Overview
Genital warts are one of the most common types of sexually transmitted infections. The virus that causes the warts is called human papillomavirus (HPV). There are various types of HPV. And nearly all sexually active people will become infected with at least one type at some point.
Genital warts affect the moist tissues of the genital area. They can look like small, skin-colored bumps. The bumps may resemble cauliflower. Often, the warts are too small to be seen with your eyes.
Some strains of genital HPV can cause genital warts. Others can cause cancer. Vaccines can help protect against certain strains of genital HPV.
Symptoms
Female genital warts
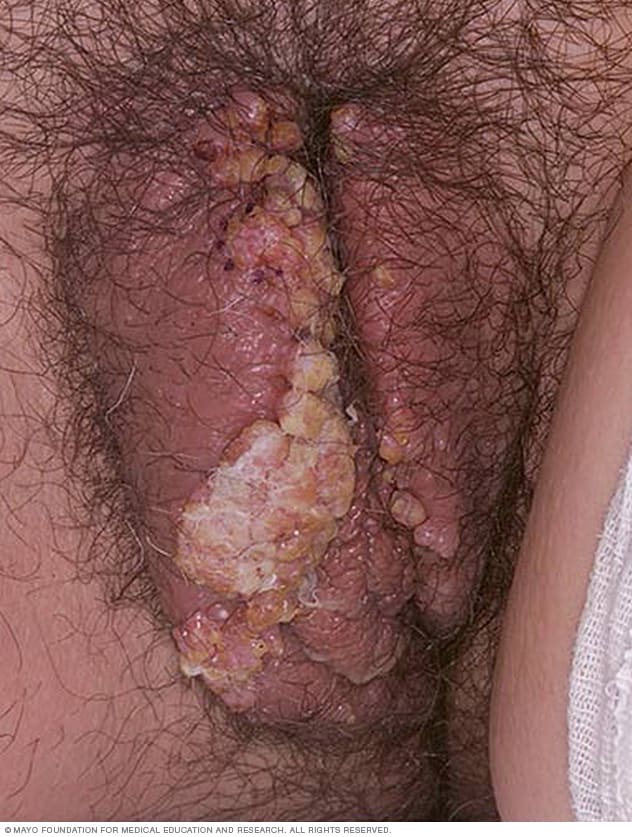
Female genital warts
Genital warts are a common sexually transmitted infection. They can appear on the genitals, in the pubic area or in the anal canal. In women, genital warts also can grow inside the vagina.
Male genital warts
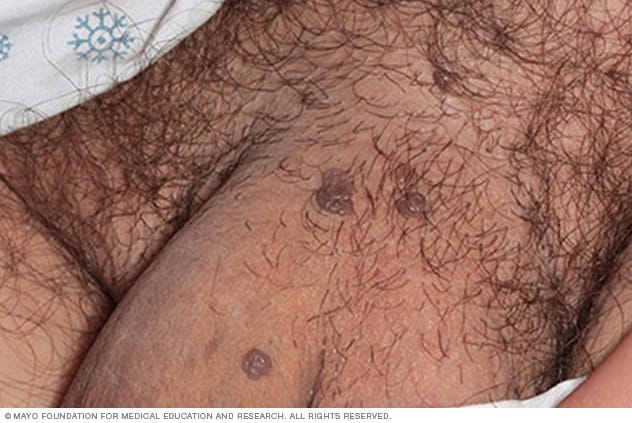
Male genital warts
Genital warts are a common sexually transmitted infection. They can appear on the genitals, in the pubic area or in the anal canal.
Genital warts can grow on the:
- Vulva.
- Walls of the vagina.
- Area between the outer part of the genitals and the anus.
- Anal canal.
- Cervix.
- Tip or shaft of the penis.
- Scrotum.
- Anus.
Genital warts also can form in the mouth or throat of a person who has had oral sex with an infected person.
The symptoms of genital warts include:
- Small swellings in the genital area that may be skin-colored or a different color.
- A cauliflower-like shape caused by a few warts close together.
- Itching or discomfort in your genital area.
- Bleeding with sex.
Genital warts can be so small and flat that you can't see them. But rarely, they can multiply into large clusters in someone with a weakened immune system.
When to see a doctor
See a health care professional if you or your partner gets bumps or warts in the genital area.
Causes
The human papillomavirus (HPV) causes warts. There are more than 40 strains of HPV that affect the genital area.
Genital warts almost always are spread through sexual contact. Even if your warts are too small to be seen, you could spread the infection to your sexual partner.
Risk factors
Most people who are sexually active get infected with genital HPV at some time. Factors that can raise your risk of infection include:
- Not getting the HPV vaccine.
- Having sex without a condom or with more than one partner.
- Having had another sexually transmitted infection.
- Having sex with a partner whose sexual history you don't know.
- Becoming sexually active at a young age.
- Having a weakened immune system, such as from HIV or medicines from an organ transplant.
Complications
An HPV infection can lead to health problems such as:
-
Cancer. Cervical cancer has been closely linked with genital HPV infection. Certain types of HPV also are linked with cancers of the vulva, anus, penis, and mouth and throat.
HPV infection doesn't always lead to cancer. But it's important for women to have regular Pap tests, which check for cancer of the cervix. Pap tests are key for those who've been infected with higher-risk types of HPV.
-
Problems during pregnancy. Rarely during pregnancy, warts can become larger. This makes it hard to urinate. Warts on the vaginal wall can hinder the stretching of vaginal tissues during childbirth. Large warts on the vulva or in the vagina can bleed when stretched during delivery.
Very rarely, a baby born to a pregnant person with genital warts get warts in the throat. The baby might need surgery to keep the airway from being blocked.
Prevention
Get the HPV vaccine to help prevent genital warts. And if you have sex, limit your number of partners. It's safest to have sex with just one partner who only has sex with you. It's also a good idea to use a condom every time you have sex. But this won't fully protect you from genital warts. That's because HPV can infect parts of the body that the condom doesn't cover.
Vaccination
In the United States, the Centers for Disease Control and Prevention (CDC) recommends routine HPV vaccination for girls and boys ages 11 and 12. But the vaccine can be given as early as age 9.
It's ideal for children to receive the vaccine before they have sexual contact.
Most often, side effects from the vaccines are mild. They include soreness where the shot was given, headaches, a low-grade fever or flu-like symptoms.
The CDC now recommends that all 11- and 12-year-olds receive two doses of HPV vaccine 6 to 12 months apart. The agency used to recommend a three-dose schedule. Younger children ages 9 and 10 and teens ages 13 and 14 also can get two doses of the vaccine. Research has shown that two doses work for children under 15.
Teens and young adults who start the vaccine series later, at ages 15 through 26, should receive three doses. The CDC recommends that the second dose be given 1 to 2 months after the first. The third dose should be given 6 months after the first.
The CDC now recommends catch-up HPV vaccinations for all people through age 26 who aren't fully vaccinated.
The U.S. Food and Drug Administration approved the use of the Gardasil 9 HPV vaccine for males and females ages 9 to 45. If you're ages 27 to 45, ask your health care team about your risks to decide if you should get the HPV vaccine.
Other HPV vaccines are offered outside of the United States. Talk with your health care team about when to get vaccinated and how many doses are needed.
Dec. 19, 2023