Overview
Carotid artery
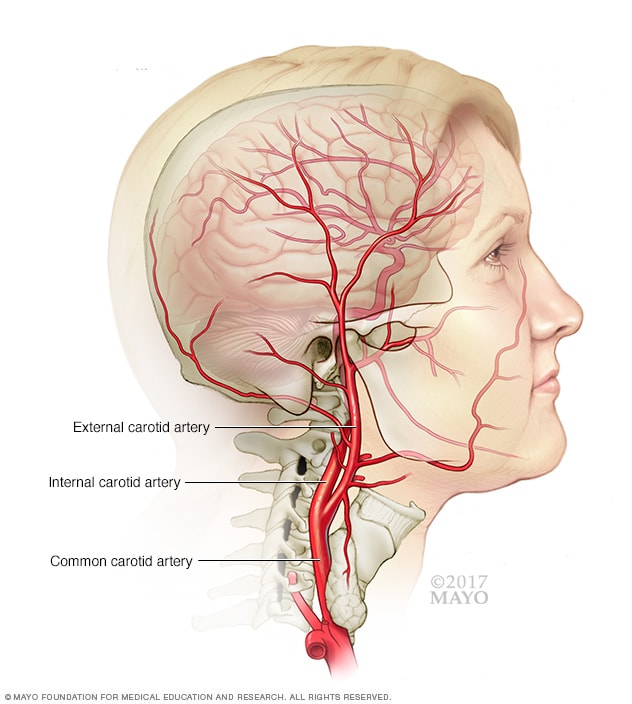
Carotid artery
The carotid arteries are a pair of blood vessels. There's one on each side of the neck. The carotid arteries deliver blood to the brain and head.
Carotid angioplasty (kuh-ROT-id AN-jee-o-plas-tee) and stenting are procedures that open clogged arteries to restore blood flow to the brain. They're often performed to treat or prevent strokes.
The carotid arteries are located on each side of your neck. These are the main arteries supplying blood to your brain. They can be clogged with fatty deposits (plaque) that slow or block blood flow to the brain — a condition known as carotid artery disease — which can lead to a stroke.
The procedure involves temporarily inserting and inflating a tiny balloon into the clogged artery to widen the area so that blood can flow freely to your brain.
Carotid angioplasty is often combined with another procedure called stenting. Stenting involves placing a small metal coil (stent) in the clogged artery. The stent helps prop the artery open and decreases the chance of it narrowing again. Carotid angioplasty and stenting may be used when traditional carotid surgery (carotid endarterectomy) isn't possible, or it's too risky.
Products & Services
Why it's done
Carotid angioplasty and stenting may be appropriate stroke treatments or stroke-prevention options if:
- You have a carotid artery with a blockage of 70% or more, especially if you've had a stroke or stroke symptoms, and you aren't in good enough health to undergo surgery — for example, if you have severe heart or lung disease or had radiation for neck tumors
- You have already had a carotid endarterectomy and are experiencing new narrowing after surgery (restenosis)
- The location of the narrowing (stenosis) is difficult to access with endarterectomy
In some cases, carotid endarterectomy may be a better choice than angioplasty and stenting to remove the buildup of fatty deposits (plaque) clogging the artery. You and your doctor will discuss which procedure is safest for you.
Risks
With any medical procedure, complications might happen. Here are some of the possible complications of carotid angioplasty and stenting:
-
Stroke or ministroke (transient ischemic attack, or TIA). During angioplasty, blood clots that may form can break loose and travel to your brain. You'll receive blood thinners during the procedure to reduce this risk.
A stroke can also occur if plaque in your artery is dislodged when the catheters are being threaded through the blood vessels.
- New narrowing of the carotid artery (restenosis). A major drawback of carotid angioplasty is the chance that your artery will narrow again within months of the procedure. Special drug-coated stents have been developed to reduce the risk of restenosis. Medications are prescribed after the procedure to decrease the risk of restenosis.
- Blood clots. Blood clots can form within stents even weeks or months after angioplasty. These clots may cause a stroke or death. It's important to take aspirin, clopidogrel (Plavix) and other medications exactly as prescribed to decrease the chance of clots forming in your stent.
- Bleeding. You may have bleeding at the site in your groin or wrist where catheters were inserted. Usually this may cause a bruise, but sometimes serious bleeding occurs and may require a blood transfusion or surgical procedures.
How you prepare
Before a scheduled angioplasty, your doctor reviews your medical history and performs a physical exam. You may also have one or more of the following examinations:
- Ultrasound. A scanner passes over the carotid artery to produce images using sound waves of the narrowed artery and of the blood flow to the brain.
- Magnetic resonance angiography (MRA) or computerized tomography angiography (CTA). These exams provide highly detailed images of blood vessels by using either radiofrequency waves in a magnetic field or by using X-rays with contrast material.
- Carotid angiography. During this exam, contrast material (visible on X-rays) is injected into an artery to better see and examine the blood vessels.
Food and medications
You'll receive instructions on what you can or can't eat or drink before angioplasty. Your preparation may be different if you're already staying at the hospital before your procedure.
The night before your procedure:
- Follow your doctor's instructions about adjusting your current medications. Your doctor may instruct you to stop taking certain medications before angioplasty, particularly if you take certain diabetes medications, nonsteroidal anti-inflammatory drugs (NSAIDs) or blood thinners.
- Take approved medications with only small sips of water.
- Arrange for transportation home. Angioplasty may require an overnight hospital stay, and you won't be able to drive yourself home the next day because of lingering effects of the sedative.
What you can expect
Carotid angioplasty is considered a nonsurgical procedure because it's less invasive than surgery. Your body isn't cut open except for a very small nick in a blood vessel in your groin.
Most people don't need general anesthesia and stay awake during the procedure. However, some people may not stay awake based on their anesthesia and how sleepy they feel. You'll receive fluids and medications through an IV catheter to help you relax.
Before the procedure
- You're taken to an X-ray imaging room and asked to lie on a procedure bed. You'll rest your head in a cup-shaped area to help you remain comfortable and still while pictures of the carotid artery are taken.
- Your groin is shaved and prepared with antiseptic solution, and a sterile drape is placed over your body.
- A local anesthetic is injected into your groin to numb the area.
- Small electrode pads are placed on your chest to monitor your heart rate and rhythm during the procedure.
During the procedure
Carotid angioplasty
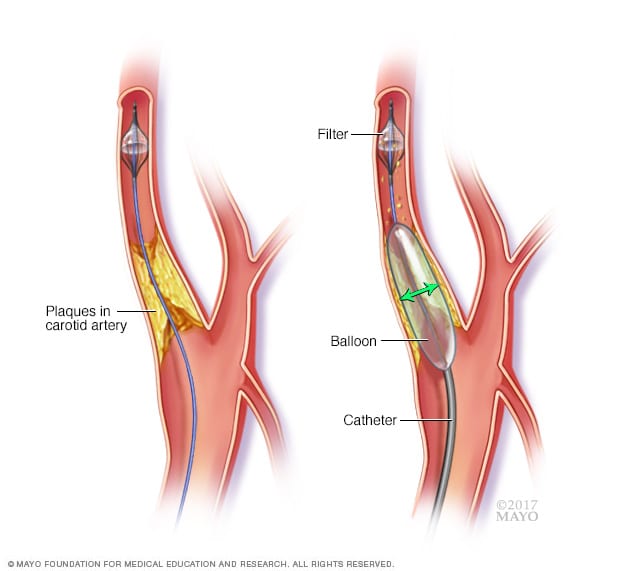
Carotid angioplasty
In carotid angioplasty, a surgeon sends a long, hollow tube, known as a catheter, through the arteries to the narrowed carotid artery in the neck. The surgeon puts in a filter to catch any debris that may break off during the procedure. Then, the surgeon inflates a tiny balloon at the end of the tube to open the narrowed area.
Carotid stenting
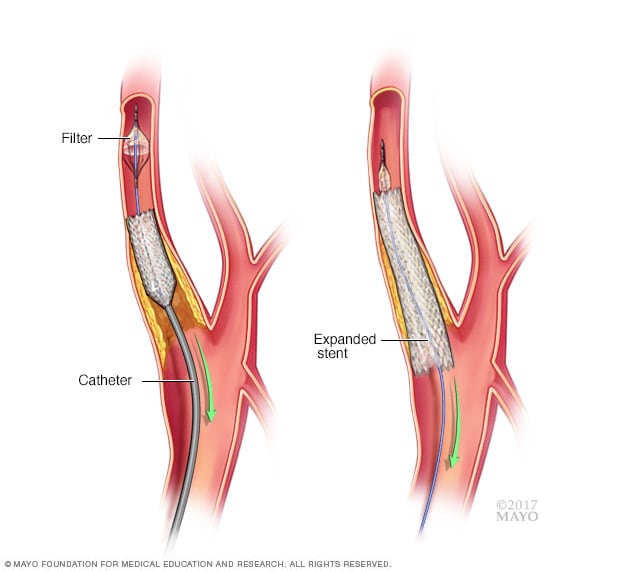
Carotid stenting
In carotid stenting, a surgeon sends a long, hollow tube, known as a catheter, through the arteries to the narrowed carotid artery in the neck. The surgeon then puts a small wire mesh coil, known as a stent, into the vessel to keep the artery from narrowing again. Finally, the surgeon removes the tube and the filter that was used to catch debris that might have broken off during the procedure.
Once you're sedated, your doctor makes a puncture in an artery, usually the femoral artery in the groin area. The following describes the angioplasty and stenting procedure.
- A small tube (sheath) is placed into the artery. A catheter with a balloon tip is then threaded through the tube to the narrowing in the carotid artery under X-ray guidance. You won't feel the catheter passing through the arteries because the insides of arteries don't have nerve endings.
- Contrast material is injected into the carotid artery through the catheter. The contrast material may cause a temporary warm feeling on one side of your face. Contrast material provides a detailed view of the narrowed artery and blood flow to the brain.
- A filter is placed in the artery. The filter, called an embolic protection device, is inserted beyond the narrowing to catch any debris that may break off from the narrowed area of artery during the procedure.
- The balloon tip is threaded into the narrowed area and inflated to push the plaque to the side and widen the vessel.
- A small metal mesh tube (stent) may be placed in the newly opened vessel. The expanded stent provides support that helps prevent the artery from narrowing again. The stent may be coated in a drug that is released slowly over time to help prevent restenosis.
- The filter, sheath, catheter and balloon are removed. Pressure is applied to the small catheter insertion site to prevent bleeding.
When the procedure is done, you lie still in one position while pressure is applied to the site to stop bleeding. You generally won't have stitches, but a dressing is applied to cover the small incision site. You'll then be taken to the recovery area.
After the procedure
To avoid bleeding from the catheter insertion site, you need to lie relatively still for several hours. You'll be either in the recovery area or in your hospital room. After the procedure, you may receive an ultrasound of your carotid artery. Most people are discharged from the hospital within 24 hours after the procedure.
The catheter site may remain tender, swollen and bruised for a few days. There may be a small area of discoloration or a small lump in the area of the puncture. You may take acetaminophen (Tylenol, others) in the recommended dose as needed for discomfort, or other medication as prescribed by your doctor.
You may need to avoid strenuous activity and heavy lifting for 24 hours after the procedure.
Results
For most people, carotid angioplasty and stenting increase blood flow through the previously blocked artery and reduce the risk of stroke.
Seek emergency medical care if your signs and symptoms return, such as trouble walking or speaking, numbness on one side of your body, or other symptoms similar to those you had before your procedure.
Carotid angioplasty and stenting aren't appropriate for everyone. Your doctor can determine if the benefits outweigh the potential risks.
Because carotid angioplasty is newer than traditional carotid surgery, long-term results are still under investigation. Talk to your doctor about what results you might expect and what type of follow-up is needed after your procedure.
Lifestyle changes will help you maintain your good results:
- Don't smoke.
- Lower your cholesterol and triglyceride levels.
- Maintain a healthy weight.
- Control other conditions, such as diabetes and high blood pressure.
- Exercise regularly.