Diagnosis
Currently, there isn't a specific test to diagnose Parkinson's disease. A diagnosis is made by a doctor trained in nervous system conditions, known as a neurologist. A diagnosis of Parkinson's is based on your medical history, a review of your symptoms, and a neurological and physical exam.
It can take time to diagnose Parkinson's disease. Healthcare professionals may recommend regular follow-up appointments with neurologists trained in movement disorders to evaluate your condition and symptoms over time and diagnose Parkinson's disease.
Your healthcare team may order some of these tests and procedures:
- Physical and neurological exam. This includes taking your medical history and doing a neurological exam that tests your thinking and mental abilities, senses, coordination, and reflexes.
- Blood and lab tests. These are used to rule out other conditions that may be causing your symptoms.
- Imaging tests, such as an MRI, brain ultrasound and PET scan. These are used to rule out other conditions. They are not very helpful in diagnosing Parkinson's disease.
- A specific single-photon emission computerized tomography (SPECT) scan called a dopamine transporter (DAT) scan. This can help support the suspicion that you have Parkinson's disease and help identify different types of tremor. But it is your symptoms and the results of your neurological exam that determine your diagnosis. Most people do not require a DAT scan.
- Genetic testing. This tests for gene changes if there is a known family history of Parkinson's disease or if you have early-onset disease.
- A short, low-dose treatment of medicines. You may be given medicines used to treat Parkinson's disease to see if you get better. If your symptoms show significant improvement, this may help confirm your diagnosis. You must be given a sufficient dose to show the benefit, as getting low doses for a day or two isn't reliable.
- Follow-up appointments. Regular appointments with neurologists trained in movement disorders may be needed over time to confirm a diagnosis.
-
Alpha-synuclein test. This test, also called an alpha-synuclein seed amplification assay, detects Parkinson's disease before symptoms begin. Alpha-synuclein clumps are a hallmark sign of Parkinson's disease. Healthcare professionals can test for this condition in the skin or spinal fluid.
Alpha-synuclein is found in Lewy bodies. It forms clumps that the body can't break down. The clumps spread and damage brain cells.
In a 2023 study, researchers tested the spinal fluid of more than 1,000 people to look for clumps of the protein alpha-synuclein. The test accurately identified people with Parkinson's disease 87.7% of the time. The test also was highly sensitive for detecting people at risk of Parkinson's disease.
This study of the alpha-synuclein seed amplification assay was the largest so far. Some researchers say the study may be a breakthrough for Parkinson's disease diagnosis, research and treatment trials. But larger studies are needed.
There's hope among researchers that in the future, the test could be done using blood samples rather than spinal fluid.
Treatment
Parkinson's disease can't be cured, but medicines can help control the symptoms. Medicines often work very well. When medicine is no longer helping, some people may have surgery. Your healthcare team also may recommend aerobic exercise, physical therapy that focuses on balancing and stretching, and speech therapy.
Medicines
Medicines may help improve problems with walking, movement and tremor. The medicines work by increasing or substituting for dopamine in the brain.
People with Parkinson's disease have low levels of brain dopamine. But dopamine can't be given directly because it can't enter the brain.
Your symptoms may improve significantly after you start treatment. The benefits may lessen over time, but usually medicines still control symptoms well.
Medicines you may be prescribed include:
-
Carbidopa-levodopa (Rytary, Sinemet, others). Levodopa is the most effective Parkinson's disease medicine. It is a natural chemical that passes into the brain and becomes dopamine. Levodopa is combined with carbidopa to help levodopa reach the brain and to prevent or lessens side effects such as nausea.
Side effects may include nausea and lightheadedness when you stand, called orthostatic hypotension. Higher doses of levodopa may cause involuntary movements, known as dyskinesia. If this happens, your dose may need to be lessened or adjusted.
The benefit from levodopa may lessen over time. It also may wax and wane. This is called wearing off.
Carbidopa-levodopa usually is best taken on an empty stomach if you have advanced Parkinson's disease. Follow your healthcare team's advice on the best time to take it.
- Inhaled levodopa (Inbrija). This medicine helps manage symptoms when oral medicines suddenly stop working during the day.
-
Carbidopa-levodopa infusion (Duopa). This medicine is given through a feeding tube in a gel form and goes directly into the small intestine.
The tube is placed during a minor surgery. There are some risks of having the tube. The tube may fall out or cause an infection at the infusion site.
Carbidopa-levodopa infusion is for patients with advanced Parkinson's who still respond to the medicine but need a more constant level of levodopa. It helps control motor difficulties and other symptoms such as anxiety and depression.
-
Dopamine agonists. Unlike levodopa, dopamine agonists don't change into dopamine. Instead, they mimic dopamine effects in the brain.
They aren't as effective as levodopa in treating symptoms. But they last longer and may be used with levodopa to improve how well it works.
Dopamine agonists include:
- Pramipexole (Mirapex ER).
- Rotigotine (Neupro), given as a patch.
- Apomorphine (Apokyn), a short-acting dopamine agonist shot for quick relief.
Side effects of dopamine agonists may include lightheadedness, nausea, hallucinations and sleepiness. The medicine also may cause involuntary movements and compulsive behaviors, such as hypersexuality, gambling, and eating.
If you're taking these medicines and behaving in ways that aren't typical for you, talk with your healthcare team.
-
Monoamine oxidase B (MAO B) inhibitors. These medicines include:
- Selegiline (Zelapar).
- Rasagiline (Azilect).
- Safinamide (Xadago).
MAO B inhibitors help block an enzyme called monoamine oxidase B (MAO B) that breaks down brain dopamine. When selegiline is given with levodopa, it may keep levodopa from wearing off.
Side effects of MAO B inhibitors may include headaches, nausea, insomnia and confusion.
MAO B inhibitors also may cause hallucinations. When added to carbidopa-levodopa, these medicines increase the risk of hallucinations.
MAO B inhibitors usually are not used along with most antidepressants or some pain medicines because serious but rare reactions may happen. Ask your healthcare professional before taking any other medicines with an MAO B inhibitor.
-
Catechol O-methyltransferase, also called COMT, inhibitors. These help levodopa therapy last longer by blocking an enzyme that breaks down dopamine. They include:
- Entacapone (Comtan).
- Opicapone (Ongentys).
- Tolcapone (Tasmar). This medicine is rarely prescribed because of its risk of serious liver damage and liver failure.
Side effects of COMT inhibitors may include increased risk of involuntary movements. Side effects also may include diarrhea, nausea or vomiting.
-
Anticholinergics. These medicines were used for many years. They aren't used as often now because of their modest benefits and risk of side effects. They may be helpful in controlling severe tremor for some people with Parkinson's disease. They include:
- Benztropine.
- Trihexyphenidyl.
Side effects of anticholinergics may include memory loss, urinary problems, confusion, blurred vision, dry mouth and constipation.
-
Amantadine (Gocovri). This medicine may be taken alone for short-term relief of mild, early-stage Parkinson's disease symptoms. It's mainly used with carbidopa-levodopa during advanced Parkinson's disease to help control involuntary muscle movements.
Side effects of amantadine may include mottled skin, thinking and memory problems, ankle swelling, hallucinations, and agitation.
- Adenosine receptor antagonists (A2A receptor antagonists). One of these medicines is istradefylline (Nourianz). These help prevent the wearing off of dopamine and allow more dopamine to be released. Researchers also are looking into whether these medicines may help treat other Parkinson's disease symptoms.
- Pimavanserin (Nuplazid). This medicine treats hallucinations and delusions that can occur with Parkinson's disease.
Surgery
Deep brain stimulation
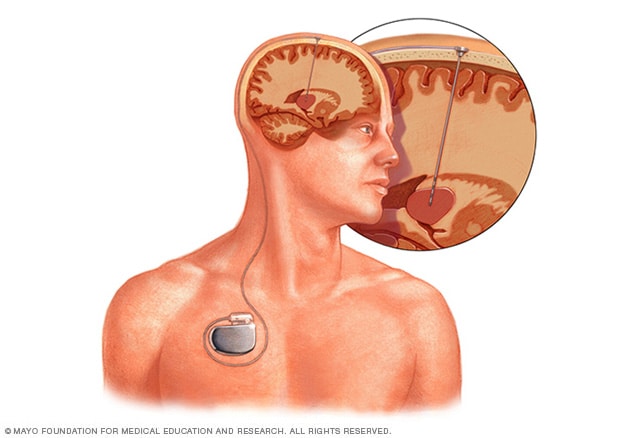
Deep brain stimulation
Deep brain stimulation involves implanting an electrode deep within the brain. The amount of electrical activity delivered by the electrode is controlled by a pacemakerlike device placed under the skin of the chest. A wire that travels under the skin connects the device to the electrode.
Surgery for Parkinson's disease includes deep brain stimulation.
Deep brain stimulation
Deep brain stimulation, also called DBS, involves putting electrodes within the brain. The electrodes are connected to a pacemaker-like device that is inserted under the skin on the chest. The electrodes are connected to a generator placed in the chest near the collarbone. The generator sends electrical pulses to the brain and may reduce Parkinson's disease symptoms.
You may need follow-up appointments to adjust the settings for best results. Some people experience problems with the DBS system or have complications due to stimulation. A member of your healthcare team may need to adjust or replace some parts of the system.
DBS can be very helpful for improving severe tremor and controlling involuntary muscle movements, called dyskinesia. It is effective for controlling changing responses to levodopa or for controlling dyskinesia that doesn't improve with medicine changes.
Deep brain stimulation is most effective for people who respond to levodopa therapy. Although DBS may have long-term benefits for helping with symptoms, it does not keep Parkinson's disease from getting worse. Researchers are looking into ways to improve how well DBS works.
Side effects of deep brain stimulation may include:
- Bleeding in the brain.
- Injury or death of tissue.
- Infection.
- Skin breakage.
- Muscle twitches.
- Depression.
- Speech or vision problems.
Advanced treatments
MRI-guided focused ultrasound, also called MRgFUS, is a minimally invasive treatment that helps manage tremor in some people with Parkinson's disease. An MRI guides an ultrasound to the brain areas where tremor starts. The ultrasound waves are at a very high temperature and burn these areas.
Side effects of MRI-guided focused ultrasound may include:
- Walking and speech problems.
- New involuntary muscle movements, also called dyskinesia.
More Information
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Some lifestyle changes may help ease your Parkinson's disease symptoms. But certain medicines can make your symptoms worse. Ask your healthcare team which remedies provide the greatest symptom relief with the fewest side effects.
Healthy eating
No foods are proved to treat Parkinson's disease, but some may help ease symptoms. For example, eating foods high in fiber and drinking plenty of fluids can help prevent constipation.
A balanced diet also provides nutrients, such as omega-3 fatty acids, that may help people with Parkinson's disease.
Exercise
Exercising may improve your muscle strength, walking, flexibility and balance. It also may help decrease depression and anxiety.
Ask your healthcare professional to suggest a physical therapist who can help create an exercise program for you. Exercises that may help include walking, swimming, gardening, dancing, water aerobics and stretching.
To improve your balance and gait, try these tips:
- Don't move too quickly.
- Put down your heel first when walking.
- Look straight ahead, not down, when you walk.
Prevent falls
The following tips may help:
- Don't rush.
- Don't do too many things at once.
- Use handrails.
- Use night-lights.
- Don't use throw rugs or rolling chairs and keep cords out of the way.
- Learn new turning and walking techniques, including landing on your heel first. Also, stand tall and look straight ahead rather than down at your feet when you walk. If you start shuffling, stop. Check your posture and make sure you're standing up straight.
- Use a walker or cane if your healthcare professional recommends it.
Daily living activities
These healthcare professionals can help with daily tasks:
- Occupational therapist. An occupational therapist can show you ways to help with activities such as dressing, bathing and cooking.
- Speech therapist. A speech therapist may be able to help with swallowing and speech problems.
Alternative medicine
Supportive therapies may help ease some of the symptoms of Parkinson's disease, such as pain, fatigue and depression. When combined with your medical treatments, they may improve your quality of life. These include:
- Massage. Massage therapy can reduce muscle tension and promote relaxation. This therapy is rarely covered by health insurance.
- Tai chi. An ancient form of Chinese exercise, tai chi uses slow, flowing motions that may improve flexibility, balance and muscle strength. Tai chi also may help prevent falls. Several forms of tai chi are tailored for people of any age or physical condition.
- Yoga. In yoga, gentle stretching movements and poses may increase flexibility and balance. You may modify most poses to fit your physical abilities.
- Alexander technique. This technique — which focuses on muscle posture, balance and thinking about how you use muscles — may reduce muscle tension and pain.
- Meditation. In meditation, you quietly reflect and focus your mind on an idea or image. Meditation may reduce stress and pain and improve your sense of well-being.
- Relaxation techniques. These practices help lower blood pressure and heart rate and improve muscle tone.
- Self-hypnosis. This method helps you learn to relax when prompted by your own phrase or suggestion.
Coping and support
Living with any chronic illness can be hard, and it's common to feel angry, depressed or discouraged at times. Parkinson's disease can be profoundly frustrating as walking, talking and even eating become more difficult and time-consuming.
Depression is common in people with Parkinson's disease. But antidepressant medicines can help ease the symptoms of depression. Talk with your healthcare team if you have feelings of sadness or hopelessness that don't go away.
Although friends and family can be your best allies, the understanding of people who know what you're going through can be especially helpful. Support groups aren't for everyone. However, for many people with Parkinson's disease and their families, a support group can be a good resource for practical information about Parkinson's disease.
Also, groups offer a place for you to find people who are going through similar situations and can support you.
Trying to maintain some of your usual activities may be helpful. Aim to do as many things as possible that you could do before Parkinson's disease symptoms started. Focus on the present and try to maintain a positive attitude.
To learn about support groups in your community, talk with your healthcare team, a Parkinson's disease social worker or a local public health nurse. Or contact the Parkinson's Foundation or the American Parkinson Disease Association.
You and your family also may benefit from talking with a mental health professional, such as a psychologist or social worker trained in working with people who have chronic conditions.
Preparing for your appointment
You're likely to first see your family healthcare professional. You may then be referred to a doctor trained in nervous system disorders, called a neurologist.
Because there's often a lot to discuss, it's a good idea to prepare for your appointment. Here's some information to help you get ready.
What you can do
- Write down any symptoms you have, including any that may seem unrelated to the reason for your appointment.
- Write down key personal information, including any major stresses or recent life changes.
- Make a list of all medicines, vitamins and supplements that you're taking.
- Ask a family member or friend to come with you, if possible. Sometimes it can be hard to remember all the information provided to you during an appointment. Someone who goes with you may remember something that you missed or forgot.
- Write down questions to ask during your appointment.
Your time with your care team is limited, so preparing a list of questions ahead of time can help you make the most of your time together. For Parkinson's disease, some basic questions to ask include:
- What's the most likely cause of my symptoms?
- Are there other possible causes?
- What kinds of tests do I need? Do these tests require any special preparation?
- How does Parkinson's disease usually get worse?
- Will I eventually need long-term care?
- What treatments are available, and which do you recommend for me?
- What types of side effects can I expect from treatment?
- If the treatment doesn't work or stops working, do I have additional options?
- I have other health conditions. How can I best manage these conditions together?
- Are there any brochures or other printed material that I can take home with me? What websites do you recommend?
In addition to the questions that you've prepared to ask your care team, don't hesitate to ask questions that occur to you during your appointment.
What to expect from your doctor
Your healthcare team is likely to ask you a several questions. Being ready to answer them may reserve time to go over any points you want to spend more time on. You may be asked:
- When did you first begin having symptoms?
- Do you have symptoms all the time, or do they come and go?
- Does anything seem to improve your symptoms?
- Does anything seem to make your symptoms worse?
Sept. 27, 2024