Overview
The anal canal
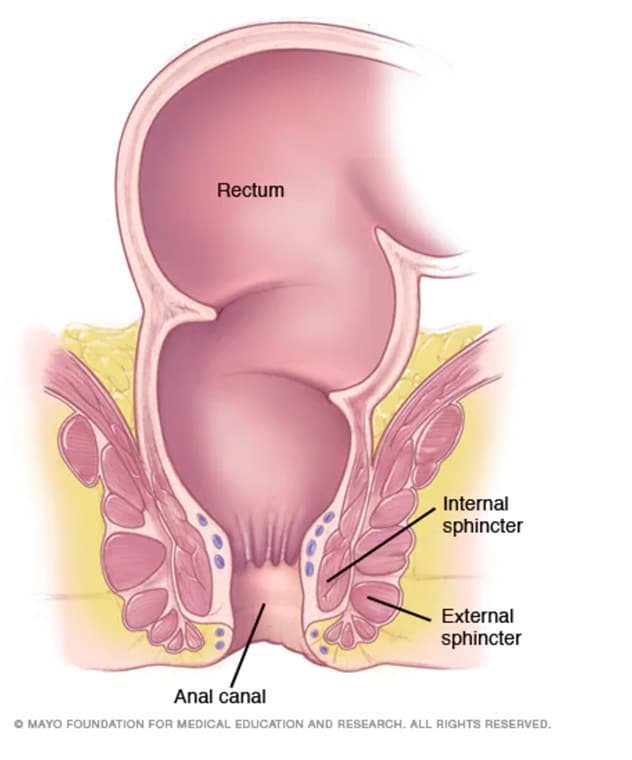
The anal canal
The anal canal is a tube at the end of the rectum that measures 1 1/2 inches in length (about 4 centimeters). Muscles called sphincters surround the anal canal. The sphincters relax to allow waste to leave the body.
Anal cancer is a growth of cells that starts in the anal canal. The anal canal is a short tube at the end of rectum. Stool passes through the anal canal as it leaves the body.
Anal cancer can cause symptoms such as rectal bleeding, blood in the stool and anal pain. As it grows, it might cause a growth or lump. Sometimes these symptoms might be mistaken for hemorrhoids.
In the past, most people with anal cancer had surgery to remove the cancer. Often this operation involved making a new way for waste to leave the body. Today, most anal cancer treatment involves chemotherapy and radiation therapy. With this approach, surgery might not be needed.
Symptoms
Anal cancer signs and symptoms include:
- Bleeding from the anus or rectum.
- Blood in the stool.
- Pain in the area of the anus.
- A mass or growth in the anal canal.
- Anal itching.
- Having to go to the bathroom more often.
When to see a doctor
Make an appointment with a doctor or other healthcare professional if you have any symptoms that worry you.
Causes
Anal cancer happens when cells in the anal canal develop changes in their DNA. A cell's DNA holds the instructions that tell a cell what to do. In healthy cells, the DNA gives instructions to grow and multiply at a set rate. The instructions tell the cells to die at a set time. In cancer cells, the changes give different instructions. The changes tell the cancer cells to make many more cells quickly. Cancer cells can keep living when healthy cells would die. This causes too many cells.
The cancer cells might form a mass called a tumor. The tumor can grow to invade and destroy healthy body tissue. In time, cancer cells can break away and spread to other parts of the body. When cancer spreads, it's called metastatic cancer.
Most anal cancers are thought to be caused by human papillomavirus, also called HPV. HPV is a common virus that's passed through sexual contact. For most people, the virus never causes problems. It usually goes away on its own. For some, though, the virus can cause changes in the cells that may lead to cancer.
Risk factors
Things that may increase the risk of anal cancer include:
- Being exposed to human papillomavirus, also called HPV. HPV is a common virus that's passed through sexual contact. For most people, it causes no problems and goes away on its own. For others, it causes changes in the cells that can lead to many types of cancer, including anal cancer.
- Increasing number of sexual partners. The greater your number of sexual partners, and the greater your partner's number of sexual partners, the greater your chance of acquiring HPV.
- Having anal sex. People who have receptive anal sex have an increased risk of anal cancer.
- Smoking cigarettes. People who smoke cigarettes have an increased risk of anal cancer.
- Having a history of cancer. Those who have had cervical, vulvar or vaginal cancer have an increased risk of anal cancer.
- Having a weak immune system. If the body's germ-fighting immune system is weakened by medicines or illness, there might be a higher risk of anal cancer. People with a weakened immune system include those taking medicines to control the immune system, such as after an organ transplant. Certain medical conditions, such as infection with HIV, also can weaken the immune system.
Complications
Anal cancer rarely spreads to other parts of the body. Only a small percentage of cancers are found to have spread. Those that do are especially difficult to treat. Anal cancer that spreads most commonly goes to the liver and the lungs.
Prevention
Take steps to reduce your risk
There is no sure way to prevent anal cancer. To reduce your risk of anal cancer:
- Practice safer sex. Reduce your risk of anal cancer by taking measures to prevent sexually transmitted infections. This may include using a condom every time you have sex and limiting the number of sexual partners you have.
- Consider the HPV vaccine. Receiving a vaccination to prevent HPV infection may reduce your risk of anal cancer and other HPV-related cancers. Ask your healthcare team if an HPV vaccine is right for you.
- Don't use tobacco. If you don't use tobacco, don't start. If you currently use tobacco of any kind, talk with a healthcare professional about strategies to help you quit.
Ask about anal cancer screening
Screening tests can help detect anal cancer and precancerous cells that may one day develop into anal cancer. Healthcare professionals sometimes recommend screening for people with a high risk of anal cancer.
You might have a high risk of anal cancer if you:
- Have HIV.
- Are taking medicine to control your immune system after an organ transplant.
- Have been diagnosed with precancerous cells in the penis, scrotum, cervix, vagina or vulva.
Screening tests might include:
- Anal Pap test. During an anal Pap test, a healthcare professional swabs cells from your anal canal. The cells are tested in a lab to check for cancer cells and cells that look like they could become cancerous.
- Anal HPV test. The anal HPV test involves testing cells from the anal canal for infection with HPV.
- Digital rectal exam. During a digital rectal exam, a healthcare professional inserts a gloved, lubricated finger into the anus. The health professional feels the anal canal and rectum for growths or other signs of cancer.
Medical groups don't agree on who should have anal cancer screening and what tests should be used. Screening can detect anal cancer when it's small and easier to treat. But studies haven't proved that anal cancer screening can save lives. Talk about the benefits and risks of screening with your healthcare team.
Nov. 29, 2023