Overview
In telestroke medicine — also called stroke telemedicine — health care providers who have advanced training in treating strokes can use technology to treat people who've had strokes in another location. These stroke experts work with local emergency health care providers to recommend a diagnosis and treatment.
The stroke specialists communicate with local health care providers and the people needing care using digital cameras, internet telecommunications, smartphones, tablets and other technology. They also may use robotic telepresence, which gives providers a remote presence through the use of a robot.
Stroke telemedicine operates on a distant-site and originating-site system. Stroke experts at the distant site are usually at a large urban medical center. The medical center that serves as the distant site is typically certified as a primary or comprehensive stroke center. Remote locations, often smaller regional hospitals, serve as the originating site.
In telestroke medicine, many people work together as a team. Members of the team at the distant site usually include a program manager, a clinical coordinator, vascular neurologists, neurosurgeons and radiologists. Members at the originating site include emergency health care providers and other staff. Radiology technicians, informational technology staff, researchers, nurses, nurse practitioners and other staff also are important members of the telestroke team.
Products & Services
Why it's done
In stroke telemedicine, your health care provider and the stroke expert at the distant site work together to provide quality stroke care in your community. This means there's a lower chance you'll need to be transferred to another medical center if you have a stroke.
Many regional hospitals don't have neurologists on call to recommend the most appropriate stroke care. In stroke telemedicine, a stroke expert at the distant site consults live with health care providers and people who've had strokes at the originating remote site.
This is important because getting a prompt diagnosis and a treatment recommendation is crucial after a stroke. It increases the chances that clot-dissolving therapies called thrombolytics can be delivered in time to reduce stroke-related disability. The therapies must be given through an IV within four and a half hours after you experience stroke symptoms.
Procedures to dissolve clots may be considered within 24 hours of stroke symptoms. These require being transferred from the originating to the distant site.
What you can expect
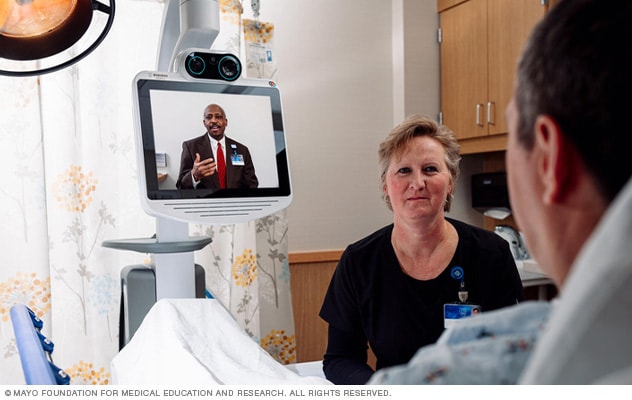 Telestroke consultation
Telestroke consultation
Your health care provider performs a live, real-time consultation with video and sound with the stroke expert at the distant hospital.
During a stroke telemedicine consultation, an emergency health care provider at your regional hospital will examine you. If your provider suspects that you've had a stroke, the provider will activate the stroke telemedicine hotline at the distant hospital. The stroke telemedicine hotline triggers a group paging system to contact stroke experts on call 24 hours a day, 365 days a year. The stroke expert at the distant site usually responds within five minutes.
After you have a CT scan, the stroke expert at the distant site performs a live, real-time consultation with video and sound. You'll likely be able to see, hear and speak with the expert. The stroke specialist may discuss your medical history and review your test results.
The stroke specialist evaluates you and works with your health care provider to create the most appropriate treatment plan. The stroke expert sends treatment recommendations electronically to the originating hospital.
Jan. 18, 2023