Feb. 14, 2020
Artificial intelligence (AI) is emerging as a tool with which gastroenterologists can improve colon polyp detection rates, characterization and management. This branch of computer science attempts to mimic the intelligence and behavior of human beings.
A process called deep learning is integral to the development of AI tools in gastroenterology, especially in imaging technologies. AI tools use general purpose algorithms specialized through training to perform tasks such as image classification and enhancement, diagnosis, or outcomes prediction. These deep neural networks analyze large, previously annotated datasets of images to learn in an iterative fashion. And with ongoing use, they get smarter.
Flat polyp commonly missed by endoscopists
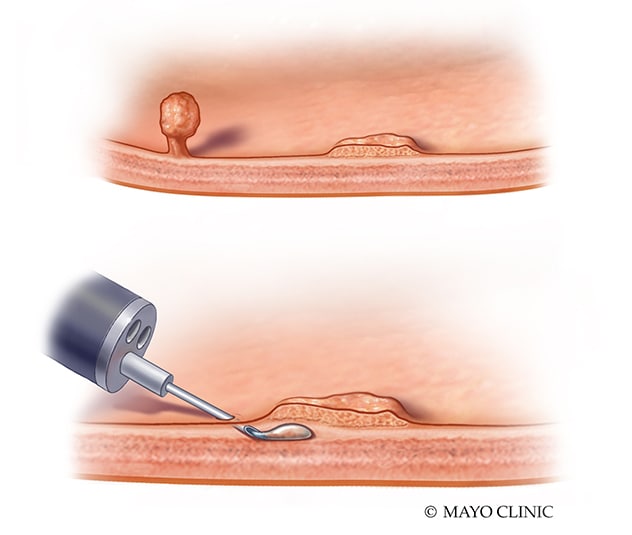
Flat polyp commonly missed by endoscopists
AI deep learning tools may be particularly helpful in detection of certain types of polyps, such as flat and serrated lesions, that are more commonly missed by endoscopists.
An article published in Endoscopy in 2012 noted that up to 25% of polyps can be missed during colonoscopy. Factors related to these misses include withdrawal time, preparation quality and endoscopist-specific variables, such as the extent of lining visualized and the ability to recognize flat polyps.
Computer-aided polyp detection systems using deep learning have been shown to increase the ability of endoscopists to detect polyps and aid in their characterization during routine screening and surveillance colonoscopy. In an article published in Gut in 2019, researchers prospectively examined the effect of a computer-aided polyp detection system based on deep learning on polyp detection rate and adenoma detection rate (ADR). Most of the additional polyps identified were small and hyperplastic, thus limiting the clinical relevance of the study. But the authors demonstrated that the computer-aided diagnosis system yielded a significantly higher ADR than those achieved with standard colonoscopy (29.1% versus 20.3%, p < 0.001) and a higher mean number of adenomas detected per patient as well (0.53 versus 0.31, p < 0.001).
According to Nayantara Coelho Prabhu, M.B.B.S., AI deep learning tools may be particularly helpful in detection of certain types of polyps, such as flat and serrated lesions, that are more commonly missed by endoscopists.
Dr. Coelho Prabhu is a gastroenterologist at Mayo Clinic's campus in Rochester, Minnesota, whose research focuses on endoscopy. AI tools can also provide endoscopists with objective data that indicate whether they are performing a high-quality colonoscopy. "These tools can account for variables such as prep quality, segments of colon visualized and completeness of examination," explains Dr. Coelho Prabhu.
Use of AI tools in patients with inflammatory bowel disease (IBD) is another area of interest because of the difficulties associated with polyp detection in patients with mucosal inflammation.
"Because IBD increases an individual's risk of colorectal cancer, the potential utility of AI to enhance polyp detection in these patients is very exciting," explains Dr. Coelho Prabhu. "Once they are trained on adequate images, AI systems will be able to help gastroenterologists identify areas of higher risk of dysplasia and preneoplastic changes in these colons."
Role of AI in polyp classification and management
Characterization of polyps, as premalignant adenomatous or serrated lesions versus benign hyperplastic lesions, is an important feature of currently available AI
systems. "This differentiation is important because it determines the patient's colon cancer risk and the surveillance intervals. The currently available tools for classification are yet to be perfected but show potential for future development," says Dr. Coelho Prabhu.
Newer AI technologies are emerging that may have the potential to help endoscopists determine the depth of submucosal invasion of various parts of a lesion. "The information provided by these tools could help endoscopists determine whether a simple mucosal resection versus a deeper submucosal dissection of the lesion is required to ensure complete removal," explains Dr. Coelho Prabhu.
Dr. Coelho Prabhu notes that AI can be trained to help endoscopists identify the margin of polyps, which can sometimes be difficult to identify, especially in lesions that spread laterally. "Training AI on various filtered-light images will improve the tool's accuracy and specificity," explains Dr. Coelho Prabhu. "And with deep learning, the AI systems will continue to learn while they are being implemented, to improve and yield more fine-tuned results."
Dr. Coelho Prabhu notes that AI tools can also be trained to perform the following tasks:
- Outline polyps before resection and identify residual preneoplastic tissue to guide the complete resection of the adenomatous tissue that is required to prevent recurrence
- Standardize the quality of exams and guide accurate follow-up intervals
- Identify patients who are at higher risk of complications during resection, including bleeding, cardiorespiratory complications and perforation
AI in GI at Mayo Clinic
Dr. Coelho Prabhu notes that Mayo Clinic is well positioned to develop and validate AI tools. "Our depth of highly specialized physicians in each field of gastroenterology and the high volume of patients we see and treat both make our organization uniquely suited to this vein of research."
Having well-annotated datasets that can be used to train AI tools is an essential component in building effective and accurate AI tools. "We have records from a large volume of procedures performed, and we are working to create a rich database of high-quality images and videos needed to support AI tools. This work will position us at the forefront of AI tool development," says Dr. Coelho Prabhu.
Dr. Coelho Prabhu and colleagues are currently focused on using AI to help accurately identify the precise location of polyps and cancer in the colon to aid surgeons in cases where resection is needed, and to improve surveillance efforts, especially when these lesions are endoscopically resected.
Mayo Clinic researchers are also conducting clinical trials involving advanced imaging techniques, including the use of AI tools and blue light imaging, narrow band imaging, and colon capsule endoscopy.
Dr. Coelho Prabhu anticipates that AI tools will be used regularly in the clinical setting within the next five years to guide endoscopy (including colonoscopy), esophagogastroduodenoscopy, capsule enteroscopy, endoscopic ultrasound and endoscopic retrograde cholangiopancreatography. "I also expect to see AI employed to optimize procedure scheduling, for diagnosis augmentation and to guide surveillance," says Dr. Coelho Prabhu.
"Overall, the advances provided by AI-based learning can help us determine the best treatment option for each patient, and this will enhance our ability to offer patients truly individualized therapeutic approaches," says Dr. Coelho Prabhu.
For more information
Leufkens AM, et al. Factors influencing the miss rate of polyps in a back-to-back colonoscopy study. Endoscopy. 2012;44:470.
Wang P, et al. Real-time automatic detection system increases colonoscopic polyp and adenoma detection rates: A prospective randomised controlled study. Gut. 2019;68:1813.