Feb. 20, 2021
A sizable number of Mayo Clinic's orthopedic surgeons are active duty veterans or reservists who have been deployed overseas. Mayo's military connections serve not only members of the armed forces but also civilian patients once the surgeons return to Mayo.
"The acuity of injuries we see at Mayo, and our patient volumes, make us well prepared for deployment. We also can take new techniques from our military experience back home," says Nicholas A. Pulos, M.D., a hand surgeon at Mayo Clinic in Rochester, Minnesota, who recently returned from deployment to Kandahar, Afghanistan.
Mayo's ties to military service stretch back to Dr. William Worrall Mayo, who began his medical practice in Rochester in 1864 as an examining physician for Civil War enlistees. Dr. Pulos, who serves in the United States Navy Reserve, notes that hand surgery emerged as a medical specialty after World War II due to the wartime need for reconstructive surgeries. In addition to hand surgeons, orthopedic surgeons at Mayo Clinic specializing in the spine and hip, as well as plastic surgeons and other specialists, have military experience.
As a salaried organization with a strong founding culture, Mayo Clinic pursues a team-based approach to care. "We put our patients' interests first and work together as a team rather than as individuals to deliver the care they need," says Brett A. Freedman, M.D., an orthopedic surgeon at Mayo's campus in Minnesota, and a decorated United States Army veteran. "We take our Mayo values with us on deployment, and they blend perfectly well with the military."
With a large orthopedic practice, Mayo Clinic can transition patients to care from other experienced specialists when staff are deployed. "Even though all Mayo employees aren't able to serve in a combat zone, they do contribute by helping their colleagues and families while the deployed physicians are overseas," says Paul M. Huddleston III, M.D., an orthopedic surgeon at Mayo's campus in Minnesota and a decorated United States Army veteran who has served several deployments in Iraq and Afghanistan.
"Mayo is very supportive of deployment," Dr. Pulos adds. "As an all-volunteer force, the military relies on reservists, including physicians at Mayo Clinic, to go out on active duty and help service members."
Trauma-related expertise
Improved body armor has helped service personnel survive injuries that might have been fatal in previous conflicts. "A lot of the injuries we see on deployment involve the extremities because the body armor is so good," Dr. Pulos says. "About 50% of the surgeries I did in Afghanistan involved the hand."
Harvested groin flap covers palmar defect
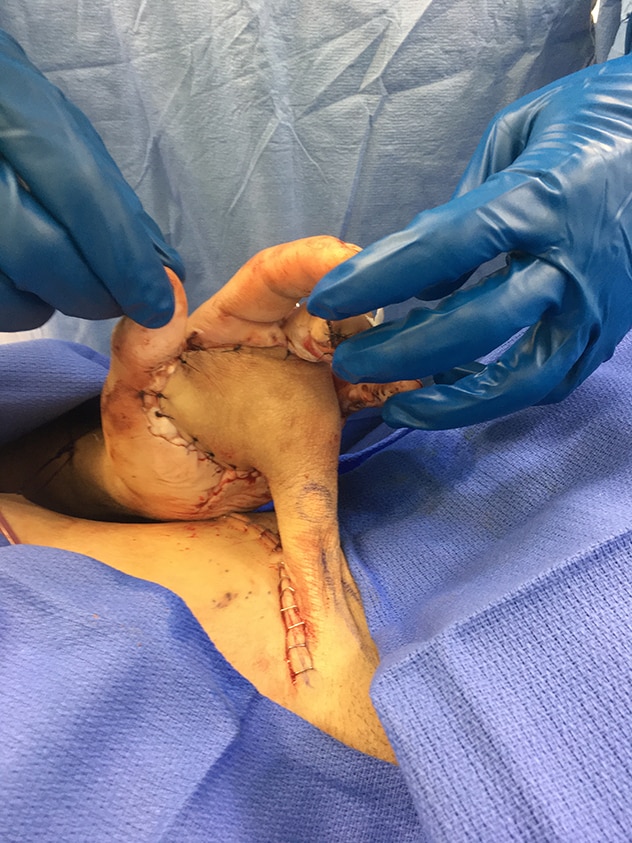
Harvested groin flap covers palmar defect
Photograph shows the hand of a wounded serviceman following treatment in Afghanistan by Nicholas A. Pulos, M.D., a Mayo Clinic hand surgeon on deployment with the United States Navy Reserve. A blasting cap injury had mutilated the hand. Working with military colleagues, Dr. Pulos harvested a groin flap to cover the palmar defect.
Mayo Clinic has a sizable orthopedic trauma practice. "The Mayo expertise is really helpful in thinking of creative ways to do orthoplastics on deployment," Dr. Pulos says. "We have experience using regional flaps and soft tissue transfers to reconstruct upper extremities after traumatic injuries."
That expertise facilitates immediate definitive treatment for service members. "Typically, service members with serious injuries in Afghanistan are stabilized and then sent back to the United States," says Peter C. Rhee, D.O., a hand surgeon at Mayo's campus in Minnesota and a United States Air Force reservist. "Military physicians are very skilled. But for a majority of trauma-related injuries out there, the Mayo surgeon may be the only person who can provide definitive treatment."
That capability is especially beneficial for local citizens who become injured while helping the United States military. "We can't send those local nationals to the United States for care," Dr. Rhee says. "But those patients can have a Mayo Clinic-trained surgeon, in the most austere environment, where normally they wouldn't have access to any surgeon."
At the same time, Mayo's surgeons learn new skills on deployment that can ultimately benefit patients back in the United States. Dr. Pulos cites the military's use of perioperative tranexamic acid and tourniquets to control bleeding. "Tourniquets weren't as popular in civilian practice," he says. "But their use in military practice has trickled down to medical practice in the civilian sector."
Mayo Clinic physicians have also published extensively on the orthopedic issues encountered on deployment. "As military surgeons, our work contributes to knowledge of lifesaving developments supporting the war effort," Dr. Huddleston says. "Our experience with combat-related spinal fractures and injuries helps us understand and treat these issues today."
Dr. Freedman's military service led to published research on topics including spinal care, compartment syndrome diagnosis and wound healing. As a first-year resident at Walter Reed Army Medical Center, he was motivated by the traumatic injuries he saw in Pentagon personnel after the attack on Sept. 11, 2001, and in soldiers and sailors who returned from war with catastrophic spine and limb injuries.
"The extremity injuries we have seen in war today have really pushed the envelope," he says. "The use of biologics and enhanced methods of bone healing, and the development of new implants and wound care devices all owe something to those experiences. We are always looking to innovate and find a better way."
Dr. Freedman notes that Mayo Clinic is exploring further ties with the military through a program that would bring military medical personnel to a Mayo campus to work alongside Mayo specialists. "The idea is to give the military personnel the Mayo experience," he says. "The benefits for Mayo and the military are definitely bidirectional. As Mayo surgeons, we give to the military but we also take back the experience of how a team can work together in an austere location when you don't have all the resources you want."