Overview
Thoracic aortic aneurysm
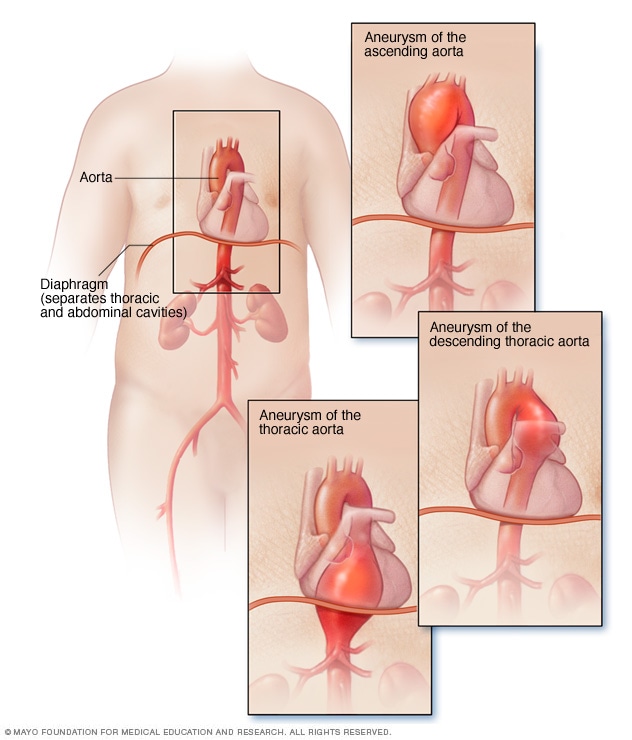
Thoracic aortic aneurysm
A thoracic aortic aneurysm is a weakened area in the upper part of the body's main artery, called the aorta. Aneurysms can develop anywhere in the aorta, including near the heart.
A thoracic aortic aneurysm is a weakened area in the body's main artery in the chest. The body's main artery is called the aorta. When the aortic wall is weak, the artery may get wider. When the artery gets very wide, it's called an aneurysm. An aneurysm can happen anywhere in the thoracic aorta, including near the heart.
A thoracic aortic aneurysm also is called a thoracic aneurysm. If the aneurysm is between the upper and lower parts of the aorta, it's called a thoracoabdominal aneurysm.
Thoracic aortic aneurysms are less common than aneurysms in the lower part of the aorta, called abdominal aortic aneurysms.
Treatment of a thoracic aortic aneurysm depends on the cause and size of the aneurysm and how fast it's growing. Treatment may range from regular health checkups to emergency surgery. A thoracic aortic aneurysm that ruptures or causes a tear called a dissection is a medical emergency that can lead to death.
Symptoms
Thoracic aortic aneurysms often grow slowly. There are usually no symptoms. That makes them hard to find. Many start small and stay small. Others get bigger over time. How quickly a thoracic aortic aneurysm may grow is hard to predict.
As a thoracic aortic aneurysm grows, symptoms may include:
- Back pain.
- Cough.
- Weak, scratchy voice.
- Shortness of breath.
- Tenderness or pain in the chest.
Symptoms that a thoracic aortic aneurysm has ruptured or caused a tear called an aortic dissection include:
- Sharp, sudden pain in the upper back that spreads down the body.
- Pain in the chest, jaw, neck or arms.
- Trouble breathing.
- Low blood pressure.
- Loss of consciousness.
- Shortness of breath.
- Trouble swallowing.
Some aneurysms may never rupture or lead to dissection.
When to see a doctor
Most people with thoracic aortic aneurysms don't have symptoms until an aortic dissection or rupture occurs. An aortic dissection or aneurysm rupture is a medical emergency. Call 911 or your local emergency number for immediate help.
Causes
Aortic dissection and aortic aneurysm
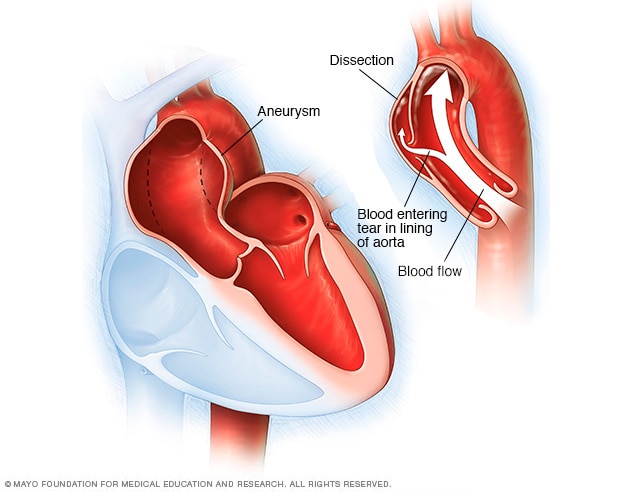
Aortic dissection and aortic aneurysm
An aortic aneurysm occurs when a weak spot in the wall of the aorta begins to bulge, as shown in the image on the left. An aneurysm can occur anywhere in the body's main artery, called the aorta. Having an aortic aneurysm increases the risk of a tear in the aortic lining, called a dissection, as shown in the image on the right.
Causes of thoracic aortic aneurysms may include:
- Atherosclerosis. A buildup of fats, cholesterol, and other substances in and on the artery walls causes the arteries to get stiff. Over time, the walls of the arteries may get weak. High blood pressure and high cholesterol increase the risk of atherosclerosis, especially in older people.
-
Genetic conditions. Aortic aneurysms in younger people are often caused by changes in genes. A genetic condition called Marfan syndrome can weaken the wall of the aorta.
If you have Marfan syndrome or a related condition, such as Loeys-Dietz syndrome or vascular Ehlers-Danlos syndrome, you have a much higher risk of a thoracic aortic aneurysm. These conditions also make you more likely to have an aortic rupture or aortic dissection.
- Blood vessel inflammation. Conditions that cause irritation and swelling of blood vessels, such as Takayasu arteritis and giant cell arteritis, are associated with thoracic aortic aneurysms.
- Bicuspid aortic valve. Usually the valve between the lower left heart chamber and the aorta has three flaps. A bicuspid valve has only two. People who are born with a bicuspid aortic valve are more likely to get a thoracic aneurysm.
- Untreated infection. Though rare, it's possible to get a thoracic aortic aneurysm if you've had an untreated infection such as syphilis or salmonella.
- Traumatic injury. Some people who are injured in falls or motor vehicle crashes get thoracic aortic aneurysms. But this is rare.
Risk factors
Anything that damages or weakens blood vessels may raise the risk of an aneurysm. Thoracic aortic aneurysm risk factors include:
- Age. Thoracic aortic aneurysms occur most often in people age 65 and older.
- Smoking and tobacco use. If you smoke or chew tobacco, it's important that you quit. Using tobacco also can worsen an aneurysm and overall health.
- High blood pressure. Increased blood pressure damages the blood vessels in the body. This raises the risk of an aneurysm.
- Coronary artery disease. This type of heart disease causes reduced blood flow to the heart. It's often caused by atherosclerosis. Atherosclerosis can damage the lining of a blood vessel, increasing the risk of an aneurysm. This is a more common risk in older people.
- Family history. You're more likely to get an aortic aneurysm and rupture if you have a parent, brother, sister or child with one. You may develop aneurysms at a younger age.
If you're at risk of an aortic aneurysm, you might get medicines to lower your blood pressure and relieve stress on weakened arteries.
Complications
Possible complications of a thoracic aortic aneurysm are:
- A tear in the wall of the aorta, also called an aortic dissection. This life-threatening condition causes bleeding into and along the aortic wall. Emergency surgery is needed to prevent death.
- Rupture of the body's main artery, called an aortic rupture. If a tear in the aorta causes bleeding outside the aorta, it's called an aortic rupture. This also is a life-threatening condition that needs treatment right away. In general, the larger the aneurysm, the greater the risk of rupture.
- Blood clots. Small blood clots can develop in the area of the aortic aneurysm. If a blood clot breaks loose from the inside wall of an aneurysm, it can block a blood vessel elsewhere in the body. This can possibly cause serious complications.
- Stroke. Signs and symptoms of stroke include weakness of or an inability to move one side of the body. It may be hard to speak.
Prevention
To prevent an aneurysm, keep the blood vessels as healthy as possible. Try these healthy lifestyle tips.
- Don't smoke or use tobacco.
- Control blood pressure and cholesterol levels.
- Keep a healthy weight and stay active.
- Eat nutritious foods.
Screening
Screening means that you have regular imaging tests, usually an echocardiogram, to look for an aneurysm.
Your healthcare professional may suggest screening for a thoracic aneurysm if:
- You have a parent, brother, sister, son or daughter with a genetic condition linked to thoracic aortic aneurysms. An example is Marfan syndrome.
- You have a family history of aortic aneurysms and wish to get pregnant.
If a screening test shows a larger than usual aorta or an aneurysm, the test is usually repeated within 6 to 12 months to look for changes.