Overview
Holter monitor
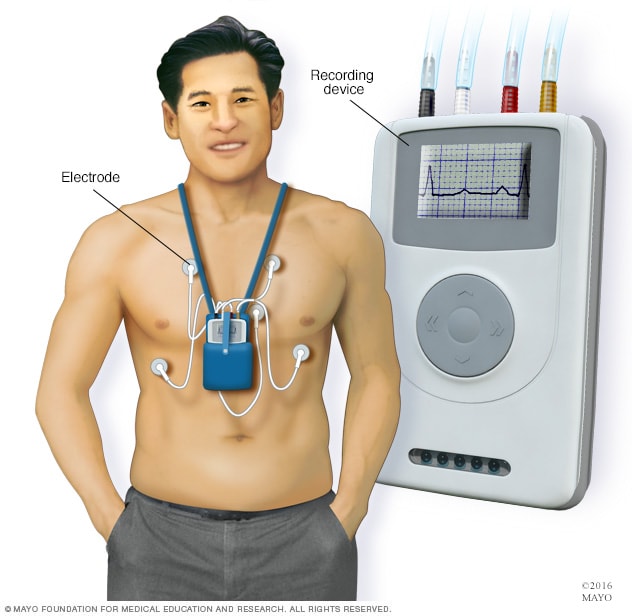
Holter monitor
A Holter monitor is a small, wearable device that continuously checks the heartbeat. It uses one or more sensors called electrodes and a recording device to measure the heart's activity. The device is typically worn for a day or more during daily activities.
A Holter monitor is a small, wearable device that records the heart's rhythm, usually for 1 to 2 days. It's used to spot irregular heartbeats, also called arrhythmias.
A Holter monitor test may be done if a traditional electrocardiogram (ECG or EKG) doesn't provide enough details about the heart's condition.
Some personal devices, such as smartwatches, offer electrocardiogram monitoring. Ask your healthcare professional if this is an option for you.
Products & Services
Why it's done
You may need to use a Holter monitor if you have:
- Symptoms of an irregular heartbeat, also called arrhythmia.
- Fainting with no known cause.
- A heart condition that increases the risk of irregular heartbeats.
Before you get a Holter monitor, you'll have an electrocardiogram (ECG or EKG). An ECG is a quick and painless test. It uses sensors, called electrodes, taped to the chest to check the heart's rhythm.
A Holter monitor may be able to find irregular heartbeats that an ECG missed.
If standard Holter monitoring doesn't find an irregular heartbeat, you may need to wear a device called an event monitor. The device records heartbeats over several weeks.
More Information
Risks
There are no significant risks involved in wearing a Holter monitor. Some people have minor discomfort or skin irritation where the sensors were placed.
Holter monitors aren't usually affected by other electrical appliances. But some devices may interrupt the signal from the electrodes to the Holter monitor. If you have a Holter monitor, avoid the following:
- Electric blankets.
- Electric razors and toothbrushes.
- Magnets.
- Metal detectors.
- Microwave ovens.
Also, keep cellphones and portable music players at least 6 inches from the Holter monitor for the same reason.
How you prepare
You are set up with a Holter monitor during a scheduled appointment at a medical office or clinic. Unless you're told differently, plan to bathe before this appointment. Most monitors can't be removed and must be kept dry once monitoring begins.
Sticky patches with sensors, called electrodes, are placed on your chest. These sensors detect the heartbeat. They're about the size of a silver dollar. If you have hair on your chest, some of it may be shaved to make sure the electrodes stick.
Wires attached to the electrodes connect to the Holter monitor recording device. The device is about the size of a deck of cards.
Once your Holter monitor is fitted and you've received instructions on how to wear it, you can return to everyday activities.
What you can expect
During
A Holter monitor is typically worn for 1 to 2 days. During that time, the device records all of the heartbeats.
Holter monitoring is painless. The electrodes and wires can be hidden under clothing. The device is worn on a belt or attached to a strap.
Don't take the Holter monitor off. It must be worn during the entire recording period, even while sleeping.
Water can damage a Holter monitor. Don't swim, shower or bathe for the entire time you're wearing a Holter monitor. If you have a wireless Holter monitor, you'll be shown how to disconnect and reconnect the sensors and the monitor so that you can shower or bathe.
While you wear a Holter monitor, you can do most other daily activities unless you have instructions to avoid certain things. You may be given a form to record your activities and any symptoms. It's particularly important to note if and when you have any of the following symptoms:
- Pounding, fluttering or skipped heartbeats.
- Shortness of breath.
- Chest pain.
- Lightheadedness.
Write down what activities you do and exactly what time you do them.
After
Once your monitoring period is over, you'll return the device. If you were asked to keep a record of symptoms that you had while wearing the device, the Holter monitor's data will be compared with your notes. This can help your care team make an accurate diagnosis.
Results
Your healthcare professional will review the Holter monitor test results and discuss them with you. Information from Holter monitor testing can show if you have a heart condition and if any heart medicines you currently take are or aren't working.
If you didn't have any irregular heartbeats while you wore the monitor, you may need to wear a wireless Holter monitor or an event recorder. These devices can be worn longer than a standard Holter monitor. Event recorders are similar to Holter monitors and generally require you to push a button when you feel symptoms. There are several different types of event recorders.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.