Diagnosis
Endoscopy
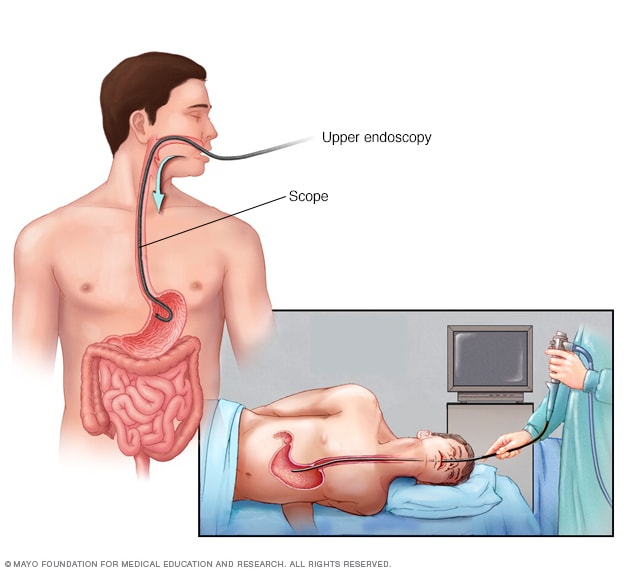
Endoscopy
An endoscopy procedure involves inserting a long, flexible tube called an endoscope down your throat and into your esophagus. A tiny camera on the end of the endoscope allows views of your esophagus, stomach and the beginning of your small intestine, called the duodenum.
Diagnosis involves the steps that your healthcare professional takes to find out if you have esophagitis. Your main healthcare professional or a specialist asks you about your symptoms and gives you a physical exam. You also may need one or more tests. These tests may include the following:
Endoscopy
Endoscopy is a test that's used to check the digestive system. A healthcare professional guides a long, thin tube equipped with a tiny camera down the throat and into the esophagus. This tool is called an endoscope. Your healthcare professional can use an endoscope to see if the esophagus looks different than usual. Small tissue samples may be taken for testing. This is called a biopsy. The esophagus may look different depending on the cause of the swelling, such as medicine-induced or reflux esophagitis. Before this test, you receive medicine that helps you relax.
Esophageal capsule
This test can be done in the healthcare professional's office. It involves swallowing a capsule attached to a string. The capsule dissolves in the stomach and releases a sponge. The healthcare professional pulls the sponge out of the mouth with the string. As the sponge is pulled out, it samples the tissues of the esophagus. This may help your healthcare professional figure out how inflamed your esophagus is without doing an endoscopy.
Barium X-ray
This test involves drinking a solution or taking a pill that contains a compound called barium. Barium coats the lining of the esophagus and the stomach so that they show up on images taken. The images can help healthcare professionals find narrowing of the esophagus and other changes in structure. The images also can help spot a hiatal hernia, tumors or other conditions that may be causing symptoms.
Laboratory tests
Small tissue samples removed during an endoscopic exam are sent to the lab for testing. Depending on the suspected cause of the condition, tests may be used to:
- Diagnose an infection caused by a bacterium, a virus or a fungus.
- Find out if allergy-related white blood cells called eosinophils have built up in the esophagus.
- Spot cells that aren't regular. Such cells may be clues of esophageal cancer or changes that raise the risk of cancer.
Treatment
Treatments for esophagitis are intended to lessen symptoms, manage complications and treat the causes of the condition. Treatment methods vary based on the cause of esophagitis.
Reflux esophagitis
Treatment for reflux esophagitis may include:
- Medicines available without a prescription. These include antacids (Maalox, Mylanta, others); medicines called H-2-receptor blockers that lower stomach acid, such as cimetidine (Tagamet HB); and medicines called proton pump inhibitors that block stomach acid and heal the esophagus, such as lansoprazole (Prevacid 24 HR) and omeprazole (Prilosec OTC), among others.
- Prescription medicines. These include prescription-strength H-2-receptor blockers and proton pump inhibitors.
- Surgery. A type of surgery called fundoplication may improve the condition of the esophagus if other treatments don't work. The surgeon wraps a portion of the stomach around the valve that separates the esophagus and stomach. This valve is called the lower esophageal sphincter. This surgery can strengthen the sphincter and prevent acid from backing up into the esophagus.
Eosinophilic esophagitis
Treatment for eosinophilic esophagitis involves staying away from the allergen that trigger symptoms. Treatment also involves easing the allergic reaction with medicines. Medicines may include:
- Proton pump inhibitors. Your healthcare professional likely will first prescribe a proton pump inhibitor. You might take one such as esomeprazole (Nexium), lansoprazole (Prevacid), omeprazole (Prilosec) or pantoprazole (Protonix).
-
Steroids. Some studies show that swallowed steroids may act on the surface tissue of the esophagus to treat eosinophilic esophagitis. One steroid called budesonide (Eohilia) comes in a liquid form. Another steroid called fluticasone is sprayed into the mouth and then swallowed.
Your healthcare professional can tell you how to swallow the steroid solution so that it coats your esophagus. Swallowing a steroid solution is much less likely to cause serious side effects compared with taking steroid pills by mouth.
-
Elimination and elemental diets. A reaction to a food allergen is likely the cause of eosinophilic esophagitis. So it may help to stop eating the food that seems to cause the allergy.
Standard allergy tests can't tell you for sure if you're allergic to a certain food. For that reason, your healthcare professional may recommend that you remove common food allergens from your diet. Then you can slowly add foods back into your diet and note when symptoms come back. This is known as an elimination diet. It needs to be done with guidance from your healthcare professional.
A more restrictive method is to remove all food from your diet for a time. Your healthcare professional replaces food with an amino acid-based formula. Over time, you slowly get back to eating food. This is called an elemental diet. It also must be done under the watch of a healthcare professional.
- Monoclonal antibodies. This type of medicine works to block the action of certain proteins in the body that cause inflammation. A monoclonal antibody called dupilumab (Dupixent) may be a treatment option for people age 12 and older with eosinophilic esophagitis. Dupilumab is given as an injection every week or every two weeks depending on your weight.
Medicine-induced esophagitis
Treatment for medicine-induced esophagitis involves not using the problem medicine when possible. It also involves lowering the risk of this condition with proper pill-taking habits. Your healthcare professional may recommend:
- Taking a different medicine that is less likely to cause medicine-induced esophagitis.
- Taking a liquid version of a medicine if possible.
- Sitting or standing for at least 30 minutes after taking a pill.
- Drinking an entire glass of water with a pill. But this option isn't right for everyone. For instance, some people need to drink less fluid because of another condition, such as kidney disease.
Infectious esophagitis
Your healthcare professional may prescribe medicine to treat an infection that causes infectious esophagitis. Medicines can help clear up infections from viruses, bacteria or fungi.
Treating common complications
A doctor called a gastroenterologist who treats digestive conditions may use medical tools to expand the esophagus. This treatment is called esophageal dilation. It tends to be used only if the esophagus becomes very narrow or if food becomes stuck in the esophagus.
During esophageal dilation, your healthcare professional guides small narrow tubes through the esophagus. Versions of these devices may be equipped with:
- A tapered tip that starts with a rounded point that gradually widens.
- A balloon that can be expanded after it's placed in the esophagus.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Depending on the type of esophagitis you have, you may lessen symptoms or stop recurring problems by following these steps:
- Do not eat foods that may make reflux worse. Consuming large amounts of certain foods or drinks may make symptoms of acid reflux worse. These can include alcohol, drinks with caffeine, chocolate and mint-flavored foods.
- Use proper pill-taking habits. Take a pill with plenty of water and before eating a meal. Don't lie down for at least 30 minutes after taking a pill.
- Lose extra weight. Talk with your healthcare professional about a diet and exercise routine to help you lose weight and stay at a healthy weight.
- If you smoke, quit. You can ask your healthcare professional to help you end a smoking habit.
- Try not to stoop or bend, especially soon after eating.
- Do not lie down after eating. Wait at least three hours after eating to lie down or go to bed.
- Raise the head of your bed. Place wooden blocks under your bed to raise the head. Aim to raise it 6 to 8 inches (15 to 20 centimeters). If it's not possible to elevate your bed, place a wedge between your mattress and box spring. This raises your body from the waist up. Raising your head by using only pillows doesn't work.
Alternative medicine
No complementary or alternative medicines are proved to treat esophagitis. Still, some of these treatments may help ease heartburn or reflux symptoms. Options may include ginger, chamomile and slippery elm. But supplements such as these do not replace the treatment that your healthcare professional recommends. Talk with your healthcare professional before you try any alternative treatment for GERD.
Preparing for your appointment
Get emergency care if you have severe chest pain that lasts more than a few minutes. Also get emergency care if you think you have food lodged in your esophagus or you can't swallow.
If you have other symptoms of esophagitis, you'll likely start by seeing your main healthcare professional. You may be referred to a doctor who checks for and treats digestive conditions, called a gastroenterologist. Or you may be referred to an allergy doctor, called an allergist. Preparing for your appointment with your healthcare professional or a specialist can help you make the best use of your time.
What you can do
Make a list ahead of time, including:
- Your symptoms, including any that may not seem related to pain, trouble swallowing or reflux.
- Key personal information, including any major stresses or recent life changes.
- Medicines that you're taking, including vitamins and other supplements.
- Family history of allergies and conditions of the esophagus or stomach.
- Questions to ask your healthcare professional.
List questions from most important to least important in case time runs out. If you think you have symptoms of esophagitis, you may ask some of the following:
- What tests do I need to find out if I have esophagitis?
- Do I need to do anything special to prepare for these tests?
- How long will it take to find out the results of tests?
- What treatments are available, and which do you recommend?
- How will we know if the treatment is working?
- Will I need follow-up tests?
- What steps can I take on my own to prevent symptoms from happening again?
- I have other medical conditions. How can I best manage these conditions together?
What to expect from your doctor
Your healthcare professional is likely to ask you many questions. Being ready to answer them may save time to go over points you want to spend more time on. Your healthcare professional may ask:
- How bad is your pain or discomfort?
- Do you have trouble swallowing?
- How often do you notice symptoms?
- Does anything seem to trigger your symptoms or make them worse, such as certain foods?
- Does anything ease symptoms, such as taking antacids available without a prescription or not eating certain foods?
- Are symptoms worse at certain times of the day?
- Do your symptoms start soon after taking any medicines? If so, which medicines?
- Do you have any allergies, and do you take any allergy medicine?
- Have you ever had food get stuck in your throat after swallowing?
- Do you ever have food come back up after swallowing?
- Do you have a family history of digestive problems?
What you can do in the meantime
If you know that certain foods trigger your symptoms or make them worse, don't eat those foods. Common triggers include spicy foods, drinks with caffeine and alcohol. Taking antacids sold without a prescription may ease your symptoms for a short time.
If you think that your symptoms are related to a prescription medicine, don't stop taking the medicine. Talk with healthcare professional first. If you can, limit the use of medicines you take without a prescription that could be causing symptoms. When you take pills, drink a glass of water. Don't lie down for at least 30 minutes after you take a pill.
Oct. 29, 2024