examines you and asks questions about your symptoms and medical history. The health professional listens to your heart with a stethoscope. If you have aortic valve stenosis, a sound called a heart murmur may be heard.
Tests
Tests can tell if you have aortic valve stenosis. They also can learn the cause and how severe the condition is.
Tests for aortic valve stenosis may include:
Echocardiogram. Sound waves are used to make pictures of the beating heart. An echocardiogram shows how blood flows through the heart and heart valves. It can tell how severe aortic valve stenosis is. The test also can show if the heart muscle is weakened.
There are different types of echocardiograms. The type you have depends on the information your healthcare team needs. A standard echocardiogram is done from outside the body. An ultrasound device moves over the skin of the chest above the heart. If more details are needed about the heart, a transesophageal echocardiogram may be done. This type creates pictures of the heart from inside the body. The ultrasound device attaches to a tube that goes down the throat and into the esophagus.
- Electrocardiogram (ECG or EKG). This quick test records the electrical activity of the heart. It shows how the heart beats. Sticky patches with sensors on them go on the chest and sometimes the legs. Wires connect the patches to a computer, which displays or prints results. Your healthcare professional can look for signal patterns related to heart disease or swelling of the heart's chambers.
- Chest X-ray. A chest X-ray shows the condition of the heart and lungs. It can show if the heart is bigger than usual, which can occur in aortic valve stenosis. It also can tell if there is calcium buildup on the aortic valve.
- Exercise tests or stress tests. These tests often involve walking on a treadmill or riding a stationary bike while the heart's activity is checked. Exercise tests show how the heart reacts to physical activity and whether valve disease symptoms happen during exercise. If you can't exercise, you may get medicine that affects the heart like exercise does.
- Cardiac computerized tomography (CT) scan. This test uses several X-rays to create detailed images of the heart and heart valves. The test may be done to check the size of the aorta and look at the aortic valve more closely. A CT scan may be done to see how much calcium buildup is on the valve. It also can show how severe the aortic valve stenosis is.
- Cardiac magnetic resonance imaging (MRI) scan. A cardiac MRI uses magnetic fields and radio waves to create detailed images of the heart. This test can show the size of the aorta. It may be used to learn how severe the aortic valve stenosis is.
- Cardiac catheterization. This test isn't often used to diagnose aortic valve disease. But it may be done to see how severe aortic valve disease is or to diagnose the condition if other tests can't. In this test, a doctor places a thin, flexible tube into a blood vessel, usually in the groin area or arm, and guides it to the heart. Cardiac catheterization also may be used before aortic valve surgery to make sure the heart arteries are not blocked.
After testing confirms a diagnosis of aortic valve disease, your healthcare professional may tell you the stage of disease. Staging helps your healthcare team pick the most appropriate treatment.
Heart valve disease is staged into four basic groups:
- Stage A: At risk. Risk factors for heart valve disease are present.
- Stage B: Progressive. Valve disease is mild or moderate. There are no heart valve symptoms.
- Stage C: Asymptomatic severe. There are no heart valve symptoms but the valve disease is severe.
- Stage D: Symptomatic severe. Heart valve disease is severe and is causing symptoms.
The stage of heart valve disease depends on many things, including symptoms, disease severity, the structure of the valve or valves, and blood flow through the heart and lungs.
More Information
Treatment
Treatment for aortic valve stenosis depends on the symptoms and how severe the condition is. Aortic valve stenosis ranges from mild to severe.
If you have no symptoms or just mild ones, you may only need regular health checkups. Some people need medicines to treat valve disease symptoms or reduce the risk of complications.
Other treatments for aortic valve disease may include:
- Heart-healthy lifestyle changes. Eat healthy, get regular exercise and stay active, and do not smoke.
- Medicines to treat symptoms or reduce the risk of complications.
- Surgery to fix or replace the valve.
Medications
Some people with aortic valve stenosis may need medicines to treat symptoms or reduce the risk of complications. For example, medicines may be used to:
- Lower blood pressure.
- Prevent irregular heartbeats.
- Remove excess fluid from the body to reduce the strain on the heart.
Surgery or other procedures
Biological valve replacement
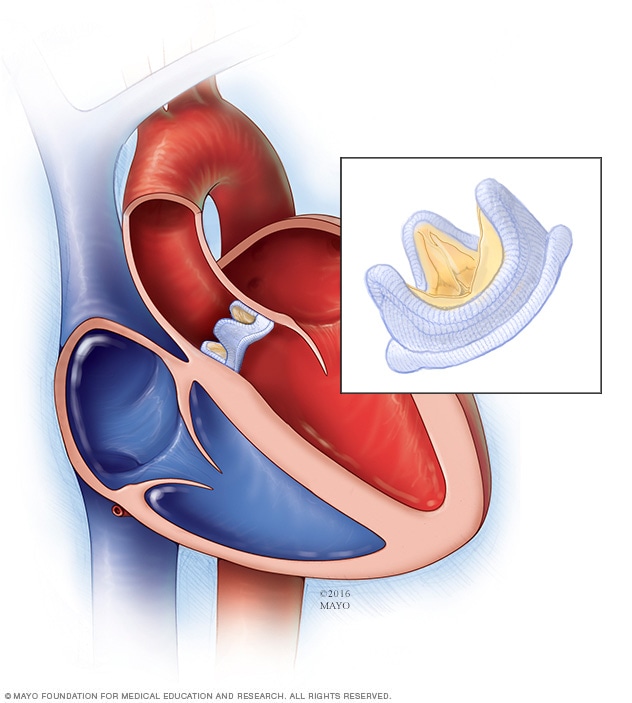
Biological valve replacement
In a biological valve replacement, a valve made from cow, pig or human heart tissue replaces the damaged heart valve.
Mechanical valve replacement

Mechanical valve replacement
In mechanical valve replacement, a mechanical valve replaces the damaged valve.
Transcatheter aortic valve replacement (TAVR)
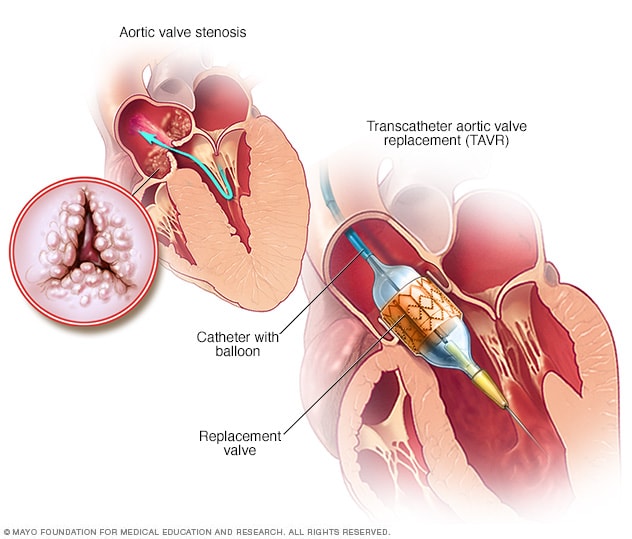
Transcatheter aortic valve replacement (TAVR)
Transcatheter aortic valve replacement, also called TAVR, is a minimally invasive procedure. It is done to replace a narrowed aortic valve that fails to open properly, a condition called aortic valve stenosis. During TAVR, a doctor places a thin, flexible tube into the leg or chest and guides it to the heart. A replacement valve goes through the tube to the correct position in the heart. A balloon on the catheter expands to press the valve into place. Some TAVR valves expand on their own.
You may eventually need a surgery to repair or replace the narrowed aortic valve, even if you don't have symptoms. Aortic valve surgery may be done at the same time as other types of heart surgery.
Surgery to repair or replace an aortic valve is usually done through a cut in the chest. Less invasive approaches may be available. Ask your healthcare professional which type of aortic valve treatment is best for you.
Surgery and procedures for aortic valve stenosis include:
Balloon valvuloplasty. This treatment helps open a narrowed valve. It may be done in infants and children with aortic valve stenosis. In adults, the aortic valve tends to narrow again after the treatment. So it's usually done only if an adult is too sick for surgery or if an adult is waiting for a valve replacement.
In balloon valvuloplasty, a doctor places a thin tube into a blood vessel in the arm or groin and guides it to the aortic valve. Once in place, a balloon on the tip of the tube is inflated. This makes the valve opening wider. The balloon is deflated. The tube and balloon are removed.
Aortic valve replacement. Aortic valve replacement is often needed to treat aortic valve stenosis. In aortic valve replacement, the surgeon takes out the damaged valve and replaces it with a mechanical valve or a valve made from cow, pig or human heart tissue. A tissue valve is called a biological tissue valve.
Sometimes, the aortic valve is replaced with the person's own lung valve, called the pulmonary valve. The pulmonary valve is replaced with a biological lung tissue valve from a deceased donor. This more complicated surgery is called the Ross procedure.
Biological tissue valves break down over time and may eventually need to be replaced. People with mechanical valves need to take blood thinners for life to prevent blood clots. Talk with your healthcare team about the benefits and risks of each type of valve.
Transcatheter aortic valve replacement (TAVR). TAVR is an option to open-heart valve surgery. It uses small cuts and a thin, flexible tube called a catheter to replace the aortic valve. During TAVR, a surgeon replaces a narrowed aortic valve with a valve made of cow or pig tissue. TAVR may be an option if you're at intermediate or high risk of complications from surgical aortic valve replacement. Ask your healthcare team about your options.
During TAVR, the surgeon places a tube into a blood vessel and guides it to the heart. A replacement valve made of cow or pig tissue goes through the tube to the aortic valve area. A balloon on the tube's tip inflates to press the new valve into place. Some valves can self-expand. The tube is removed. Surgeons also may use tubes, called catheters, to put a replacement valve into a biological tissue valve that is no longer working properly.
- Aortic valve repair. Surgeons may fix the aortic valve by separating valve flaps that are stuck together. However, valve repair is rarely used to treat aortic valve stenosis. Generally aortic valve stenosis requires aortic valve replacement.
More Information
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Try these tips to help prevent or slow aortic valve stenosis and other types of heart disease.
- Do not smoke or use tobacco. Smoking is a major risk factor for heart disease. If you smoke and can't quit, talk to your care team about programs or treatments that can help.
- Eat a heart-healthy diet. Eat a variety of fruits and vegetables, low-fat or fat-free dairy products, poultry, fish, and whole grains. Limit salt and saturated fats.
- Keep a healthy weight. Lose weight if you are overweight or have obesity. Losing just a few pounds can help reduce risk factors for heart disease. Ask your healthcare professional what weight is best for you.
- Get regular exercise. Exercise helps manage weight and control risk factors for heart disease. Exercise at least 30 minutes a day on most days of the week. Talk with your healthcare team about the amount and type of exercise that's best for you.
- Manage stress. Learn ways to help reduce emotional stress. Some ideas are to get more exercise, practice mindfulness or connect with others in support groups.
- Control blood pressure, blood sugar and cholesterol. Make lifestyle changes and take medicines as directed. Get regular health checkups.
- Limit alcohol. If you choose to drink alcohol, do so in moderation. For healthy adults, that means up to one drink a day for women and up to two drinks a day for men.
- Get good sleep. Poor sleep may increase the risk of heart disease and other health conditions. Adults should aim for 7 to 9 hours daily.
If you have aortic valve stenosis, your healthcare team may recommend that you limit strenuous activity to avoid overworking your heart.
Pregnancy and aortic valve disease
If you have aortic stenosis and are considering pregnancy, it's important to talk with your healthcare team about your plans. Together, you can talk about the safety of medicines and whether you need treatment for aortic valve stenosis before getting pregnant.
Those with heart valve disease such as aortic valve stenosis usually require close checkups by a healthcare professional during pregnancy. If you have severe aortic stenosis, healthcare professionals may tell you not to get pregnant due to the risk of complications.
Preparing for your appointment
If you think you have aortic valve disease, make an appointment for a health checkup. Consider being seen and treated at a medical center with a multidisciplinary heart valve team. This is a team of heart doctors, called cardiologists, and other healthcare professionals trained and experienced in heart valve disease.
Here's some information to help you prepare for your appointment.
What you can do
- Be aware of pre-appointment restrictions. When you make the appointment, ask if there's anything you need to do in advance. For example, you may be told not to eat or drink for a few hours before a cholesterol test.
- Write down your symptoms, including any that seem unrelated to aortic valve stenosis or the heart.
- Write down important personal information. Include any family history of heart disease and any major stresses or recent life changes.
- Make a list of all medicines, vitamins and supplements you take. Include the dosages.
- Take someone with you, if possible. Someone who goes with you can help you remember information you receive.
- Write down questions to ask your healthcare professional.
For aortic valve stenosis, some basic questions to ask your healthcare professional are:
- What is the likely cause of my symptoms or condition?
- What are other possible causes?
- What tests do I need?
- What's the best treatment?
- What are the options to the treatment you suggested?
- I have other health conditions. How can I best manage them together?
- How do I need to change my diet or activities?
- Should I see a specialist?
- If I need surgery, which surgeon do you recommend for heart valve surgery?
- Is there any information about my condition that I can take home with me? What websites do you recommend?
Don't hesitate to ask any other questions.
What to expect from your doctor
Your healthcare team is likely to ask you many questions such as:
- When did your symptoms start?
- Do you always have symptoms, or do they come and go?
- How bad are your symptoms?
- What, if anything, makes your symptoms better?
- What, if anything, makes your symptoms worse?
- Does anyone in your family have heart disease?