Overview
Giant cell arteritis is an inflammation of the lining of your arteries. Most often, it affects the arteries in your head, especially those in your temples. For this reason, giant cell arteritis is sometimes called temporal arteritis.
Giant cell arteritis frequently causes headaches, scalp tenderness, jaw pain and vision problems. Untreated, it can lead to blindness.
Prompt treatment with corticosteroid medications usually relieves symptoms of giant cell arteritis and might prevent loss of vision. You'll likely begin to feel better within days of starting treatment. But even with treatment, relapses are common.
You'll need to visit your doctor regularly for checkups and treatment of any side effects from taking corticosteroids.
Products & Services
Symptoms
Giant cell arteritis
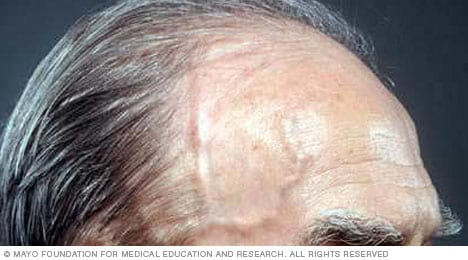
Giant cell arteritis
Giant cell arteritis causes irritation and swelling, called inflammation, of certain arteries, mainly those near the temples.
The most common symptoms of giant cell arteritis are head pain and tenderness — often severe — that usually affects both temples. Head pain can progressively worsen, come and go, or subside temporarily.
Generally, signs and symptoms of giant cell arteritis include:
- Persistent, severe head pain, usually in your temple area
- Scalp tenderness
- Jaw pain when you chew or open your mouth wide
- Fever
- Fatigue
- Unintended weight loss
- Vision loss or double vision, particularly in people who also have jaw pain
- Sudden, permanent loss of vision in one eye
Pain and stiffness in the neck, shoulders or hips are common symptoms of a related disorder, polymyalgia rheumatica. About 50 percent of people with giant cell arteritis also have polymyalgia rheumatica.
When to see a doctor
If you develop a new, persistent headache or any of the signs and symptoms listed above, see your doctor without delay. If you're diagnosed with giant cell arteritis, starting treatment as soon as possible can usually help prevent vision loss.
Causes
With giant cell arteritis, the lining of arteries becomes inflamed, causing them to swell. This swelling narrows your blood vessels, reducing the amount of blood — and, therefore, oxygen and vital nutrients — that reaches your body's tissues.
Almost any large or medium-sized artery can be affected, but swelling most often occurs in the arteries in the temples. These are just in front of your ears and continue up into your scalp.
What causes these arteries to become inflamed isn't known, but it's thought to involve abnormal attacks on artery walls by the immune system. Certain genes and environmental factors might increase your susceptibility to the condition.
Risk factors
Several factors can increase your risk of developing giant cell arteritis, including:
- Age. Giant cell arteritis affects adults only, and rarely those under 50. Most people with this condition develop signs and symptoms between the ages of 70 and 80.
- Sex. Women are about two times more likely to develop the condition than men are.
- Race and geographic region. Giant cell arteritis is most common among white people in Northern European populations or of Scandinavian descent.
- Polymyalgia rheumatica. Having polymyalgia rheumatica puts you at increased risk of developing giant cell arteritis.
- Family history. Sometimes the condition runs in families.
Complications
Giant cell arteritis can cause serious complications, including:
- Blindness. Diminished blood flow to your eyes can cause sudden, painless vision loss in one or, rarely, both eyes. Loss of vision is usually permanent.
-
Aortic aneurysm. An aneurysm is a bulge that forms in a weakened blood vessel, usually in the large artery that runs down the center of your chest and abdomen (aorta). An aortic aneurysm might burst, causing life-threatening internal bleeding.
Because this complication can occur even years after the diagnosis of giant cell arteritis, your doctor might monitor your aorta with annual chest X-rays or other imaging tests, such as ultrasound and CT.
- Stroke. This is an uncommon complication of giant cell arteritis.
Sept. 21, 2022