Diagnosis
 Acoustic neuroma ear exam at Mayo Clinic
Acoustic neuroma ear exam at Mayo Clinic
A thorough physical exam, including an ear exam, is often the first step in acoustic neuroma diagnosis and treatment.
An acoustic neuroma, now called vestibular schwannoma, may be difficult to diagnose in the early stages since the symptoms develop gradually and can be overlooked. Common symptoms such as hearing loss also are associated with many other middle and inner ear issues.
After asking questions about your symptoms, a member of your healthcare team conducts an ear exam. You may need the following tests:
- Hearing test. Known as an audiogram or audiometry, this test is conducted by a hearing specialist called an audiologist. During the test, sounds of various tones are directed to one ear at a time. You indicate each time you hear the sound. Each tone is repeated at fainter levels to find out when you can barely hear. The audiologist also may use words to test your hearing. A hearing test by itself can't confirm an acoustic neuroma. But it is often one of the first steps healthcare teams use to investigate hearing loss or ringing in the ears. If the test shows certain patterns, an MRI may be ordered to look for an acoustic neuroma.
- Imaging. MRI with contrast is usually used to diagnose an acoustic neuroma. This imaging test can detect tumors as small as 1 to 2 millimeters in diameter. If MRI is not available or you can't have an MRI scan, a CT scan may be done. However, CT scans may miss small tumors.
Because other conditions, such as Meniere's disease, can cause similar symptoms, testing is especially important. A hearing test helps identify patterns of hearing loss, while imaging like MRI or CT can detect whether a tumor is present. Together, these evaluations help doctors to accurately distinguish between the two conditions.
More Information
Treatment
 Acoustic neuroma surgery at Mayo Clinic
Acoustic neuroma surgery at Mayo Clinic
Surgical removal of the tumor by an experienced neurosurgeon is one of many acoustic neuroma treatment options at Mayo Clinic.
Treatment for an acoustic neuroma, now called vestibular schwannoma, usually cannot bring back hearing that has already been lost. But if the tumor is found early, surgery or radiation may sometimes help keep the hearing you have. If much of your hearing is already gone, your care team may talk with you about ways to manage the loss. These options may include hearing aids and cochlear implants. In rare cases, a special device called an auditory brainstem implant, which sends sound signals directly to the brain, may help.
Your acoustic neuroma treatment may vary, depending on:
- The size and growth rate of the acoustic neuroma.
- Your overall health.
- Your signs and symptoms.
There are three treatment approaches for acoustic neuroma: monitoring, surgery and radiation therapy.
Monitoring
You and your healthcare team may decide to monitor an acoustic neuroma if it is small and not growing or if it is growing slowly. Also called watchful waiting, this may be an option if the acoustic neuroma causes few or no symptoms. Monitoring also may be recommended if you're an older adult or if you're not a good candidate for more aggressive treatment such as surgery.
While being monitored, you'll need regular imaging and hearing tests, usually every 6 to 12 months. These tests can determine whether the tumor is growing and how quickly. If the scans show the tumor is growing or if the tumor causes worse symptoms, you may need to have surgery or radiation.
Surgery
You may need surgery to remove an acoustic neuroma, especially if the tumor:
- Continues to grow.
- Is very large.
- Causes symptoms.
Surgeons can use different techniques to remove an acoustic neuroma. Usually, acoustic neuroma surgery involves a craniotomy. This is a surgery that removes part of the skull. Several different types of craniotomy approaches may be used to remove an acoustic neuroma. The approach depends on the tumor's size, your hearing and other individual factors.
Surgeons use three main approaches for acoustic neuroma craniotomy surgery:
- Retrosigmoidal. Also called suboccipital, this is the most common approach, made through an opening behind the ear. It can be used for tumors of many sizes and sometimes allows hearing preservation.
- Translabyrinthine. This is done through the inner ear bone. This approach sacrifices hearing but gives the surgeon a wide view to safely remove larger tumors and protect the facial nerve. This may be recommended when significant hearing is already lost.
- Middle fossa. This is done through a small opening above the ear. It's often chosen for small tumors when hearing preservation is the main goal.
The main goals of surgery are to remove as much of the tumor as possible and to preserve the facial nerve, which controls the muscles in the face. In some cases, complete removal is not possible. If the tumor is very close to the brainstem or facial nerve, the surgeon may leave a small portion behind to avoid serious complications.
Before surgery, you may have a brain MRI. MRI is the preferred imaging test because it shows the exact size and location of the tumor and its relationship to nearby nerves and brain structures. This information helps your surgeon plan the safest and most effective approach.
Surgery is done under general anesthesia. The tumor is removed either through the inner ear or through an opening in the skull, depending on the chosen surgical approach.
As with any surgery, there are some risks. Hearing loss on the side of the tumor is possible. Balance issues are common right after the procedure, but these usually improve with time. In some cases, the hearing, balance or facial nerves may be irritated or damaged during surgery, which can lead to lasting changes.
Complications of surgery may include:
Recovery after acoustic neuroma surgery varies depending on the tumor's size and the surgical approach. Hospital stays are usually 3 to 7 days. You may need several weeks at home to rest. Balance troubles often get better within weeks to months as the brain adapts. Fatigue can last for several months. Full recovery may take weeks to months, though some nerve-related changes, such as hearing loss, are permanent.
Radiation therapy
Gamma Knife stereotactic radiosurgery unit
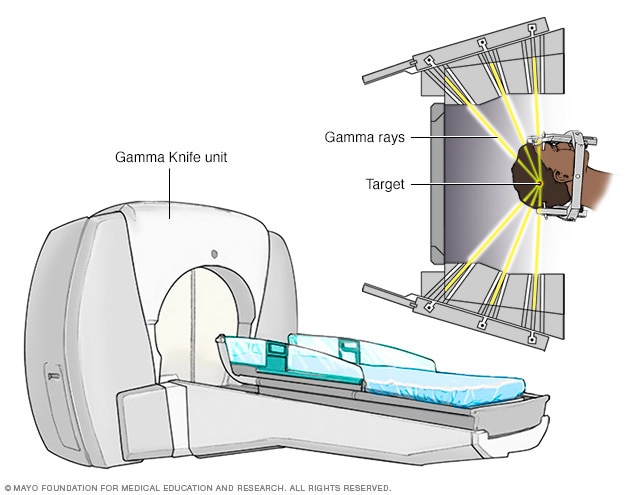
Gamma Knife stereotactic radiosurgery unit
Stereotactic radiosurgery technology uses many small gamma rays to deliver a precise dose of radiation to the target.
There are several types of radiation therapy used to treat an acoustic neuroma.
- Stereotactic radiosurgery is a form of highly focused radiation therapy often used to treat small acoustic neuromas, usually less than 2.5 centimeters in size. That's about the size of a peanut. It also may be recommended if you are an older adult or if health conditions make surgery too risky.
- Fractionated stereotactic radiotherapy, also called SRT, is another type of radiation treatment for acoustic neuroma. It gives small doses of radiation over several sessions to slow the tumor's growth. This helps protect nearby healthy brain tissue.
- Proton beam therapy is another kind of radiation treatment for acoustic neuroma. It uses tiny particles called protons to target the tumor. This method lowers the amount of radiation that reaches healthy areas of the brain.
How is Gamma Knife surgery used to treat acoustic neuroma?
Gamma Knife is one of the most common forms of stereotactic radiosurgery. It uses many small beams of gamma rays to deliver a precise dose of radiation directly to the tumor. Other systems, such as CyberKnife and linear accelerator based radiosurgery, work in a similar way by shaping multiple beams of radiation so they meet at the tumor. This allows treatment without an incision and helps protect the surrounding brain and nerves.
The goal of radiosurgery is to stop the tumor from growing, preserve facial nerve function, and in some cases, preserve hearing. The effects happen slowly, so it may take weeks, months or even years before changes are seen. Your healthcare team monitors your progress with follow-up MRI scans and hearing tests.
Risks and side effects of radiosurgery may include:
- Changes in hearing, including hearing loss.
- Ringing in the ear, also called tinnitus.
- Weakness or numbness in the face.
- Poor balance.
- The possibility that the tumor continues to grow and needs additional treatment.
Outcomes after surgery or radiosurgery for acoustic neuroma
Research looking at many studies shows that both surgery and radiosurgery are effective treatments for acoustic neuroma. Here's what people should know:
- Tumor control. Both surgery and radiosurgery are effective at controlling tumor growth. For smaller tumors, the results are similar. For larger tumors, surgery offers better long-term control.
- Hearing. Hearing loss is common after either treatment. Radiosurgery tends to preserve hearing in more people than surgery does, especially when the tumor is small.
- Facial nerve function. Right after surgery, some people may experience facial weakness, though most recover over time. Radiosurgery is more likely to preserve facial nerve function overall.
- Other symptoms. Surgery is more likely to improve symptoms such as tinnitus, vertigo, imbalance and facial numbness. Radiosurgery is less likely to improve these symptoms but generally causes fewer new nerve problems.
Can acoustic neuroma grow back after treatment?
Yes, acoustic neuroma sometimes can return after treatment. The risk depends on how it was treated.
- After surgery. If the tumor is removed completely, regrowth is rare, usually less than 5%. But when part of the tumor is left behind to protect nearby nerves or the brainstem, the chance of regrowth is between 10% and 20%.
- After radiosurgery. Treatments such as Gamma Knife and CyberKnife are designed to stop the tumor from growing, not to remove it. Most tumors remain stable or shrink, but in about 5% to 10% of cases, the tumor may continue to grow or regrow later.
Follow-up after acoustic neuroma treatment
Regular MRI scans are recommended after either surgery or radiosurgery. These scans help check whether the tumor is stable or if additional treatment is needed.
Can acoustic neuroma shrink on its own?
Most acoustic neuromas grow slowly. Some stop growing for years. Rarely, studies have shown that an acoustic neuroma may shrink slightly without treatment. But this is not common, and it's not possible to predict which tumors might do this. For this reason, regular MRI scans are important if you and your care team choose monitoring, also called observation or watchful waiting, for acoustic neuroma.
What are the risks of untreated acoustic neuroma?
If left untreated, an acoustic neuroma can continue to grow and cause permanent complications. These include hearing loss (usually in one ear), ringing in the ear and problems with balance. Larger tumors may press on nearby nerves, leading to facial numbness or weakness. In rare cases, very large tumors can block the flow of cerebrospinal fluid and cause hydrocephalus, a dangerous buildup of fluid and pressure in the brain.
Supportive therapy
In addition to treatment to remove or stop the growth of the tumor, supportive therapies can help reduce your symptoms. The therapies help with dizziness, trouble with balance or other complications. For hearing loss, you can use cochlear implants or other treatments.
 Supportive care for acoustic neuromas at Mayo Clinic
Supportive care for acoustic neuromas at Mayo Clinic
Supportive care including balance therapy, physical therapy, occupational therapy and hearing assistance is part of the comprehensive acoustic neuroma treatment at Mayo Clinic.
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
No natural remedies, vitamins or lifestyle changes can shrink or cure an acoustic neuroma, now called vestibular schwannoma. Because this tumor grows from Schwann cells on the nerve responsible for hearing and balance, it requires medical monitoring and sometimes treatment such as surgery or radiosurgery. Healthy habits such as reducing noise exposure, managing stress, eating well and staying active can support overall wellness, but they do not stop tumor growth.
Coping and support
Dealing with the possibility of hearing loss and facial paralysis can be quite stressful. Deciding which treatment approach is right for you also can be challenging. These suggestions may help:
- Educate yourself about acoustic neuromas. The more you know, the better prepared you can be to make choices about treatment. Besides talking to your healthcare team and your audiologist, you may want to talk to a counselor or social worker. Or you may find it helpful to talk to other people who've had an acoustic neuroma. It may help to learn more about their experiences during and after treatment.
- Maintain a strong support system. Family and friends can help you as you go through this challenging time. You also might find the concern and understanding of other people with an acoustic neuroma especially comforting. A member of your healthcare team or a social worker may be able to put you in touch with a support group. Or you can find an in-person or online support group through the Acoustic Neuroma Association.
Preparing for your appointment
You first may see a healthcare professional. This person may refer you to a doctor trained in ear, nose and throat conditions. Or you may be referred to a doctor trained in brain and nervous system surgery, known as a neurosurgeon. Here's some information to help you get ready for your appointment.
What you can do
When you make the appointment, ask if there's anything you need to do in advance, such as fasting before having a specific test. Make a list of:
- Write down any symptoms you're experiencing, including any that may seem unrelated to the reason for which you scheduled the appointment.
- Make a list of all medicines, vitamins or supplements that you're taking.
- Ask a family member or friend to join you, if possible. Sometimes it can be hard to remember all the information provided to you during an appointment. Someone who comes with you may remember something that you missed or forgot.
- Write down questions to ask your healthcare team.
Preparing a list of questions will help you make the most of your time. For an acoustic neuroma, some basic questions to ask include:
- What is likely causing my symptoms?
- Are there any other possible causes for my symptoms?
- What kinds of tests do I need?
- What treatment options are available?
- Which one do you recommend for me?
- What is the likelihood of side effects from each treatment option?
- What happens if I do nothing?
- Are there any brochures or other printed material that I can take home with me? What websites do you recommend visiting?
In addition to the questions that you've prepared, don't hesitate to ask any that come up during your appointment.
What to expect from your doctor
You'll be asked some questions. Being ready to answer them can give you more time to go over any points that you need to clarify. You may be asked:
- When did your symptoms begin?
- Have your symptoms been constant or off and on?
- How bad are your symptoms?
- Do you have any family members with an acoustic neuroma?
- Can you hear with the affected ear? For example, can you use that ear on the phone? Does that ear help you tell where sound is coming from?
- Do you have regular headaches currently or have you had them in the past?
Nov. 11, 2025