Diagnosis
During a physical exam, your healthcare professional asks about your symptoms and looks for swelling or lumps on your thumb joints.
Your healthcare professional might hold your joint while pressing your thumb against your wrist bone. If this causes a grinding sound, pain or a gritty feeling, the cartilage likely has worn away. So the bones are rubbing against each other.
Imaging techniques, most often X-rays, can confirm a diagnosis of thumb arthritis.
More Information
Treatment
In the early stages of thumb arthritis, treatment most often involves a mix of therapies that don't include surgery. But some people need surgery.
Medication
To ease pain, your healthcare professional might suggest:
- Pain relievers you put on the skin over the joint, called topical NSAIDs. These include diclofenac (Voltaren Arthritis Pain).
- Pain relievers you can get without a prescription. These include acetaminophen (Tylenol, others), ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve).
- Prescription pain relievers. These might include celecoxib (Celebrex, Elyxyb) or tramadol (Conzip).
Splint
A splint can support your joint and keep your thumb and wrist from moving too much. You might wear a splint just at night or throughout the day and night.
Splints can help:
- Ease pain.
- Keep your joint in place while you complete tasks.
- Rest your joint.
Injections
If pain relievers and a splint don't work, your healthcare professional might suggest putting a long-acting corticosteroid into your thumb joint. Corticosteroid shots can ease pain and irritation and swelling, called inflammation.
Surgery or other procedures
If other treatments don't work or if you barely can bend and twist your thumb, you might need surgery. Types of surgery include:
- Joint fusion, also called arthrodesis. This procedure fuses the bones in the affected joint. The fused joint can bear weight without pain. But it can't move well.
- Osteotomy. This procedure moves the bones in the affected joint to form them better.
- Trapeziectomy. This procedure removes all or part of one of the bones in the thumb joint. The bone is called the trapezium. A surgeon may put a graft from a tendon into the space where the trapezium was.
- Joint replacement, also called arthroplasty. This procedure removes all or part of the affected joint and replaces it with a human-made joint.
You can have any of these surgeries without an overnight hospital stay. After surgery, you can expect to wear a cast or splint over your thumb and wrist for up to eight weeks. After your healthcare professional removes the cast, you might have physical or occupational therapy to help you regain hand strength and movement.
More Information
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
To ease pain and help your thumb move better:
- Use hand tools. Tools such as jar openers, key turners and large zipper pulls are made for people who don't have much hand strength. Use levers to replace door handles that you grasp with your thumb.
- Apply cold. Put ice on the joint for 5 to 15 minutes several times a day to help ease swelling and pain.
- Apply heat. For some people, heat may work better than cold to ease pain. Heated paraffin wax, heat wraps, heating pads and steam can provide heat.

Toothbrushes with and without foam handles.
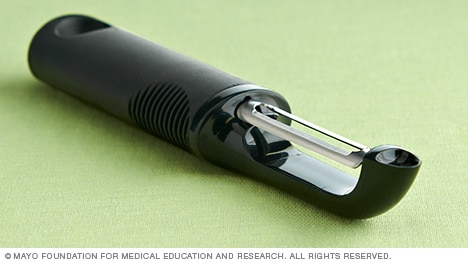
Vegetable peeler with a large, cushioned handle.

Pin tool engaging a house key.
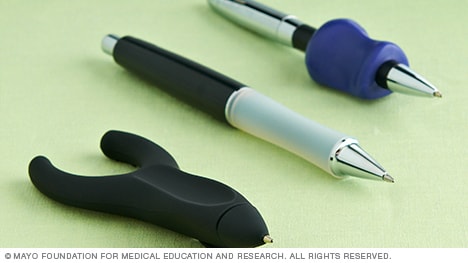
A variety of pens designed to reduce stress on finger and thumb joints.

A kitchen knife with a handle similar to a saw.

A cutting board with nail pegs.
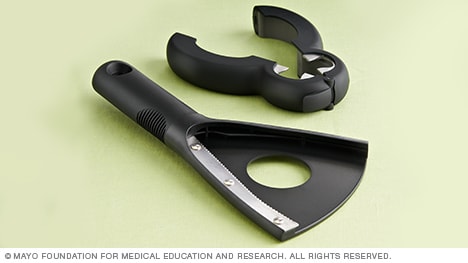
Two types of jar-opening devices.
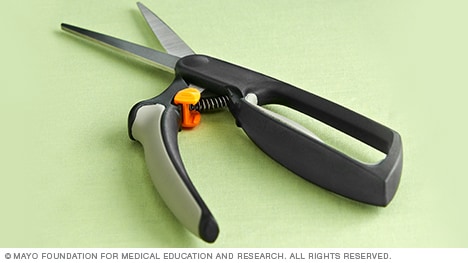
Scissors that open automatically.
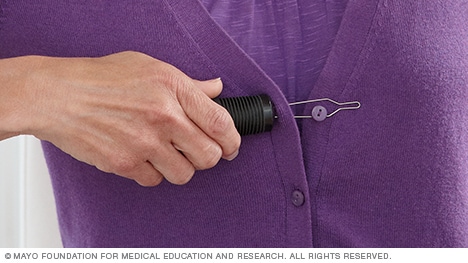
A device that helps button clothes.

A lever that attaches to doorknobs.

A woman carrying a large purse by its shoulder strap across her body.

Incorrect and correct ways to hold a book.
Preparing for your appointment
You might start by seeing your main healthcare professional. You might then see a specialist in joint conditions, called a rheumatologist.
What you can do
Have a friend or family member go with you to help you remember what you learn.
Make a list of:
- Your symptoms, including any that may not seem linked to the reason you made the appointment, and when they began.
- Your key medical information, including other conditions you have and any injuries to the painful joint.
- Key personal information, including any major changes or stressors in your life.
- All your medicines, vitamins and supplements, including dosages.
- Questions to ask your healthcare professional.
Questions to ask might include:
- What's the most likely cause of my symptoms?
- What tests do I need?
- Is my condition likely to go away?
- What treatments are there?
- Are there restrictions I should follow?
- I have other health conditions. How can I best manage them together?
Be sure to ask all the questions you have.
What to expect from your doctor
Your healthcare professional is likely to ask you questions, such as:
- How bad are your symptoms?
- Do you always have symptoms or do they come and go?
- What, if anything, seems to make your symptoms better or worse?
- Have you ever injured that hand?
Aug. 22, 2025