Overview
Cluster headache is a rare and severe type of headache that causes intense pain in or around the eye on one side of the head. It's typically the most painful type of headache. You may have several headaches over short periods of time. This is known as a cluster. Cluster periods can last from weeks to months. Then they may stop for months or years.
Cluster headache is rare. Treatments can shorten cluster headache attacks and lessen the pain. Also, medicines can reduce the number of cluster headaches.
Symptoms
Common symptoms
Cluster headache
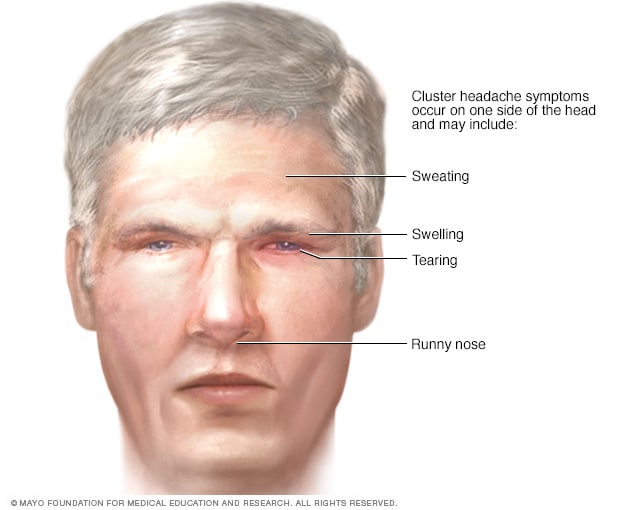
Cluster headache
Cluster headaches usually come close together in a group. Possible symptoms include severe pain in or around one eye or on one side of the head. There may be tears and a stuffy and runny nose on the side of the head that hurts.
A cluster headache usually starts quickly with no warning. But some people might first have migraine-like nausea and aura. Aura may include flashes of light and tingling in the tongue.
Common symptoms during a cluster headache include:
- Extreme sharp or stabbing pain, usually in, behind or around one eye. The pain can spread to other areas of the face, head and neck.
- Pain on one side of the head in a single cluster. Pain can switch to the other side in another cluster.
- Restlessness.
- A lot of tears.
- Forehead or facial sweating.
On the side of the head that hurts, common symptoms include:
- Redness of the eye.
- Stuffy or runny nose.
- Swelling around the eye.
- Drooping eyelid.
Because the pain of a cluster headache can be so bad, those who have one are likely to pace or sit and rock back and forth.
Cluster periods
A cluster period usually lasts for several weeks to months. Each cluster period may start at about the same time of year and last about the same length of time. For example, cluster periods can come during certain seasons, such as every spring or every fall.
For most people with cluster headaches, the cluster period lasts from one week to a year. Then there's a pain-free period, known as remission, for three months or longer before the next cluster headache comes. This is known as episodic cluster headache.
Cluster periods may go on for more than a year. Pain-free periods might last less than one month. If a cluster period lasts a year without stopping, it's called chronic cluster headache.
During a cluster period:
- Headaches usually come every day, often several times a day.
- A single attack can last from 15 minutes to 3 hours, but more often lasts 30 to 45 minutes.
- The attacks often occur at the same time each day.
- Most attacks occur at night, usually 1 to 2 hours after bedtime. Cluster headache can wake people from sleep.
The pain usually ends as suddenly as it begins. After attacks, most people are pain-free but exhausted.
When to see a doctor
See a healthcare professional if you've just started to have cluster headaches. Your care team can rule out other illnesses and suggest treatment.
Even bad headache pain isn't usually the result of another disease. But headaches can sometimes mean a serious medical condition. This can include a brain tumor or a tear of a weakened blood vessel, known as a dissection.
Also, if you have a history of headaches, see your healthcare professional if there's a change in how they feel or how often they happen.
Seek emergency care if you have any of these symptoms:
- A severe headache that comes on suddenly, often like a clap of thunder.
- A headache with a fever, nausea or vomiting, a stiff neck, confusion, seizures, numbness or trouble speaking. These might point to a stroke, meningitis, encephalitis, a brain tumor or other conditions.
- A headache after a head injury, especially if it gets worse, even if it was a minor fall or bump.
- A sudden, severe headache unlike any other.
- A headache that worsens over days and changes in pattern.
Causes
Experts don't know what causes cluster headache. Cluster headache patterns suggest a link to the area of the brain that helps run the body's biological clock, known as the hypothalamus.
Cluster headache triggers
There are several cluster headache triggers. The most common are drinking alcohol and smoking. Other triggers might include weather changes and certain medicines.
Risk factors
Risk factors for cluster headache include:
- Sex. People assigned male at birth may be more likely to have cluster headaches than people assigned female. Recent studies suggest that people assigned female at birth may be misdiagnosed with a different headache disorder such as migraine or other heath condition such as sinusitis.
- Age. Most people who develop cluster headaches are between 20 and 50 years old. But the condition can start at any age.
- Smoking. Many people who get cluster headaches are smokers. But quitting smoking usually doesn't stop the headaches.
- Alcohol use. If you have cluster headaches, drinking alcohol during a cluster period may increase the risk of an attack.
- Family history. A parent, brother or sister with cluster headache might increase the risk.
Aug. 12, 2025