Overview
Obstructive sleep apnea
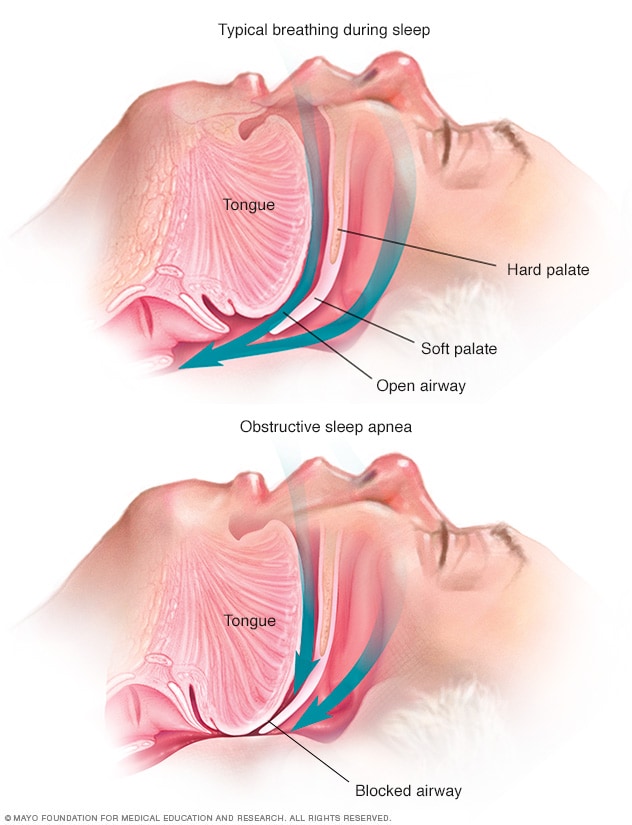
Obstructive sleep apnea
Obstructive sleep apnea occurs when the muscles that support the soft tissues in your throat, such as your tongue and soft palate, relax briefly. When these muscles relax, your airway is narrowed or closed, and breathing is momentarily cut off.
Obstructive sleep apnea is the most common sleep-related breathing disorder. People with obstructive sleep apnea repeatedly stop and start breathing while they sleep. These breath pauses are known as apneas.
There are several types of sleep apnea. Obstructive sleep apnea occurs when the throat muscles relax and block the airway. This happens off and on many times during sleep. A common sign of obstructive sleep apnea is snoring.
Treatments for obstructive sleep apnea are available. One treatment is a device that uses air pressure to keep the airway open during sleep. Another option is a mouthpiece to thrust the lower jaw forward during sleep. In some people, surgery might be an option. In people with obesity, weight loss may improve symptoms of obstructive sleep apnea.
Products & Services
Symptoms
Symptoms of obstructive sleep apnea during the night include:
- Loud snoring.
- Pauses in breathing during sleep, often noticed by a partner.
- Waking during the night gasping or choking.
- Needing to urinate often.
Symptoms of obstructive sleep apnea during the day include:
- Excessive daytime sleepiness.
- Waking in the morning with a dry mouth or sore throat.
- Morning headaches.
- Trouble focusing.
- Mood changes, such as feeling depressed or being easily upset.
- High blood pressure, especially if you're taking multiple medicines to manage it.
- Decreased interest in sex.
When to see a doctor
Consult a healthcare professional if you have, or if your partner notices, the following:
- Snoring loud enough to disturb your sleep or the sleep of others.
- Waking up gasping or choking.
- Pausing in your breathing during sleep.
- Excessive daytime drowsiness. You may fall asleep while working, watching television or even driving a vehicle.
Snoring doesn't always indicate something potentially serious, and not everyone who snores has obstructive sleep apnea.
Be sure to talk to your healthcare professional if you snore loudly, especially if your snoring is interrupted by periods of silence.
Ask your healthcare professional about any sleep issues that leave you fatigued, sleepy and irritable on a regular basis. Excessive daytime drowsiness may be due to other conditions, such as narcolepsy. These conditions are treated separately.
Causes
Obstructive sleep apnea happens when the muscles in the back of the throat relax too much to let you breathe properly. These muscles support the back of the roof of the mouth, known as the soft palate. The muscles also support the tongue and side walls of the throat.
When the muscles relax, the airway narrows or closes as you breathe in. This can lower the level of oxygen in the blood and cause a buildup of carbon dioxide.
Your brain senses this pause in breathing and briefly wakes you so that you can reopen your airway. This awakening is usually so brief that you don't remember it.
You may awaken with shortness of breath that corrects itself quickly, within one or two deep breaths. Or you might make a snorting, choking or gasping sound.
This pattern can repeat itself more than five times an hour during the night. These disruptions make it hard for you to reach the deep, restful phases of sleep, and you'll probably feel sleepy during your waking hours.
People with obstructive sleep apnea might not be aware of their interrupted sleep. Many people with this type of sleep apnea don't realize they haven't slept well all night.
Risk factors
Anyone can develop obstructive sleep apnea. However, certain factors put you at increased risk, including:
- Excess weight. Most but not all people with obstructive sleep apnea are overweight. Fat deposits around the upper airway can obstruct breathing. Medical conditions that are associated with obesity, such as hypothyroidism and polycystic ovary syndrome, also can cause obstructive sleep apnea.
- Older age. The risk of obstructive sleep apnea increases as you age but appears to level off after your 60s and 70s.
- Male sex. In general, men are 2 to 3 times more likely than premenopausal women to have obstructive sleep apnea. However, the risk of obstructive sleep apnea increases in women after menopause.
- A family history of sleep apnea. Having family members with obstructive sleep apnea might increase your risk.
- Narrowed airway. Your tonsils or adenoids might become enlarged and block your airway, increasing your risk of obstructive sleep apnea. Enlarged tonsils are an important risk factor for obstructive sleep apnea in children. A narrowed airway also can be passed down in families.
- Chronic nasal congestion. Obstructive sleep apnea occurs twice as often in those who have consistent nasal congestion at night, no matter what causes it.
- Smoking. People who smoke are more likely to have obstructive sleep apnea.
- Other health conditions. Obstructive sleep apnea is associated with other health conditions, including high blood pressure, heart attack, stroke, irregular heartbeat, diabetes, chronic lung disease and depression.
Complications
Obstructive sleep apnea is considered a serious medical condition. Complications can include:
Fatigue and trouble concentrating. Because of a lack of restorative sleep at night, people with obstructive sleep apnea often have severe daytime drowsiness, fatigue, irritability, symptoms of depression and decreased interest in sex. They might have memory concerns and difficulty concentrating. They may find themselves falling asleep at work, while watching TV or even when driving. This can put them at higher risk of potentially fatal work-related accidents and motor vehicle accidents.
Children and young people with obstructive sleep apnea might do poorly in school. They commonly show attention or behavior issues.
Heart and blood vessel conditions. Sudden drops in blood oxygen levels that occur during obstructive sleep apnea increase blood pressure and strain the cardiovascular system. Many people with obstructive sleep apnea develop high blood pressure, which can increase the risk of heart disease.
The worse the obstructive sleep apnea, the greater the risk of coronary artery disease, heart attack, heart failure and stroke.
Obstructive sleep apnea also increases the risk of heart rhythm conditions known as arrhythmias. Arrhythmias can affect blood pressure. If there's underlying heart disease, repeated episodes of arrhythmias could lead to sudden death.
Complications with medicines and surgery. Obstructive sleep apnea also is a concern with certain medicines and general anesthesia. Medicines such as sedatives, some prescription painkillers and general anesthetics make it harder to breathe and can make obstructive sleep apnea worse.
If you have obstructive sleep apnea, having major surgery can worsen breathing issues. This is especially true if you have been sedated and you were lying on your back. People with obstructive sleep apnea might be more prone to complications after surgery.
Before you have surgery, tell your surgeon if you have obstructive sleep apnea or symptoms related to the condition. You may need to get tested for obstructive sleep apnea before surgery.
- Eye conditions. Some research has found a connection between obstructive sleep apnea and certain eye conditions, such as glaucoma. Eye complications usually can be treated.
- Sleep-deprived partners. Loud snoring can keep those around you from getting good rest and may disrupt your relationships. Some partners choose to sleep in another room.
- COVID-19. Obstructive sleep apnea might be a risk factor for COVID-19. People with obstructive sleep apnea have been found to be at higher risk of developing a severe form of COVID-19. They may be more likely to need hospital treatment than do those who don't have obstructive sleep apnea.
Dec. 04, 2025