Diagnosis
Health care professionals often can find genital warts during a physical exam. Sometimes, a small piece of tissue needs to be removed and checked by a lab. This is called a biopsy.
Pap tests
Pap test
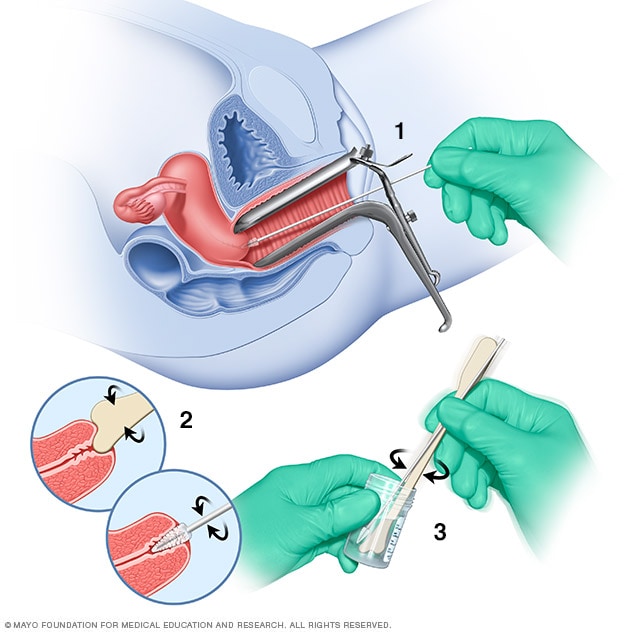
Pap test
During a Pap test, a tool called a speculum holds the vaginal walls apart. A sample of cells from the cervix is collected using a soft brush and a flat scraping device called a spatula (1 and 2). The cells are placed in a bottle that contains a solution to preserve them (3). Later, the cells are checked under a microscope.
For women, it's important to have regular Pap tests. These tests can help find changes in the vagina and cervix caused by genital warts. They also can find the early signs of cervical cancer.
During a Pap test, a device called a speculum holds open the vagina. Then, the health care professional can see the passage between the vagina and uterus, called the cervix. A long-handled tool collects a small sample of cells from the cervix. The cells are checked with a microscope for irregular changes.
HPV test
Only a few types of genital HPV have been linked to cervical cancer. A sample of cervical cells, taken during a Pap test, can be tested for these cancer-causing HPV strains.
Most often, this test is done for women age 30 and older. It isn't as useful for younger women. That's because for them, HPV usually goes away without treatment.
Treatment
If your warts don't cause discomfort, you might not need treatment. But medicine or surgery can help you clear an outbreak if you have itching, burning and pain. Treatment also can help if you're concerned about spreading the infection.
Warts often return after treatment though. And there is no treatment for the virus itself.
Medications
Genital wart treatments that can go on the skin include:
-
Imiquimod (Zyclara). This cream seems to boost the immune system's ability to fight genital warts. Do not have sexual contact while the cream is on your skin. It might weaken condoms and diaphragms and irritate your partner's skin.
One possible side effect is a change in skin color where the medicine is used. Other side effects might include blisters, body aches or pain, a cough, rashes, and fatigue.
-
Podophyllin (Podocon-25) and podofilox (Condylox). Podophyllin is a plant-based substance that destroys genital wart tissue. A health care professional puts this solution on your skin. Podofilox contains the same active compound, but you can put it on at home.
Never place podofilox inside your body. Also, this medicine isn't recommended for use during pregnancy. Side effects can include mild skin irritation, sores and pain.
- Trichloroacetic acid. This chemical treatment burns off genital warts. It also can treat warts inside the body. Side effects can include mild skin irritation, sores and pain.
- Sinecatechins (Veregen). This ointment can treat genital warts on the body and warts in or around the anus. Side effects can include a change in skin color, itching or burning, and pain.
Do not try to treat genital warts with wart removers sold in stores. These medicines aren't meant for use in the genital area.
Surgery
You might need surgery to remove larger warts or ones that don't get better with medicine. If you're pregnant, you may need surgery to remove warts that your baby could come in contact with during delivery. Surgeries for genital warts include:
- Freezing with liquid nitrogen. This also is called cryotherapy. Freezing works by causing a blister to form around the wart. As the skin heals, the warts slough off and new skin appears. You might need to repeat the treatment. The main side effects include pain and swelling.
- Electrocautery. This procedure uses an electric current to burn off warts. You might have some pain and swelling afterward.
- Surgical excision. Warts can be cut off during surgery. You'll need medicine called anesthesia that keeps you from feeling pain during this treatment. You might have pain afterward.
- Laser treatments. This approach uses an intense beam of light. It can be expensive. Most often, it's saved for warts that are extensive and tough to treat. Side effects can include scarring and pain.
Preparing for your appointment
You'll likely start by seeing your health care professional.
What you can do
Make a list of your:
- Symptoms and when they began. Describe your symptoms. If you have a sexual partner, note whether your partner has had similar symptoms.
- Sexual history. Include any situations that might have exposed you to infections. This is key if you've had sex without a condom or sex with a new partner.
- Key medical information. Include other conditions you're being treated for.
- All medicines, vitamins or other supplements you take. Include the doses.
For genital warts, some basic questions to ask your health care professional include:
- What tests do I need?
- Should I also be tested for other sexually transmitted infections?
- What treatment do you recommend, if any?
- How soon after I start treatment can I expect to get better?
- Am I contagious? How can I lower the risk of passing this infection to others?
- Should my partner be tested for this condition?
- When can I safely have sex again?
- Will my genital warts come back?
- Am I at risk of health problems related to genital warts?
- How often should I be screened for other health conditions related to genital warts?
- Are there printed materials I can have? What websites do you recommend?
Feel free to ask other questions.
What to expect from your doctor
Your health care professional is likely to ask you questions, including:
- How severe are your symptoms?
- Do you practice safe sex? Have you always done so?
- Have you recently had sex with a new partner?
- Has your partner been tested for sexually transmitted infections?
- Have you had the HPV vaccine? When?
- Are you pregnant or planning to become pregnant?
Dec. 19, 2023