Oct. 01, 2021
Dry eye disease is a common condition causing ocular discomfort, reduced visual acuity and impaired quality of life. Meibomian gland dysfunction is the most common cause of dry eye disease: Abnormal meibum obstructs meibomian glands and causes altered tear film, which can result in eye irritation, ocular surface disease, inflammation and bacterial overgrowth.
"When meibomian gland dysfunction is treated early, there is potential for the return of gland function. However, many of the current therapies only treat the symptoms of dry eye disease rather than addressing the underlying pathophysiology of meibomian gland dysfunction," says Joanne F. Shen, M.D., chair of Ophthalmology at Mayo Clinic in Phoenix/Scottsdale, Arizona.
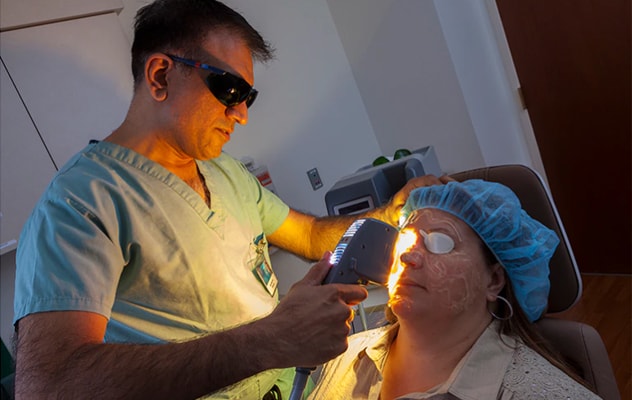 Treatment with intense pulsed light
Treatment with intense pulsed light
Dharmendra (Dave) R. Patel, M.D., an ophthalmologist at Mayo Clinic in Phoenix/Scottsdale, Arizona, treats a patient with intense pulsed light.
Meibomian gland expression (MGX) is a relatively inexpensive and readily available treatment option that requires minimal equipment and has proved efficacious in patients with dry eye related to meibomian gland dysfunction. However, it is often painful and requires frequent treatment sessions. Intense pulsed light (IPL) combined with MGX is a recognized treatment for ocular rosacea and meibomian gland disease with dry eye symptoms, but "despite the growing acceptance of IPL in ophthalmology, the mechanism by which it improves dry eye symptoms is not fully understood and the treatment is not widely available," says Dr. Shen.
Dr. Shen and fellow researchers investigated the efficacy and mechanism of IPL in ocular rosacea with dry eye symptoms by evaluating symptoms and signs and analyzing tear film transforming growth factor-beta (TGF-β) and ocular microbiome changes in patients receiving IPL with MGX compared with MGX alone. Results were published in Clinical Ophthalmology in 2021.
For this pilot study, 20 patients with a greater than one-year history of ocular rosacea with meibomian gland dysfunction and dry eye disease were recruited from November 2017 through September 2018 and randomly assigned to receive either IPL-MGX or MGX. Patients were examined, treated and administered the Ocular Surface Disease Index survey every 4 to 6 weeks for four total treatments. Tear film and conjunctival samples were collected at first and last visits and analyzed for TGF-β concentration and 16s rRNA amplicon sequencing of ocular microbiome.
Ocular Surface Disease Index survey results
Mean baseline Ocular Surface Disease Index scoring was equivalent between the IPL-MGX and the MGX treatment groups (55.7 versus 43.5, P = 0.212). By the fourth visit, scores were significantly improved from baseline in the IPL-MGX treatment group compared with the group that received MGX alone (P = 0.030).
The number of meibomian glands yielding liquid secretions increased from baseline to visit 4 in both groups. The increase was greater in the IPL-MGX group, though not different enough to achieve statistical significance in this small cohort.
Dermatology literature has reported elevation in TGF-β1 in patients with back acne treated with IPL, so an association was investigated in the patients with ocular rosacea. However, there was no significant difference in mean TGF-β1, TGF-β2 or TGF-β3 concentration after IPL-MGX (P = 0.385, 0.709 and 0.948, respectively). Ocular microbiome was examined, but though quantities of clostridium, klebsiella, brevibacterium, lactobacillus, neisseria, streptococcus, corynebacterium, butyricicoccus and actinomyces were significantly reduced from baseline in both groups, there was no significant difference between the two treatment groups.
Dr. Shen concludes: "Refractory dry eye symptoms can be extremely debilitating. There is an array of treatments offered to patients with dry eye, many of which are not covered by insurance and lack any guarantee of improvement. Patients who have ocular rosacea and respond to doxycycline but are intolerant to this systemic treatment are good candidates for this out-of-pocket cost treatment. Patients with refractory red eyes from ocular rosacea also have responded well. Understanding the mechanism of IPL on dry eye from ocular rosacea will both enable providers to identify other patients as good candidates based on their individual traits and open the door to investigating additional therapeutic interventions."
For more information
Sagaser S, et al. Effects of intense pulsed light on tear film TGF-β and microbiome in ocular rosacea with dry eye. Clinical Ophthalmology. 2021;15:323.