Overview
Measles, also called rubeola, was once a common childhood illness. It's caused by a virus that spreads easily through the air and settles on surfaces. A vaccine can prevent measles infection.
Most people recover from measles in about 10 days. It usually doesn't cause long-term medical issues. But measles can be serious and even deadly. This is especially true for children younger than age 5 and people with severely weakened immune systems.
Measles is treated by managing symptoms and preventing complications.
Get a measles vaccine when recommended to keep the virus from spreading. Because of vaccination, measles hasn't been common in the United States for more than two decades. Often, measles cases in the U.S. come from outside the country. Outbreaks are more common among people who are not vaccinated.

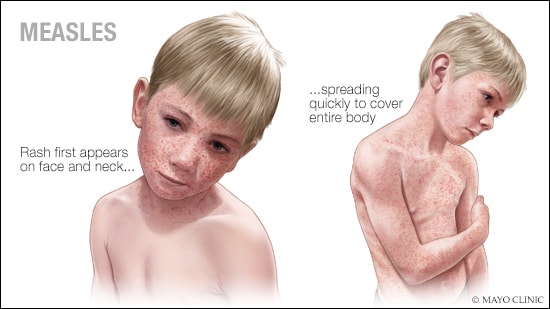
Measles
Measles illness causes a blotchy rash. It may be shades of red, purple or brown depending on your skin color. The rash most often shows up first on the face and behind the ears. The rash then spreads to the chest and back and finally to the feet.
Symptoms
Measles symptoms show up around 7 to 14 days after contact with the virus.
The first symptoms usually are:
- Fever, which may be as high as 105 degrees Fahrenheit (40.6 degrees Celsius).
- Dry cough.
- Runny nose.
- Red, watering eyes, called conjunctivitis.
About 2 to 3 days after the first symptoms, you also may see tiny white spots inside the mouth, called Koplik spots.
About 3 to 5 days after symptoms first start, or about 14 days after you come into contact with the virus, it's common to see a rash. The rash is made up of large, flat spots and small raised bumps. The rash starts on the face or neck and spreads down the body from the chest to the arms and legs.
A person with measles can spread the virus four days before the rash appears and four days after. Measles can spread very easily. About 90% of people who haven't had measles or haven't been vaccinated will become infected when around someone with measles.
When to see a doctor
Call your healthcare professional if you think you or your child may have been around measles. Also call if you or your child has a rash that looks like measles. Check your family's vaccination records with your healthcare professional. This is most important before your children start child care, school or college, and before traveling outside of the U.S.
From Mayo Clinic to your inbox
Causes
Measles is caused by a virus that spreads only among humans. When someone with measles coughs, sneezes or talks, droplets spray into the air. People who breathe in the droplets can catch the virus. Droplets also may land on surfaces. You can catch measles if you touch an infected surface and then touch your mouth, nose or eyes. These droplets can infect other people for up to two hours.
Risk factors
Your risk of measles goes up if you aren't vaccinated. Your risk also goes up if you've had only one dose of the vaccine. People who travel to places where measles regularly spreads or where there is a measles outbreak are more likely to get the illness. This is especially true if you haven't had two doses of the measles vaccine.
Students living in dormitories may be at higher risk. People with weakened immune systems are at higher risk of catching measles. And infants who aren't old enough to get the vaccine are at higher risk than average if exposed to measles virus.
Complications
Complications of measles may include:
- Dehydration. Diarrhea and vomiting can cause the body to lose too much water, called dehydration.
- Ear infection. One of the most common complications of measles is an ear infection caused by bacteria.
- Bronchitis, laryngitis or croup. Measles may lead to irritation and swelling, called inflammation, of the airways. This inflammation of the airways is called croup. Measles also can lead to inflammation of the inner walls that line the main air passages of the lungs. This condition is called bronchitis. Measles also causes inflammation of the voice box, which is called laryngitis.
- Pneumonia. Measles can cause an infection in the lungs, called pneumonia.
- Encephalitis. About 1 in 1,000 people with measles can get irritation and swelling of the brain, called encephalitis. The condition can be a danger to people with weakened immune systems. Encephalitis may happen right after measles or months later. Encephalitis can cause lasting brain damage.
- Pregnancy complications. Getting measles while pregnant can put the pregnant person's life in danger. It also can lead to pregnancy loss, fetal death or problems with how the baby forms.
Pneumonia and encephalitis complications are the most common causes of death from measles. Some groups of people have a higher than average risk of death due to measles, including:
- Children younger than age 5.
- Adults older than age 20.
- People who are pregnant.
- People with weakened immune systems.
- People who are severely malnourished, including those with vitamin A deficiency.
It's rare, but measles can cause brain or nervous system illness years after infection.
- People who have a weakened immune system can get a disease called measles inclusion body encephalitis, also called MIBE.
- Measles also can lead to a disease called subacute sclerosing panencephalitis, also called SSPE. The disease most often shows up 7 to 11 years after getting a measles infection. Children who caught measles before age 2 seem to be at higher risk than average.
Also, a measles infection in children may wipe out the immune system's memory of germs. This means after infection with the measles virus, children may be more likely to get sick from germs they recovered from before. They also may need to get standard childhood vaccines again.
Prevention
The U.S. Centers for Disease Control and Prevention, also called CDC, recommends that children and adults get a measles vaccine. On average, the vaccine gives lifelong protection from measles for about 97% of people who get two doses of the vaccine.
For the small group of people who get measles after being fully vaccinated, illness symptoms tend to be mild. These people tend not to spread the disease to others.
In the United States, the measles vaccine is made from a weakened measles virus. The vaccine is offered as a combined shot to protect against measles and other viruses.
- The MMR vaccine protects against measles, mumps and rubella.
- The MMRV vaccine protects against measles, mumps, rubella and chickenpox, also called varicella.
Measles vaccines offered outside the United States may protect against measles only or a combination of measles, mumps, rubella and varicella.
Most people can get the measles vaccines.
Do not get the vaccine if you've had a serious allergic reaction after the first dose of MMR or MMRV or the antibiotic medicine neomycin. Don't get the measles vaccine if you're pregnant. And don't get the vaccine if you have a severely weakened immune system due to treatment or illness.
Check with a healthcare professional before getting a measles vaccine if you:
- Have had seizures in the past or have a family history of seizures.
- Plan to get pregnant in the next four weeks.
- Recently needed a blood transfusion or other blood products.
- Recently took corticosteroids.
- Are being treated for tuberculosis.
If you have questions about whether you should get a measles vaccine, talk to your healthcare professional.
Measles vaccine in children
The CDC recommends that children get a measles vaccine between 12 and 15 months of age, and again between 4 and 6 years of age, before they start school. The timing of a measles vaccine could shift in some situations. The shortest time between the first and second dose of measles vaccine is 28 days.
- Children 6 to 11 months old may get the vaccine early if they were exposed to measles or due to travel. Talk to your child's healthcare professional before you travel anywhere that has an ongoing measles outbreak or anyplace where measles regularly spreads. Children who are vaccinated early still need two doses of the measles vaccine at the recommended ages.
- Children or teens who didn't get two doses of the vaccine and need to catch up might need to get those doses at least 28 days apart.
Side effects from the vaccine include a sore area where the shot was given. That area also may change color to a shade of red, purple or brown depending on your skin color.
Other side effects are fever, rash, swelling of glands in the face or neck, and joint stiffness or pain. If your child gets a rash after the MMRV shot, it could be linked to the varicella part of the vaccine. If that happens, keep your child away from people with weakened immune systems and infants. Rarely, some children have had seizures after vaccination. Some children may have a temporary drop in platelets. Platelets help with blood clotting.
Talk to your child's healthcare professional about other side effects and risks for your child.
No proven link between the MMR vaccine and autism
Vaccines do not cause autism. The study that suggested this connection in 1998 was based on scientific errors. That study was removed from the scientific record in 2010.
Measles vaccine in adults
Most people born or living in the U.S. before 1957 are immune to measles because they've had the infection. If you've had measles, you can't get measles again.
Proof that you've had measles includes:
- A vaccine log or other document showing you had two doses of a vaccine made from the weakened measles virus.
- Lab test that show you had measles or have antibodies to the virus.
- A medical record showing you had measles.
If you got the measles vaccine offered between 1963 and 1968, you'll need to get vaccinated again. The vaccine from that time doesn't give you long-term protection from measles. And if you only got one shot of the measles vaccine, you may need to get another dose. This is true for people at high risk during an outbreak, college students, healthcare professionals and people who travel widely.
If you're not sure if you need the measles vaccine, talk with your healthcare professional. The measles vaccine available for adults in the United States is the MMR vaccine.
Preventing measles during an outbreak or known infection
When measles starts to spread in a community, health departments in the area may suggest other precautions. Second shots for children may be moved up, and earlier vaccination of infants may be discussed with families. If you have had two shots of the MMR vaccine, it isn't recommended that you get a third dose during an outbreak.
If you think you or your child has measles, call your healthcare professional right away. Because measles spreads easily from about four days before to four days after the rash appears, people with measles should stay home and stay away from other people during this time.
Preventing new infections
Getting a measles vaccine is important to prevent measles from spreading during an outbreak or in the future. Soon after vaccination rates drop, measles start to come back. Measles spreads so easily that 95% of a population may need to be immune to stop an outbreak. To prevent measles from becoming more widespread, more than 90% of people in the United States may need to be immune to measles.
History of infectious disease outbreaks and vaccines timeline.
Learn about the history of major disease outbreaks, epidemics and pandemics, as well as the impact vaccines and research had on many infectious diseases.
Find out more at History of infectious disease outbreaks and vaccines timeline.