Overview
Lyme disease is an illness caused by borrelia bacteria. Humans usually get Lyme disease from the bite of a tick carrying the bacteria.
Ticks that can carry borrelia bacteria live throughout most of the United States. But Lyme disease is most common in the upper Midwest and the northeastern and mid-Atlantic states. It's also common in Europe and in south central and southeastern Canada.
You're at risk of Lyme disease if you spend time where the ticks live, such as grassy, brushy or wooded areas. Taking safety measures in these areas can lower the risk of Lyme disease.
Products & Services
Symptoms
A tick bite may look like as a tiny, itchy bump on your skin, much like a mosquito bite. This doesn't mean you have a tick-borne disease. Many people will not notice they've had a tick bite.
The symptoms of Lyme disease vary. They usually show up in stages. But the stages can overlap. And some people don't have symptoms of the typical early stage.
Stage 1
Lyme disease rash
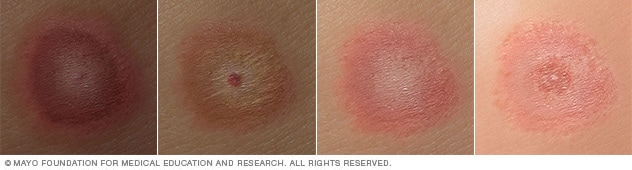
Lyme disease rash
Illustration of Lyme disease rash on different skin colors. People with Lyme disease might get a bull's-eye rash. The rash gradually spreads over a period of days.
Early symptoms of Lyme disease usually happen within 3 to 30 days after a tick bite. This stage of disease has a limited set of symptoms. This is called early localized disease.
A rash is a common sign of Lyme disease. But it doesn't always happen. The rash is usually a single circle that slowly spreads from the site of the tick bite. It may become clear in the center and look like a target or bull's-eye. The rash often feels warm to the touch, But it's usually not painful or itchy.
Other stage 1 symptoms include:
- Fever.
- Headache.
- Extreme tiredness.
- Joint stiffness.
- Muscle aches and pains.
- Swollen lymph nodes.
Stage 2
Without treatment, Lyme disease can get worse. The symptoms often show up within 3 to 10 weeks after a tick bite. Stage 2 is often more serious and widespread. It is called early disseminated disease.
Stage 2 may include the stage 1 symptoms and the following:
- Many rashes on other parts of the body.
- Neck pain or stiffness.
- Muscle weakness on one or both sides of the face.
- Immune-system activity in heart tissue that causes irregular heartbeats.
- Pain that starts from the back and hips and spreads to the legs.
- Pain, numbness or weakness in the hands or feet.
- Painful swelling in tissues of the eye or eyelid.
- Immune-system activity in eye nerves that causes pain or vision loss.
Stage 3
In the third stage, you may have symptoms from the earlier stages and other symptoms. This stage is called late disseminated disease.
In the United States, the most common condition of this stage is arthritis in large joints, particularly the knees. Pain, swelling or stiffness may last for a long time. Or the symptoms may come and go. Stage 3 symptoms usually begin 2 to 12 months after a tick bite.
The type of Lyme disease common in Europe can cause a skin condition called acrodermatitis chronic atrophicans. The skin on the backs of the hands and tops of the feet get discolored and swell. It also may show up over the elbows and knees. More-serious cases may cause damage to tissues or joints.
This skin condition may show up many months to many years after a tick bite.
When to see a doctor
Most people who get Lyme disease don't remember having a tick bite. And many symptoms of Lyme disease relate to other conditions. See your healthcare professional if you have Lyme disease symptoms. An early diagnosis and proper treatment can improve outcomes.
If you know you had a tick bite or might have been around ticks, watch for symptoms. If they show up, see your healthcare professional as soon as possible.
Causes
Deer tick

Deer tick
The deer tick, also called the black-legged tick and Ixodes scapularis, is mainly found in eastern half and Midwest region of the United States.
Lyme disease is caused by borrelia bacteria. In North America, the black-legged tick, also called the deer tick, mainly carry the bacteria.
In Europe, a different species of borrelia causes Lyme disease. Ticks carry the bacteria. These ticks are known by a few names, including castor bean tick, sheep tick or deer tick.
Tick bites
Ticks feed on blood by attaching to a host's skin. The tick feeds until it's swollen to many times its typical size. Deer ticks can feed on a host's blood for several days.
Ticks pick up bacteria from a host, such as a deer or rodent. They don't get sick. But they can pass the bacteria to another host. When an infected tick feeds on a person, the bacteria can move to the person's bloodstream. The bacteria are less likely to spread Lyme disease if you remove the tick within 24 hours.
Both young and adult ticks can carry the disease. Young ticks are tiny and hard to spot. You may not notice if a young tick bites you.
Risk factors
Your risk for getting Lyme disease depends on if you spend time where they are likely to live. This includes the:
- Region. Deer ticks that carry Lyme disease are widespread. They are mostly found in the upper Midwest, the northeastern and mid-Atlantic states, and in south central and southeastern Canada. The castor bean tick is found throughout Europe.
- Habitat. Ticks live in wooded, shrubby or grassy areas.
- Time of year. The risk of infection is greater in the spring, summer and fall. But ticks can be active any time the temperature is above freezing.
Complications
Some people with Lyme disease report symptoms that continue after treatment. These longer-lasting symptoms may include:
- Arthritis that begins with Lyme disease and doesn't improve.
- Body aches and pains.
- Constant or frequent tiredness.
- Memory complaints.
Prevention
The best way to prevent Lyme disease is to avoid tick bites when you are outdoors. Most ticks attach themselves to your lower legs and feet as you walk or work in grassy, wooded areas or overgrown fields. After a tick attaches to your body, it often crawls upward to find a spot to burrow into your skin.
If you're in or plan to be in an area where ticks are likely to live, follow these tips to protect yourself.
Use tick repellents
- Spray your outdoor clothing, shoes, tent and other camping gear with a repellent that has 0.5% permethrin. Some gear and clothing may be pre-treated with permethrin.
- Use an insect repellent registered with the Environmental Protection Agency on any exposed skin, except your face. These include repellents that contain DEET, picaridin, IR3535, oil of lemon eucalyptus (OLE), para-menthane-diol (PMD) or 2-undecanone.
- Do not use products with OLE or PMD on children under age 3.
Dress for protection
- Wear light-colored clothing that makes it easier for you or others to see ticks on your clothing.
- Avoid open-toed shoes or sandals.
- Wear long-sleeved shirts tucked into your pants.
- Wear long pants tucked into your socks.
Check for ticks
- Shower as soon as possible to wash off any loose ticks. Check for ticks that may have burrowed.
- Use a mirror to check your body well. Pay attention to your underarms, hair and hairline. Also check your ears, waist, and the area between your legs, behind your knees, and inside your bellybutton.
- Check your gear. Before you wash your outdoor clothes, put them in the dryer on hot for at least 10 minutes to kill ticks.
Other tips
- Do a daily inspection for ticks on any pet that spends time outdoors.
- Stay on clear paths as much as possible in wooded and grassy areas.