Overview
Prolactinoma is a tumor of the pituitary gland that is not cancer. This tumor causes the pituitary gland to make too much of a hormone called prolactin.
A prolactinoma isn't life-threatening. But it can cause health concerns, including vision problems. Having a prolactinoma also can make it hard to get pregnant. That's because it lowers the body's levels of the sex hormones estrogen and testosterone. Prolactinoma is the most common type of pituitary gland tumor that can make hormones.
A prolactinoma often can be treated with medicines to shrink the tumor and bring the prolactin level in the body down. Some people need surgery to remove the tumor.

Prolactinoma
Symptoms
A prolactinoma might not cause any symptoms. But too much of the hormone prolactin in the blood due to a prolactinoma may lead to symptoms. This condition is called hyperprolactinemia. A large tumor also can put pressure on the tissue around it. That can cause symptoms too.
Too much prolactin can cause health concerns within the reproductive system — a condition called hypogonadism. Because of that, some of the symptoms of a prolactinoma are specific to females or males.
In females, prolactinoma can cause:
- Menstrual periods that are not regular or no menstrual periods.
- Milky discharge from the breasts when a person is not pregnant or breastfeeding.
- Sore breasts.
- Painful sex due to vaginal dryness.
- Acne and extra body and facial hair.
In males, prolactinoma can cause:
- Erectile dysfunction.
- Less body and facial hair.
- Smaller muscles.
- Larger breasts, called gynecomastia.
In anyone, prolactinoma can cause:
- Difficulty getting pregnant, called infertility.
- Weak and brittle bones that break easily, called osteoporosis.
- Loss of interest in sex.
Pressure from a large tumor can cause:
- Vision problems.
- Headache.
- The pituitary gland to make less of other hormones.
Females who haven't gone through menopause tend to notice symptoms earlier, when tumors are smaller. This is probably because of missed periods or periods that aren't regular. Females who have gone through menopause are more likely to notice symptoms later, when tumors are larger and more likely to cause headaches or vision problems. Males also are more likely to notice symptoms later.
When to see a doctor
If you have symptoms that may be caused by a prolactinoma, see your healthcare professional.
If you have a prolactinoma and you want to become pregnant or already are pregnant, talk to your healthcare professional. How the prolactinoma is treated may need to change.
From Mayo Clinic to your inbox
Causes
The cause of a prolactinoma often can't be found.
Prolactinoma is one type of tumor that starts in the pituitary gland. The pituitary gland is a small bean-shaped gland at the base of the brain. Although it's small, the pituitary gland has an effect on nearly every part of the body. Its hormones help control important work in the body, such as growth, metabolism, blood pressure and reproduction.
A prolactinoma causes the pituitary gland to make too much of a hormone called prolactin. This lowers the amount of the sex hormones estrogen and testosterone in the body.
The pituitary gland can make a high amount of prolactin due to reasons other than a prolactinoma, including:
- Medicines.
- Other types of pituitary tumors.
- Kidney disease.
- The thyroid gland not working correctly.
- Pregnancy and breastfeeding.
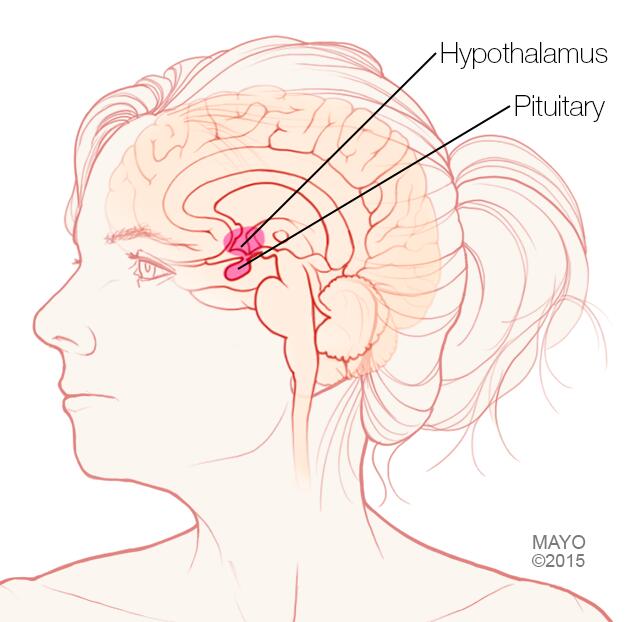
Pituitary gland and hypothalamus

Endocrine system
Risk factors
Risk factors for a prolactinoma include sex and genetics.
More prolactinomas happen in females than in males. The condition rarely happens in children.
Rarely, an inherited disorder such as multiple endocrine neoplasia type 1 ⸺ a condition that causes tumors in glands that make hormones ⸺ may raise the risk of a prolactinoma.
Complications
Health concerns linked to a prolactinoma, called complications, may include:
- Difficulty getting pregnant, called infertility. Too much prolactin lowers how much estrogen and testosterone the body makes. Too much prolactin also can keep the body from releasing an egg during a menstrual cycle. This condition is called anovulation. Too much prolactin can lower the amount of sperm that the body makes.
- Bone loss, called osteoporosis. Less estrogen and testosterone in the body causes a loss of bone strength. This leads to weak and brittle bones that can break easily.
- Health concerns during pregnancy. During pregnancy, the amount of estrogen that the body makes goes up. That can cause a prolactinoma to grow. The growth may lead to symptoms such as headaches and vision changes in pregnant people who have a large prolactinoma.
- Vision problems. If it isn't treated, a prolactinoma may grow large enough to press on the optic nerve. The optic nerve sends images from the eye to the brain so that you can see. The first sign of pressure on the optic nerve often is a loss of side vision, called peripheral vision.
- Low levels of other pituitary gland hormones. Larger prolactinomas can put pressure on the healthy part of the pituitary gland. This can lead to lower levels of other hormones that the pituitary gland controls. Those include thyroid hormone, growth hormone and cortisol.