Diagnosis
Liver biopsy
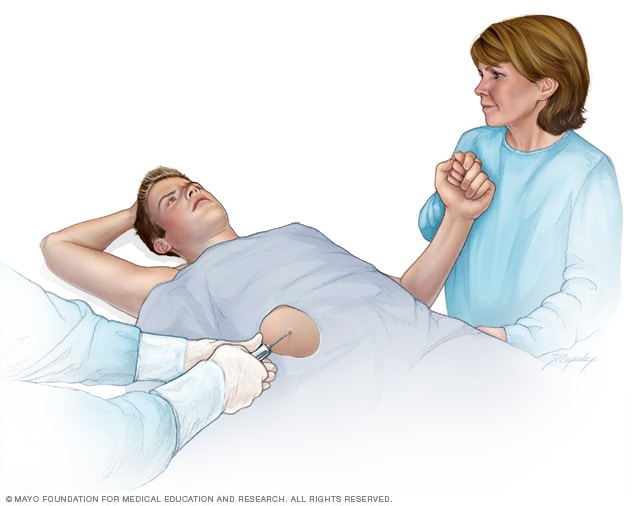
Liver biopsy
A liver biopsy removes a small sample of liver tissue for lab testing. A liver biopsy most often is done by putting a thin needle through the skin and into the liver.
Diagnosing alcoholic hepatitis typically starts with a physical exam and a conversation about how much alcohol a person drinks. To get the right diagnosis, it's important to be honest about alcohol use, now and in the past. Sometimes a healthcare professional might ask to talk to family members about a loved one's drinking.
Diagnosing alcoholic hepatitis also may involve these tests:
Liver enzymes and liver function tests (LFTs)
LFTs are blood tests that help your healthcare team understand how well your liver is working. These tests are especially important in diagnosing alcoholic hepatitis because they show signs of liver inflammation and damage.
In alcoholic hepatitis, typical results may include:
- Aspartate aminotransferase (AST) and alanine aminotransferase (ALT). A common finding is an AST to ALT ratio greater than 2 to 1, which suggests alcohol-related liver injury.
- Total bilirubin. High bilirubin levels can cause yellowing of the skin and eyes, called jaundice. This is a key sign of liver inflammation.
- International normalized ratio (INR) or prolonged prothrombin time (PT). High levels mean the liver isn't making enough clotting proteins, which increases bleeding risk.
- Albumin. Low albumin levels show poor liver function and possible malnutrition.
- Gamma-glutamyltransferase (GGT). This enzyme is often higher in alcohol-related liver disease.
These tests alone don't confirm alcoholic hepatitis, but they help guide the diagnosis when combined with symptoms, alcohol use history and other findings.
Blood tests
Other blood tests may be used to rule out viral hepatitis, such as hepatitis A, B or C, or autoimmune liver disease, which can cause similar symptoms. Additional tests may include iron studies or markers for conditions such as Wilson's disease or alpha-1 antitrypsin deficiency, depending on the situation.
Imaging tests
Tests such as ultrasound, CT or MRI can show liver size, fat buildup, scarring or other signs of liver disease. These tests also can help rule out bile duct issues or liver tumors.
Liver biopsy
If other tests don't provide a clear answer or if another condition might be causing liver inflammation, a liver biopsy may be done. This involves taking a small sample of liver tissue to examine under a microscope.
More Information
Treatment
Treating alcoholic hepatitis involves quitting drinking along with treatment to ease the symptoms of liver damage.
Quitting drinking
If you've been diagnosed with alcoholic hepatitis, you need to stop drinking alcohol and never drink alcohol again. In people with mild to moderate alcoholic hepatitis, quitting alcohol completely may give the liver a chance to heal and possibly reverse the damage. Some people begin to improve within weeks if they stop drinking and follow medical care.
In more-severe cases, stopping alcohol is still the most important step. But the damage may be harder, or impossible, to reverse. People who don't stop drinking are likely to have some life-threatening health issues.
If you want to stop drinking and want help, talk to a healthcare professional. It may be harmful to stop drinking all at once. Talk to your healthcare professional about a plan that's right for you.
Treatments that can help people stop drinking include:
- Medicines.
- Counseling.
- Alcoholics Anonymous or other support groups.
- Treatment programs.
Treatment to improve nutrition
Your healthcare professional might suggest a special diet to fix poor nutrition. You may be referred to an expert in diet to manage disease, called a dietitian. A dietitian can suggest ways to eat better to improve your diet.
If you have trouble eating, your health professional might suggest a feeding tube. A tube is passed down the throat or through the side and into the stomach. A liquid diet that's rich in nutrients is then passed through the tube.
Medicines to ease liver swelling
The following medicines may be used to help lower liver swelling, also called inflammation:
- Corticosteroids. These medicines might help some people with advanced alcoholic hepatitis live longer. However, corticosteroids can have serious side effects. They're not likely to be used if you have failing kidneys, stomach bleeding or an infection.
- Other treatment. A medicine called N-acetylcysteine may help some people with alcoholic hepatitis. More studies are needed. There may be clinical trials available.
Liver transplant for alcoholic hepatitis
For many people with advanced alcoholic hepatitis, the risk of dying is high without a liver transplant.
In the past, people with alcoholic hepatitis typically weren't offered liver transplants. That was due to concern that they might keep drinking after a transplant. But studies now suggest that in carefully selected people with advanced alcoholic hepatitis, survival rates after a transplant are similar to people with other types of liver disease who get liver transplants.
How long does alcoholic hepatitis last?
The length of time alcoholic hepatitis lasts depends on how severe it is and whether a person stops drinking. Mild or moderate alcoholic hepatitis symptoms may improve within a few weeks to months if the person stops drinking and gets medical care. In some people, liver function may return to near normal.
However, severe alcoholic hepatitis can last much longer and may cause permanent liver damage. Even after the initial illness improves, many people continue to have complications such as fluid buildup or confusion. In one study, only 7% of people with severe alcoholic hepatitis fully recovered to a stable condition without complications, even after more than two years.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Preparing for your appointment
If you have any symptoms that worry you, start by making an appointment with a doctor or other healthcare professional. If your healthcare professional suspects that you have alcoholic hepatitis, you may be referred to a digestive disease specialist, called a gastroenterologist.
What you can do
When you make the appointment, ask if there's anything you need to do before certain tests, such as not eating or drinking.
Make a list of:
- Your symptoms, including any that don't seem linked to the reason you made the appointment, and when they began.
- All medicines, vitamins and supplements you take, including doses.
- Key medical information, including other conditions you have.
- Key personal information, including recent changes or stressors in your life. Keep track of how much alcohol you drink for a few days before your appointment.
- Questions to ask your healthcare professional.
Have a family member or friend go with you, if possible, to help you remember the information you're given.
Questions to ask your doctor
- What's the most likely cause of my symptoms? Are there other possible causes?
- Do I have any other liver disease?
- Is there scarring of my liver?
- What tests do I need? How do I prepare for them?
- Is my condition likely to go away or be long-lasting?
- What treatment do you suggest?
- I have other health problems. How can I best manage these conditions together?
Be sure to ask all the questions you have about your condition.
What to expect from your doctor
Your healthcare professional is likely to ask you questions, including:
- How bad are your symptoms? Do they come and go, or do you have them all the time?
- Does anything improve your symptoms or make them worse?
- Have you had hepatitis or yellowing of the skin or whites of your eyes?
- Do you use drugs that are not legal?
- Have you ever felt you should cut down on drinking or felt guilty or bad about your drinking?
- Are your family members or friends worried about your drinking? Have you been arrested or had other problems because of your drinking?
- Do you get angry or upset when anyone talks about your drinking?
- Do you feel guilty about drinking?
- Do you drink in the morning?
Jan. 27, 2026