Oct. 13, 2017
Data from the Centers for Disease Control and Prevention indicate that the prevalence of adulthood obesity in the United States, as defined by a body mass index of 30 kg/m2 or more, has increased steadily — from 12.7 percent in 1980 to 34.9 percent in 2012.
Obesity is a major risk factor for idiopathic intracranial hypertension (IIH), a condition of increased intracranial pressure of unknown cause that often produces papilledema and vision loss. IIH occurs most typically in women in their childbearing years who are obese.
John J. Chen, M.D., Ph.D., and a research team from Ophthalmology at Mayo Clinic's campus in Rochester, Minnesota, wondered whether the incidence of IIH had risen in parallel with the epidemic of obesity. "Although we know that obesity is a large risk factor for IIH, there have been no studies evaluating whether the incidence of IIH is rising with the increase in obesity," says Dr. Chen.
Much of the knowledge on the incidence of IIH came from a prior study from the Rochester Epidemiology Project, published in the Archives of Neurology in 1993, which demonstrated an incidence of 1.0 per 100,000 people from 1976 to 1990. "Our goal was to re-evaluate that Rochester Epidemiology Project data to determine if the incidence of IIH mirrors the large rise in obesity over the past 20 years," says Dr. Chen.
The research team reviewed medical records of all patients diagnosed in Olmsted County, Minnesota, with IIH, intracranial hypertension, pseudotumor cerebri or papilledema between Jan. 1, 1990, and Dec. 31, 2014.
Patients were classified as having IIH if they met the modified Dandy criteria, which included:
- Signs and symptoms of increased intracranial pressure
- No localizing neurological finding except cranial nerve VI palsies
- Normal neuroimaging results
- Lumbar puncture opening pressure of more than 250 mm H20 with normal cerebrospinal fluid constituents
- No other apparent cause
Patients with papilledema and borderline opening pressures (200 to 250 mm H20) also were included in the study.
Rates increase in parallel
The research team identified 63 new cases of IIH, yielding an overall age- and sex-adjusted annual incidence of 1.8 per 100,000 people (95 percent confidence interval, 1.3 to 2.2) between 1990 and 2014. This was double the incidence found in the original incidence study from 1976 to 1990.
In the current study period, the annual incidence increased from 1.0 per 100,000 (1990 to 2001) to 2.4 per 100,000 (2002 to 2014; P = 0.007). The incidence of IIH was 3.3 per 100,000 in women and 0.3 per 100,000 in men (P ≤ 0.001). In women ages 15 to 44 years who are obese, the incidence was 22.0 per 100,000 compared with 6.8 per 100,000 among all women in the same age group.
Idiopathic intracranial hypertension incidence and obesity rates in Minnesota
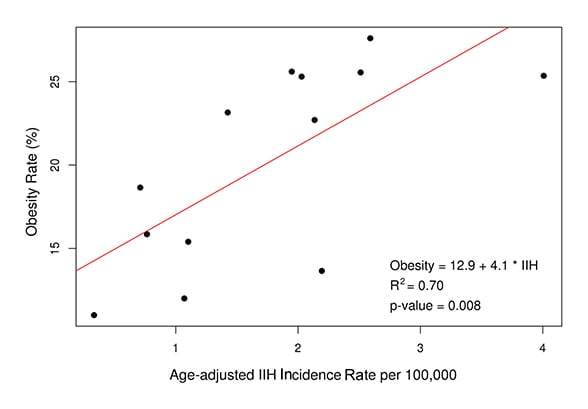
Idiopathic intracranial hypertension incidence and obesity rates in Minnesota
In this correlation between age-adjusted idiopathic intracranial hypertension (IIH) incidence and obesity rates in Minnesota (R2 = 0.70, P = 0.008), each point represents two-year intervals. The obesity rates increased consistently throughout the time period of the study and corresponded to an increase in the incidence of IIH. Graph reprinted with permission from Ophthalmology.
The increase in incidence of IIH mirrored the increase in obesity during this time period, with a strong correlation between IIH incidence rates and obesity rates in Minnesota (R2 = 0.70, P = 0.008). Data from the Centers for Disease Control and Prevention indicate that the obesity rate in Minnesota in 1990 was less than 10 percent; it increased to 28 percent by 2014. Olmsted County mirrored this trend and now has an adulthood obesity of 27 percent.
"Our study shows that the incidence rates of IIH and obesity have risen in parallel since 1990," says Dr. Chen. "There is no sign of obesity rates declining, so recognizing and treating patients with IIH promptly are of increasing importance."
Study results were published in Ophthalmology in 2017.
For more information
Centers for Disease Control and Prevention. Obesity trends among U.S. adults between 1985 and 2010.
Radhakrishnan K, et al. Idiopathic intracranial hypertension (pseudotumor cerebri): Descriptive epidemiology in Rochester, Minnesota, 1976 to 1990. Archives of Neurology. 1993;50:78.
Centers for Disease Control and Prevention. Community profile: Olmsted County, Minnesota — Obesity prevention.
Kilgore KP, et al. Re-evaluating the incidence of idiopathic intracranial hypertension in an era of increasing obesity. Ophthalmology. 2017;124:697.
Chen JJ. Palpating the brain with MR elastography to detect raised intracranial pressure. Medical Professional Video Center. Mayo Clinic. 2017.