Diagnosis
To diagnose atherosclerosis, your healthcare professional examines you and listens to your heart. You usually are asked questions about your symptoms and your family health history. You may be sent to a doctor trained in heart diseases, called a cardiologist.
Your healthcare professional may hear a whooshing sound when listening to your heart with a stethoscope.
Tests
Coronary calcium scan
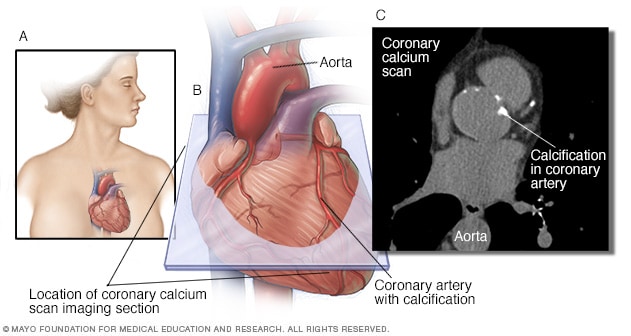
Coronary calcium scan
A coronary calcium scan uses computerized tomography (CT) imaging to take pictures of the heart's arteries. It can detect calcium deposits in the coronary arteries. Calcium deposits can narrow the arteries and increase the risk of a heart attack. The image on the left shows where the heart is typically located in the body (A). The middle image shows the area of the coronary calcium scan image (B). The image on the right shows a coronary calcium scan (C).
Tests may be done to check the health of your heart and arteries. Tests can help diagnose atherosclerosis and find the cause.
- Blood tests. Blood tests can check blood sugar and cholesterol levels. High levels of blood sugar and cholesterol raise the risk of atherosclerosis. A C-reactive protein (CRP) test also may be done to check for a protein linked to inflammation of the arteries.
- Electrocardiogram (ECG or EKG). This quick and painless test measures the electrical activity of the heart. During an ECG, sticky patches with sensors on them attach to the chest and sometimes to the arms or legs. Wires connect the sensors to a machine, which displays or prints the results. An ECG can show if there's reduced blood flow to the heart.
- Exercise stress tests. These tests often involve walking on a treadmill or riding a stationary bike while the heart's activity is watched. Because exercise makes the heart pump harder and faster than it does during most daily activities, an exercise stress test can show heart conditions that might otherwise be missed. If you can't exercise, you may get medicine that affects the heart like exercise does.
- Echocardiogram. This test uses sound waves to show blood flow through the heart. It also shows the size and shape of the structures of the heart. Sometimes an echocardiogram is done during an exercise stress test.
- Doppler ultrasound. A healthcare professional may use a special ultrasound device to check blood flow at different points in your body. The test results show the speed of blood flow in the arteries. This can reveal any narrowed areas.
- Ankle-brachial index (ABI). This test compares the blood pressure in the ankle with that in the arm. It's done to check for atherosclerosis in the arteries in the legs and feet. A difference between the ankle and arm measurements may be due to peripheral artery disease.
- Cardiac catheterization and angiogram. This test can show if the coronary arteries are narrowed or blocked. A doctor places a long, thin flexible tube in a blood vessel, usually in the groin or wrist, and guides it to the heart. Dye flows through the catheter to arteries in the heart. The dye helps the arteries show up more clearly on images taken during the test.
- Coronary calcium scan, also called a heart scan. This test uses computerized tomography (CT) imaging to look for calcium deposits in the artery walls. A coronary calcium scan may show coronary artery disease before you have symptoms. Results of the test are given as a score. The higher the calcium score, the higher the risk of heart attacks.
- Other imaging tests. Magnetic resonance angiography (MRA) or positron emission tomography (PET) also may be used to study the arteries. These tests can show hardening and narrowing of large arteries, as well as aneurysms.
More Information
Treatment
Treatment of atherosclerosis may include:
- Lifestyle changes, such as eating a healthy diet and getting more exercise.
- Medicines.
- Heart procedure.
- Heart surgery.
For some people, lifestyle changes may be the only treatment needed for atherosclerosis.
Medications
Many different medicines can slow — or even reverse — the effects of atherosclerosis. Medicines to treat atherosclerosis may include:
-
Statins and other cholesterol medicines. These medicines can help lower low-density lipoprotein (LDL) cholesterol, also called the "bad" cholesterol. The medicines also can reduce plaque buildup. Some cholesterol medicines even can reverse the buildup of fatty deposits in the arteries.
Statins are a common type of cholesterol medicine. Other types include niacin, fibrates and bile acid sequestrants. You may need more than one type of cholesterol medicine.
- Aspirin. Aspirin helps thin the blood and prevent blood clots. Daily low-dose aspirin therapy may be recommended for the primary prevention of heart attack or stroke in certain people. Primary prevention means you've never had a heart attack or stroke. You've never had coronary bypass surgery or coronary angioplasty with stent placement. You've never had blocked arteries in your neck, legs or other parts of the body. But you take a daily aspirin to prevent such heart events. The benefit of aspirin for this use has been debated. Don't start taking a daily aspirin without talking to a healthcare professional.
- Blood pressure medicine. Medicines to lower blood pressure don't help reverse atherosclerosis. Instead they prevent or treat complications related to the disease. For example, some blood pressure medicines can help reduce the risk of a heart attack.
- Other medicines. Medicines may be used to control other conditions that raise the risk of atherosclerosis. Diabetes is one example. Medicines also may be given to treat specific symptoms of atherosclerosis, such as leg pain during exercise.
- Fibrinolytic therapy. If a clot in an artery is blocking blood flow, your healthcare professional may use a clot-dissolving medicine to break it apart. This therapy is generally used in emergency situations.
Surgery or other procedures
If atherosclerosis causes a severe blockage in an artery, you may need a procedure or surgery to treat it.
Surgery or procedures for atherosclerosis may include:
- Angioplasty and stent placement, also called percutaneous coronary intervention. This treatment helps open a clogged or blocked artery. A doctor guides a thin, flexible tube called a catheter to the narrowed part of the artery. A tiny balloon is inflated to help widen the blocked artery and improve blood flow. A small wire mesh tube called a stent may be used to keep the artery open. Some stents slowly release medicine to help keep the arteries open.
- Endarterectomy. This is surgery to remove fatty buildup from the walls of a narrowed artery. When the treatment is done on arteries in the neck, it's called a carotid endarterectomy.
- Coronary artery bypass graft (CABG) surgery. A surgeon takes a healthy blood vessel from another part of the body to create a new path for blood in the heart. The blood then goes around the blocked or narrowed coronary artery. CABG is an open-heart surgery. It's usually done only in people who have many narrowed heart arteries.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Lifestyle changes can help keep the arteries healthy. They also can prevent or slow atherosclerosis. The American Heart Association recommends these eight heart-healthy tips:
- Don't smoke, vape or use tobacco. Also stay away from cigarette smoke. Smoking damages the arteries. Smoking is a major risk factor for coronary artery disease. Nicotine tightens blood vessels and forces the heart to work harder. Not smoking is one of the best ways to lower the risk of atherosclerosis complications, such as a heart attack.
- Get regular exercise. Staying active keeps the body healthy. Exercise at least 30 minutes a day on most days of the week. Talk with your healthcare team about the amount and type of exercise that's best for you.
- Keep a healthy weight. Being overweight increases the risk of coronary artery disease, which is caused by atherosclerosis. Losing even a small amount of weight can help reduce the risk. Ask your healthcare professional what weight is best for you.
- Eat healthy foods. Choose fruits, vegetables and whole grains. Limit salt and saturated fats. Read nutrition labels to check the amount of salt and fat.
- Manage stress. Find ways to help reduce stress. Some ideas are to get more exercise, practice mindfulness and connect with others in support groups. Or try yoga or deep breathing. These relaxation practices can temporarily lower blood pressure, reducing the risk of developing atherosclerosis.
- Control blood pressure, blood sugar and cholesterol. Make lifestyle changes and take medicines as directed. Get regular health checkups.
- Limit alcohol. If you choose to drink alcohol, do so in moderation. For healthy adults, that means up to one drink a day for women and up to two drinks a day for men.
- Get good sleep. Poor sleep may increase the risk of heart disease and other health conditions. Adults should aim for 7 to 9 hours daily.
Alternative medicine
Some foods and herbal supplements may help lower cholesterol and blood pressure. Those two conditions are major risk factors for developing atherosclerosis. Possible alternative medicine products for atherosclerosis include:
- Alpha-linolenic acid.
- Barley.
- Beta-sitosterol, found in supplements and added to some margarines.
- Blond psyllium, found in seed husk and some fiber supplements.
- Cocoa.
- Fish oil.
- Garlic.
- Green tea.
- Oat bran, found in oatmeal and whole oats.
- Sitostanol, found in supplements and added to some margarines.
Talk to your healthcare professional before adding supplements to your atherosclerosis treatment. Some supplements change the way medicines for atherosclerosis work. This could cause harmful side effects.
Preparing for your appointment
If you think you may have atherosclerosis or if you have a family history of heart disease, make an appointment for a health checkup. Ask if you need a cholesterol test.
Here's some information to help you get ready for your appointment.
What you can do
- Be aware of any pre-appointment restrictions. When you make the appointment, ask whether there's anything you need to do before your visit. For example, you may be told not to eat or drink for a few hours before a cholesterol test.
- Write down any symptoms. Include those that may not seem related to atherosclerosis. Always tell your healthcare team if you have symptoms such as chest pains or shortness of breath. Such information helps guide treatment.
- Write down important personal information. Include if you have a family history of high cholesterol, heart disease, stroke, high blood pressure or diabetes. Also note if you have had any major stresses or recent life changes.
- Make a list of all medicines, vitamins or supplements that you take. Include dosages.
- Take someone along, if possible. Someone who goes with you may remember something that you missed or forgot.
- Be prepared to talk about your food and exercise habits. If you don't already eat healthy or exercise, your healthcare team can give you tips on how to get started.
- Write down questions to ask your healthcare professional.
For atherosclerosis, some basic questions to ask your healthcare professional are:
- What tests will I need?
- What's the best treatment?
- What foods should I eat or not eat?
- What's an appropriate level of exercise?
- How often do I need a cholesterol test?
- What are the options to the primary treatment you're suggesting?
- Is there a generic option to the medicine you're prescribing?
- I have other health conditions. How can I best manage them together?
- Should I see a specialist?
- Are there brochures or other printed material that I can take with me? What websites do you recommend?
Don't hesitate to ask any other questions.
What to expect from your doctor
Your healthcare team is likely to ask many questions, including:
- Do you have a family history of high cholesterol, high blood pressure or heart disease?
- What are your diet and exercise habits like?
- Do you or did you smoke or use tobacco in any form?
- Do you have chest pain or discomfort or pain in your legs with walking or at rest?
- Have you had a stroke or unexplained numbness, tingling or weakness of one side of your body, or difficulty speaking?
What you can do in the meantime
It's never too early to make healthy lifestyle changes. Eat healthy, be active, get more exercise and don't smoke or vape. These are simple ways to protect yourself against atherosclerosis and its complications, including heart attack and stroke.
Sept. 20, 2024