Overview
A spinal cord injury involves damage to any part of the spinal cord. The spinal cord sends and receives signals between the brain and the rest of the body. A spinal cord injury often causes permanent changes in strength, sensation and other body functions below the site of the injury. It also may lead to loss of strength, called paralysis.
People who have had a spinal cord injury also may have mental, emotional and social side effects from the injury.
Many scientists are optimistic that advances in research someday will make repair of spinal cord injuries possible. Research into spinal cord injuries is going on around the world. In the meantime, treatments and rehabilitation allow many people with spinal cord injuries to lead productive, independent lives.
Products & Services
Symptoms
Spinal cord injuries
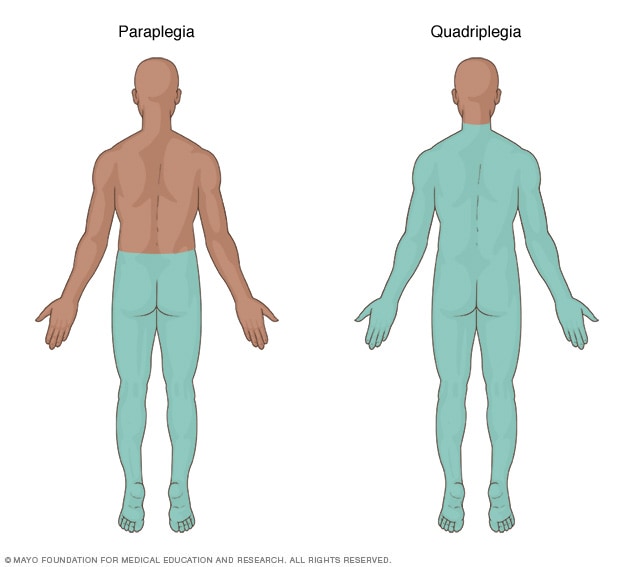
Spinal cord injuries
Paralysis of the lower half of the body is called paraplegia. Paralysis below the neck, including both arms and legs, is called quadriplegia.
Spinal cord injuries can cause the following symptoms:
- Loss of strength, called paralysis.
- Loss of or a change in sensation. This includes a change in the ability to feel heat, cold and touch. It also may affect balance.
- Loss of bowel or bladder control.
- Spasms or strong reflex movements.
- Changes in sexual function and sexual sensitivity.
- Pain or an intense stinging sensation caused by damage to the nerve fibers in the spinal cord.
- Trouble breathing, coughing or clearing the lungs.
Emergency symptoms
Emergency symptoms of a spinal cord injury after an accident include:
- Serious back pain or pressure in the neck, head or back.
- Weakness, loss of coordination or loss of control in any part of the body.
- Numbness, tingling or loss of feeling in the hands, fingers, feet or toes.
- Loss of bladder or bowel control.
- Trouble with balance and walking.
- Trouble breathing after the injury.
- A twisted neck or back.
Movement and feeling after a spinal cord injury
The ability to control the arms or legs after a spinal cord injury depends on two factors. The first factor is where the injury happened on the spinal cord. The second factor is how bad the injury is.
The lowest part of the spinal cord not damaged after an injury is known as the neurological level of the injury. Completeness of the injury is classified as:
- Complete. If all feeling and all ability to control movement are lost below the spinal cord injury, the injury is called complete.
- Incomplete. If some feeling and control of movement remain below the injury, the injury is called incomplete. There are varying degrees of incomplete injury.
A loss of muscle strength that leads to loss of movement is called paralysis. Paralysis from a spinal cord injury can be referred to as:
- Quadriplegia, also known as tetraplegia. This means that the arms, hands, trunk, legs and pelvic organs are all affected by the spinal cord injury.
- Paraplegia. This paralysis affects all or part of the trunk, legs and pelvic organs. But it doesn't affect the arms.
The healthcare team does a series of tests to find the neurological level and completeness of a spinal cord injury.
When to see a doctor
Anyone who has an injury to the head or neck needs medical attention right away. It is safest to assume that the person has a spinal injury until proven otherwise. This is important because:
- A serious spinal injury is not always easy to see right away. If a spinal injury happens but it is not cared for, worse injury may happen.
- Numbness or paralysis can happen quickly or come on slowly.
- The time between injury and treatment can be critical. Learning the level of the injury can help determine the possible recovery.
If you think that someone has a back or neck injury:
- Do not move the injured person. Permanent paralysis and other serious health issues can result.
- Call 911 or local emergency medical help.
- Keep the person still.
- Place heavy towels on both sides of the neck. Or hold the head and neck to keep them from moving until emergency medical help arrives.
- Provide basic first aid, such as stopping bleeding and making the person comfortable, without moving the head or neck.
Causes
Central nervous system
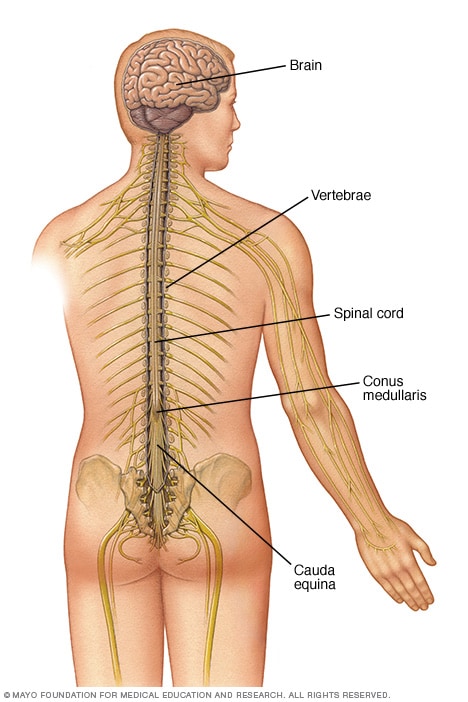
Central nervous system
The spinal cord extends downward from the base of the brain. It's made up of nerve cells and groups of nerves that carry messages between the brain and the rest of the body.
Spinal cord injuries can be caused by damage to the spinal cord itself or damage to the bones that surround the spinal cord, called the vertebrae. Injuries also may happen because of damage to the ligaments or disks of the spinal column.
A sudden blow to the spine can break, dislocate, crush or compress one or more of the vertebrae. A gunshot or knife wound that is at or near the spinal cord also can cause a spinal cord injury.
Common causes of spinal cord injuries include:
- Motor vehicle accidents. Auto and motorcycle accidents cause many spinal cord injuries each year.
- Falls. A spinal cord injury after age 65 often is caused by a fall.
- Acts of violence. Spinal cord injuries can result from violent encounters, typically from gunshot wounds. Knife wounds also can cause spinal cord injuries.
- Sports and recreation injuries. Athletic activities, such as impact sports and diving in shallow water, can lead to spinal cord injuries.
- Medical conditions. Arthritis, cancer, inflammation, infection and osteoporosis of the spinal cord can cause spinal cord injuries. Breakdown of disks in the spinal column, called disk degeneration, also can damage the spinal cord.
In the days and weeks after a spinal cord injury, more damage can happen. That damage may be due to bleeding, swelling and fluid buildup in and around the spinal cord after an injury.
The central nervous system
The body's central nervous system includes the brain and spinal cord. The spinal cord is made of soft tissue. Bones called vertebrae surround it. The spinal cord goes from the base of the brain to an area just above the waist called the conus medullaris. Below that area is a group of nerve roots called the cauda equina. Nerve roots are bundles of nerve fibers that come out of the spinal cord and join to form nerves.
The spinal cord has nerve cells and groups of nerves called tracts. The tracts go to different parts of the body and carry messages to and from the brain. Motor tracts carry signals from the brain that control muscle movement. Sensory tracts carry signals from the body to the brain focused on heat, cold, pressure, pain, and the position of the arms and legs.
Damage to nerve fibers
A spinal cord injury damages the nerve fibers that pass through the injured area. That nerve fiber damage can make it hard for part of or all of the muscles and nerves below the injury to work correctly.
An injury to the spine at the chest level or in the lower back can affect the trunk, legs, bowel, bladder and sexual function. A neck injury affects the same areas plus movements of the arms and possibly the ability to breathe.
Risk factors
The following factors can raise the risk of a spinal cord injury:
- Being male. Many more men than women have spinal cord injuries.
- Being between the ages of 15 and 29. More than half of spinal cord injuries happen in people in this age range.
- Being 65 and older. People older than 65 also are at higher risk. Falls cause most spinal cord injuries in older adults.
- Driving. Motor vehicle crashes are the leading cause of spinal cord injuries for people younger than 65.
- Using alcohol. Alcohol use is involved in many spinal cord injuries.
- Engaging in unsafe behavior. Any behavior that puts the head or neck in danger raises the risk of a spinal cord injury. Examples include diving into shallow water and playing sports without wearing safety gear or without taking other safety measures.
- Having certain medical conditions. A minor injury can cause spinal cord damage in people who have conditions that affect the joints or bones, such as osteoporosis. Other medical conditions also can raise the risk of spinal cord injuries, including arthritis, cancer, inflammation, infection and breakdown of disks in the spinal column, called disk degeneration.
Complications
A spinal cord injury can lead to many other health concerns, called complications. Complications can fall into several categories.
Breathing
If the injury affects the nerves to the stomach and chest muscles, it may be hard to breathe and cough. The neurological level of injury determines what kind of breathing problems a person with a spinal cord injury may have. If the injury affects the neck and chest, that could raise the risk of pneumonia or other lung conditions.
Blood flow
A spinal cord injury may lead to low blood pressure when a person gets up from sitting or lying down. This condition is called orthostatic hypotension. It also can cause swelling in the arms and legs. This can raise the risk of developing blood clots, such as deep vein thrombosis or a pulmonary embolus. Another issue with blood flow is a potentially life-threatening rise in blood pressure, known as autonomic dysreflexia.
Bladder
The bladder continues to store urine from the kidneys after a spinal cord injury. But the injury may make it hard for the brain to get the messages it needs to control the bladder. Changes in bladder control raise the risk of urinary tract infections. The changes also may cause kidney infections and kidney or bladder stones.
Bowels
The stomach and intestines work much like they did before the injury, but control of bowel movements often changes.
Skin
Below the neurological level of a spinal cord injury, some or all skin sensations may be lost. If that happens, the skin can't send a message to the brain when it's injured by certain things such as too much pressure. This can raise the risk of getting pressure sores.
Bones
A spinal cord injury raises the risk of osteoporosis and broken bones below the level of injury.
Muscles
Some people with spinal cord injuries have a tightening of muscles or motion in the muscles, called spasticity.
Fitness and wellness
Muscle loss, called atrophy, and weight loss are common soon after a spinal cord injury. Because limited mobility can lead to a less active lifestyle, there also is a risk of weight gain, heart disease and diabetes.
Sexual health
A spinal cord injury may lead to issues with sexual health. This may include changes in erection and ejaculation or changes in lubrication.
Pain
After a spinal cord injury, some people have pain, such as muscle or joint pain, from using certain muscle groups too much. Nerve pain also can happen after a spinal cord injury, especially in someone with an incomplete injury.
Depression
Pain and the changes a spinal cord injury brings may be linked to depression in some people.
Prevention
The following steps may help prevent a spinal cord injury:
-
Drive safely. Motor vehicle crashes are one of the most common causes of spinal cord injuries. Wear a seat belt every time you are in a moving vehicle.
Make sure children wear seat belts or use child safety seats that are made for their age and weight. To protect them from air bag injuries, children younger than 12 should always ride in the back seat.
- Check water depth before diving. Don't dive into a pool unless it's at least 9 feet (about 2.74 meters) deep and clearly marked safe for diving. Competition diving requires greater water depth. Don't dive into a pool that's above ground or into water if you don't know how deep it is.
- Prevent falls. Use a step stool with a grab bar to reach objects on high shelves. Add handrails along stairways. Put mats that won't slip on tile floors and in the bathtub or shower. For young children, use safety gates to block stairs and think about putting in window guards.
- Play sports safely. Always wear safety gear recommended for your sport. Don't lead with your head in sports. For example, don't slide headfirst in baseball. In American football, don't tackle using the top of your helmet. Use a spotter for new moves in gymnastics.
- Don't drink and drive. Don't drive after drinking alcohol or while under the influence of drugs. Don't ride with a driver who has been drinking or using drugs.