Diagnosis
Spirometer
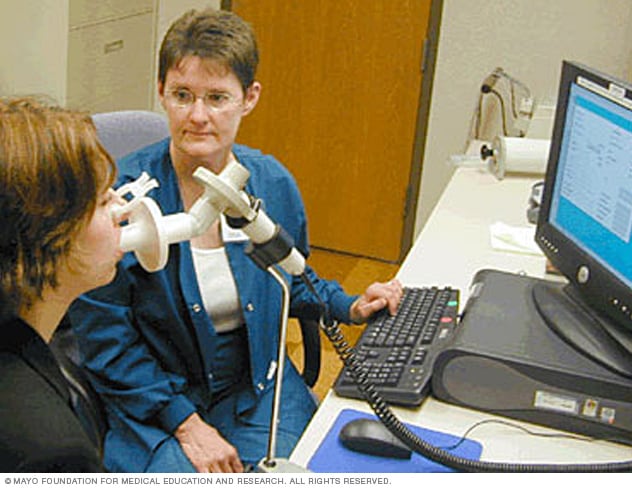
Spirometer
A spirometer is a diagnostic device that measures the amount of air you can breathe in and out and the time it takes you to breathe out completely after you take a deep breath.
Diagnosing occupational asthma is similar to diagnosing other types of asthma. However, your healthcare professional also will try to identify whether a workplace substance is causing your symptoms and what substance is causing problems.
An asthma diagnosis needs to be confirmed with a test called a lung function test. This test shows how well your lungs work. An allergy skin prick test can show if you have allergic reactions to some allergy-causing substances. Blood tests, X-rays or other tests may be necessary to rule out a cause other than occupational asthma.
Testing your lung function
Lung function tests include:
-
Spirometry. During this 10- to 15-minute test, you take deep breaths and forcefully exhale into a hose connected to a machine called a spirometer. A spirometer measures how much air your lungs can hold and how quickly you can breathe out. This is the preferred test for diagnosing asthma.
You will repeat the test after inhaling asthma medicine that helps open airways. Improved lung function after using the medicine supports a diagnosis of asthma.
-
Peak flow measurement. You may be asked to carry a small hand-held device called a peak flow meter. This device measures how quickly you can force air out of your lungs. The slower you exhale, the worse your condition.
You'll likely be asked to use your peak flow meter at certain times during working and nonworking hours. If your breathing improves significantly when you're away from work, you may have occupational asthma.
Tests for causes of occupational asthma
You may need tests to see whether you have a reaction to specific substances. These include:
- Allergy skin tests. During a skin test, small amounts of common allergy-causing substances are scratched into your skin. Then the area is observed for about 15 minutes. Swelling or a change in skin color indicates an allergy to the substance. These tests can show an allergy to animals, mold, dust mites, plants and latex. They can't be used to measure a reaction to chemicals.
- Challenge test. You inhale a mist containing a small amount of a suspected chemical to see if it triggers a reaction. Your lung function will be tested before and after the test is given to see if the chemical affects your ability to breathe.
- Chest X-ray. Occupational asthma is one kind of occupational lung disease. You might need a chest X-ray to diagnose other kinds of job-related breathing problems.
Treatment
The goal of treatment is to prevent symptoms and stop an asthma attack in progress.
Avoiding the workplace substance that causes your symptoms is important. Once you become sensitive to a substance, tiny amounts may trigger asthma symptoms, even if you wear a mask or respirator.
You may need medicines for successful treatment. The same medicines are used to treat both occupational and nonoccupational asthma.
The right medicine for you depends on many things. These include your age, symptoms, asthma triggers and what seems to work best to keep your asthma under control.
Long-term control medicines
- Inhaled corticosteroids. Inhaled corticosteroids reduce inflammation and have a relatively low risk of side effects.
- Leukotriene modifiers. These medicines are alternatives to corticosteroids. Sometimes, they're taken with corticosteroids.
- Long-acting beta agonists (LABAs). LABAs open the airways and reduce inflammation. For asthma, LABAs generally should only be taken in combination with an inhaled corticosteroid.
- Combination inhalers. These medicines contain a LABA and a corticosteroid.
Quick-relief, short-term medications
- Short-acting beta agonists. These medicines ease symptoms during an asthma attack.
- Oral and intravenous corticosteroids. These relieve airway inflammation for severe asthma. These are taken by mouth or given as a shot. Over the long term, they cause serious side effects.
If you need to use a quick-relief inhaler more often than recommended, you may need to adjust your long-term control medicine.
Also, if allergies trigger or worsen your asthma, you may benefit from allergy treatments. These treatments include medicines taken by mouth or with a nasal spray. Antihistamines help block some immune system activity that causes allergy symptoms. Decongestants help relieve a stuffy nose.
Alternative medicine
Many people claim alternative remedies reduce asthma symptoms. But in most cases, more research is needed to see if they work and if they have possible side effects. Alternative remedies that need further study include:
- Breathing techniques. These include structured breathing programs such as the Buteyko method, the Papworth method, lung-muscle training and yoga breathing exercises. While these techniques may help improve quality of life, they have not proved to improve asthma symptoms.
- Acupuncture. This technique has roots in traditional Chinese medicine. It involves placing very thin needles at strategic points on the body. Acupuncture is safe and generally painless, but there is not enough evidence to show it treats asthma.
Preparing for your appointment
You're likely to start by seeing your primary healthcare professional. Or you may start by seeing a doctor who specializes in asthma, such as an allergist-immunologist or a pulmonologist.
Here's some information to help you prepare for your appointment.
What you can do
- Be aware of any pre-appointment restrictions. When you make the appointment, ask if there's anything you need to do in advance. You may need to stop taking antihistamines if you're likely to have an allergy skin test.
- Write down any symptoms you're experiencing, including any that do not seem related to problems with breathing.
- Note the timing of your asthma symptoms — for example, note if your symptoms are worse at work and get better when you're away from work.
- Make a list of all possible workplace lung irritants and anything else that seems to trigger your symptoms. You may want to take a look at the material safety data sheet (MSDS) for your work area, if there is one. This sheet lists toxic substances and irritants used on your job site. Keep in mind, not all occupational asthma triggers are listed in the MSDS.
- Write down key personal information, including major stresses or recent life changes and changes in your job or workplace.
- Bring a list of all medicines, vitamins or supplements you take.
- Bring a family member or friend along, if possible. Someone who accompanies you may remember information you missed or forgot.
- Write down questions to ask your care healthcare professional.
For occupational asthma, some basic questions to ask include:
- Is a workplace irritant a likely cause of my breathing problems or asthma attacks?
- What are other possible causes for my symptoms or condition?
- What tests do I need? Do these tests require any special preparation?
- Is my condition likely temporary or chronic?
- How do I treat occupational asthma? Do I have to quit my job?
- What are the alternatives to the treatment you're suggesting?
- I have other health conditions. How can I best manage these conditions together?
- Are there restrictions that I need to follow?
- Should I see a specialist?
- Is there a generic alternative to the medicine you're prescribing?
- Are there brochures or other printed material I can take with me? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Your healthcare professional is likely to ask you several questions, such as:
- When did you first notice your symptoms?
- If you already use asthma medicine, how often do you use a quick-relief inhaler?
- Do you have breathing problems when you're away from work or only when you're on the job?
- Have your symptoms been continuous, or do they come and go?
- Have you been diagnosed with allergies or asthma?
- Are you exposed to fumes, gases, smoke, irritants, chemicals, or plant or animal substances at work? If so, how often and for how long?
- Do you work in unusual environmental conditions, such as extreme heat, cold or dryness?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
- Do other members of your family have allergies or asthma?
Feb. 27, 2024