Overview
Bronchoscopy
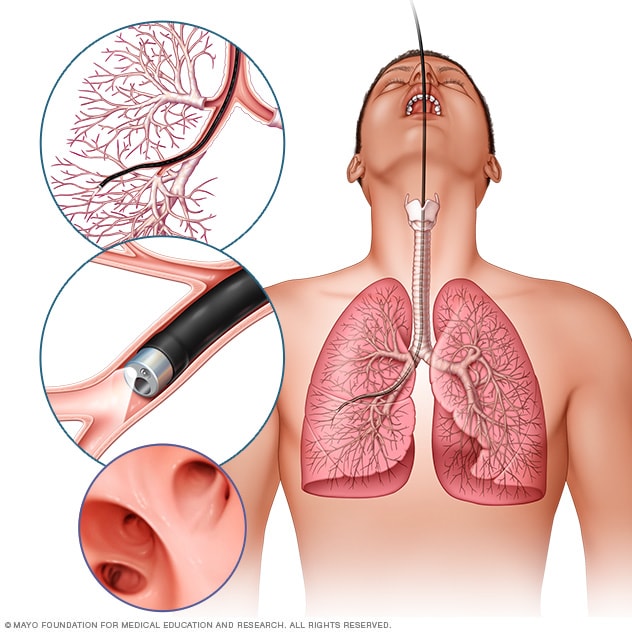
Bronchoscopy
In flexible bronchoscopy, a healthcare professional inserts a thin, bendable tube through the mouth or nose into the lungs. A light and a small camera on the bronchoscope allow the health professional to look inside the lungs' airways.
Bronchoscopy is a procedure that lets doctors look at your lungs and air passages. It's usually performed by a doctor who specializes in lung disorders (a pulmonologist). During bronchoscopy, a thin tube (bronchoscope) is passed through your nose or mouth, down your throat and into your lungs.
Bronchoscopy is most commonly performed using a flexible bronchoscope. However, in certain situations, such as if there's a lot of bleeding in your lungs or a large object is stuck in your airway, a rigid bronchoscope may be needed.
Common reasons for needing bronchoscopy are a persistent cough, infection or something unusual seen on a chest X-ray or other test.
Bronchoscopy can also be used to obtain samples of mucus or tissue, to remove foreign bodies or other blockages from the airways or lungs, or to provide treatment for lung problems.
Mayo Clinic's approach
Why it's done
Bronchoscopy is usually done to find the cause of a lung problem. For example, your doctor might refer you for bronchoscopy because you have a persistent cough or an abnormal chest X-ray.
Reasons for doing bronchoscopy include:
- Diagnosis of a lung problem
- Identification of a lung infection
- Biopsy of tissue from the lung
- Removal of mucus, a foreign body, or other obstruction in the airways or lungs, such as a tumor
- Placement of a small tube to hold open an airway (stent)
- Treatment of a lung problem (interventional bronchoscopy), such as bleeding, an abnormal narrowing of the airway (stricture) or a collapsed lung (pneumothorax)
During some procedures, special devices may be passed through the bronchoscope, such as a tool to obtain a biopsy, an electrocautery probe to control bleeding or a laser to reduce the size of an airway tumor. Special techniques are used to guide the collection of biopsies to ensure the desired area of the lung is sampled.
In people with lung cancer, a bronchoscope with a built-in ultrasound probe may be used to check the lymph nodes in the chest. This is called endobronchial ultrasound (EBUS) and helps doctors determine the appropriate treatment. EBUS may be used for other types of cancer to determine if the cancer has spread.
More Information
Risks
Complications from bronchoscopy are uncommon and usually minor, although they are rarely severe. Complications may be more likely if airways are inflamed or damaged by disease. Complications may be related to the procedure itself or to the sedative or topical numbing medicine.
- Bleeding. Bleeding is more likely if a biopsy was taken. Usually, bleeding is minor and stops without treatment.
- Collapsed lung. In rare cases, an airway may be injured during bronchoscopy. If the lung is punctured, air can collect in the space around the lung, which can cause the lung to collapse. Usually this problem is easily treated, but it may require admission to the hospital.
- Fever. Fever is relatively common after bronchoscopy but is not always a sign of infection. Treatment is generally not needed.
How you prepare
Preparation for bronchoscopy usually involves food and medication restrictions, as well as discussion about additional precautions.
Food and medications
You may be asked to stop taking blood-thinning medications such as aspirin, clopidogrel (Plavix) and warfarin (Coumadin, Jantoven) several days before bronchoscopy. You'll also be asked not to eat or drink for four to eight hours before the procedure.
Clothing and personal items
On the day of the procedure, you'll be asked to put on a gown and take out any dentures, partial dentures or removable bridges. You may also be asked to remove hearing aids, contact lenses or glasses.
Other precautions
If you'll be going home after the procedure, you'll need a friend or family member to take you home. You won't be able to drive because of the lingering effects of the medications used during the procedure. It's also a good idea to have someone stay with you for the rest of the day.
What you can expect
Bronchoscopy is usually done in a procedure room in a clinic or in a hospital operating room. The entire procedure, including prep and recovery time, typically takes about four hours. Bronchoscopy itself usually lasts about 30 to 60 minutes.
Before the procedure
You'll be asked to sit or lie back on a table or a bed with your arms at your sides. You'll be connected to monitors so that the health care team can track your heart rate, blood pressure and oxygen level during the procedure.
You'll be given a sedative medicine through a vein (intravenously) to help you relax. You'll feel sleepy, but you'll still be awake, breathing on your own, and able to indicate a response to any questions your doctor may ask you during the procedure. Sedative medications often result in you having very little memory of the bronchoscopy procedure once it is completed.
A numbing medication called an anesthetic will be sprayed in your throat. Sometimes an anesthetic gel is rubbed in your nose. These medications numb the areas, helping to lessen gagging and coughing as the bronchoscope is placed into your throat. At first the medicine may taste unpleasant, but the taste will go away.
During the procedure
During bronchoscopy, the bronchoscope is placed in your nose or mouth. The bronchoscope has a light and a very small camera at its tip that displays pictures on a monitor to help guide your doctor in performing the procedure.
The bronchoscope is advanced slowly down the back of your throat, through the vocal cords and into the airways. It may feel uncomfortable, but it shouldn't hurt. Your health care team will try to make you as comfortable as possible.
Samples of tissue and fluid may be taken and procedures may be performed using devices passed through the bronchoscope. Your doctor may ask if you have pain in your chest, back or shoulders. In general, you shouldn't feel pain.
After the procedure
You'll be monitored for several hours after bronchoscopy. Your mouth and throat will probably be numb for a couple of hours. You won't be allowed to eat or drink until the numbness wears off. This helps keep food and liquids from entering your airways and lungs.
When your mouth and throat are no longer numb, and you're able to swallow and cough normally again, you can have something to drink. Start with sips of water. Then you may eat soft foods, such as soup and applesauce. Add other foods as you feel comfortable.
You may have a mild sore throat, hoarseness, a cough or muscle aches. This is normal. Warm water gargles and throat lozenges can help lessen the discomfort. Just be sure all the numbness is gone before you try gargling or sucking on lozenges.
Call your doctor right away if you:
- Have a fever that lasts more than 24 hours
- Have increasing chest pain
- Have trouble breathing
- Cough up more than a few tablespoons of blood
Results
Your doctor will usually discuss bronchoscopy results with you one to three days after the procedure. Your doctor will use the results to decide how to treat any lung problems that were found or discuss procedures that were done. It's also possible that you may need other tests or procedures.
If a biopsy was taken during bronchoscopy, it will need to be reviewed by a pathologist. Because the tissue samples need special preparation, some results take longer than others to return. Some biopsy specimens will need to be sent for genetic testing, which might take two weeks or more.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.