Diagnosis
Tests and procedures used to diagnose Paget's disease of the breast include:
- Breast exam. Your doctor will check both of your breasts and the lymph nodes in your armpit, feeling for any lumps or other abnormalities.
- Mammogram. A mammogram is an X-ray of the breast. Mammograms are commonly used to screen for breast cancer. If an abnormality is detected on a screening mammogram, your doctor may recommend a diagnostic mammogram to further evaluate that abnormality.
- Breast ultrasound. Ultrasound uses sound waves to produce images of structures deep within the body. Ultrasound may be used to determine whether a new breast lump is a solid mass or a fluid-filled cyst.
- Breast magnetic resonance imaging (MRI). An Magnetic resonance imaging (MRI) machine uses a magnet and radio waves to create pictures of the interior of your breast. Before a breast MRI, you receive an injection of dye.
- Removing a sample of breast cells for testing (biopsy). During a biopsy, your doctor removes a sample of suspicious tissue. Biopsy samples are sent to a laboratory for analysis to determine whether the cells are cancerous. A biopsy sample is also analyzed to determine the type of cells involved in the breast cancer, the aggressiveness (grade) of the cancer, and whether the cancer cells have hormone receptors or other receptors that may influence your treatment options.
Other tests and procedures may be used depending on your situation.

Receiving a mammogram
During a mammogram, you stand in front of an X-ray machine designed for mammography. A technician places your breast on a platform and positions the platform to match your height. The technician helps you position your head, arms and torso to allow an unobstructed view of your breast.

Core needle biopsy
A core needle biopsy uses a long, hollow tube to obtain a sample of tissue. Here, a biopsy of a suspicious breast lump is being done. The sample is sent to a lab for testing and evaluation by doctors, called pathologists. They specialize in analyzing blood and body tissue.
Treatment
If you have Paget's disease of the breast, you will likely need surgery. The type of surgery depends on the condition of the skin around your nipple and how advanced the underlying cancer is.

Mastectomy
During a total (simple) mastectomy, the surgeon removes the breast tissue, nipple, areola and skin. Other mastectomy procedures may leave some parts of the breast, such as the skin or the nipple. Surgery to create a new breast is optional and can be done at the same time as your mastectomy surgery or it can be done later.
Surgical options include:
- Removing the entire breast (mastectomy). A mastectomy is an operation to remove all of your breast tissue. Most mastectomy procedures remove all of the breast tissue — the lobules, ducts, fatty tissue and some skin, including the nipple and areola (total or simple mastectomy).
- Removing the breast cancer (lumpectomy). During a lumpectomy, which may be referred to as breast-conserving surgery or wide local excision, the surgeon removes the cancer and a small margin of surrounding healthy tissue. If you and your doctor choose this option, you will also receive radiation therapy afterward.
-
Removing a limited number of lymph nodes (sentinel node biopsy). To determine whether cancer has spread to your lymph nodes, your surgeon will discuss with you the role of removing the lymph nodes that are the first to receive the lymph drainage from your cancer.
If no cancer is found in those lymph nodes, the chance of finding cancer in any of the remaining lymph nodes is small and no other nodes need to be removed.
- Removing several lymph nodes (axillary lymph node dissection). If cancer is found in the sentinel lymph nodes, your surgeon will discuss with you the role of removing additional lymph nodes in your armpit.
- Removing both breasts. Some people with cancer in one breast may choose to have their other (healthy) breast removed (contralateral prophylactic mastectomy) if they have a very increased risk of cancer in the other breast because of a genetic predisposition or strong family history.
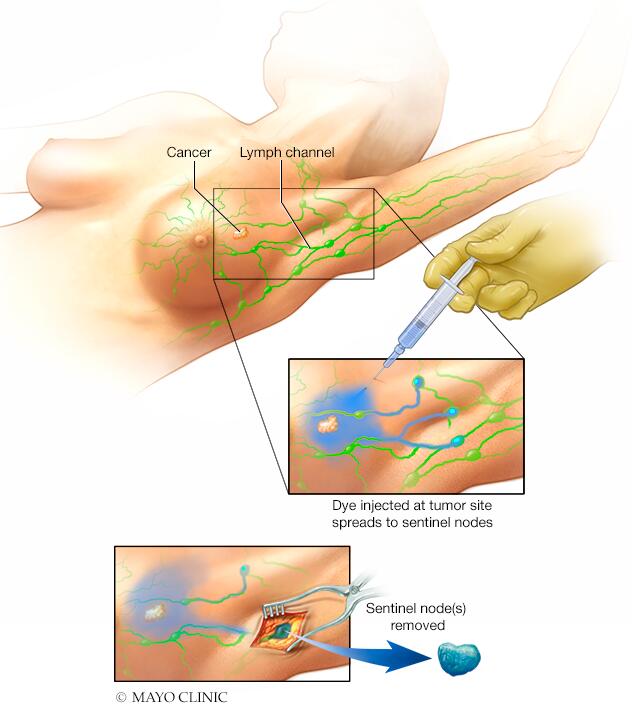
Sentinel node biopsy
Sentinel node biopsy identifies the first few lymph nodes into which a tumor drains. The surgeon uses a harmless dye and a weak radioactive solution to locate the sentinel nodes. The nodes are removed and tested for signs of cancer.
You may choose to have breast reconstruction after surgery. Discuss your options and preferences with your surgeon.
Consider a referral to a plastic surgeon before your surgery. Your options may include reconstruction with a breast implant or reconstruction using your own tissue. These operations can be performed at the time of your mastectomy or at a later date.
Adjuvant therapy
After your operation, your doctor may recommend additional treatment (adjuvant therapy) with anti-cancer drugs (chemotherapy), radiation therapy or hormone therapy to prevent a recurrence of breast cancer.
Your specific treatment will depend on the extent of the cancer and whether your cancer tests positive for certain characteristics, such as having estrogen or progesterone receptors.
Coping and support
A breast cancer diagnosis can be overwhelming. And just when you're trying to cope with the shock and the fears about your future, you're asked to make important decisions about your treatment.
Everyone finds a personal way of coping with a cancer diagnosis. Until you find what works for you, it might help to:
-
Learn what you need to know about your breast cancer. If you'd like to know more about your breast cancer, ask your doctor for details — the type, stage and hormone receptor status. Ask for good sources of up-to-date information on your treatment options.
Knowing more about your cancer and your options may help you feel more confident when making treatment decisions. Still, some people may not want to know the details of their cancer. If this is how you feel, let your doctor know that, too.
-
Talk with other breast cancer survivors. You may find it helpful and encouraging to talk to other people with breast cancer. Contact the American Cancer Society to find out about support groups in your area.
Organizations that can connect you with other cancer survivors online or by phone include After Breast Cancer Diagnosis and CancerCare.
- Find someone to talk with. Find a friend or family member who is a good listener or talk with a clergy member or counselor. Ask your doctor for a referral to a counselor or other professional who works with cancer survivors.
-
Keep your friends and family close. Your friends and family can provide a crucial support network for you during your cancer treatment.
As you begin telling people about your breast cancer diagnosis, you'll likely get many offers for help. Think ahead about things you may want help with, whether it's having someone to talk to if you're feeling low or getting help preparing meals.
- Take care of yourself. Make your well-being a priority during cancer treatment. Get enough sleep so that you wake feeling rested, choose a diet full of fruits and vegetables, make time for gentle exercise on days you feel up to it, and find time for things you enjoy, such as reading or listening to music.
Preparing for your appointment
If you suspect that you have Paget's disease of the breast, your initial appointment might be with your family doctor. Or, when you call for an appointment, you may be referred directly to a doctor who specializes in treating breast conditions.
What you can do
To prepare for your appointment:
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your diet.
- Write down any symptoms you're experiencing. Include even those that may seem unrelated to the reason for which you scheduled the appointment.
- Write down key personal information. Include any major stresses or recent life changes.
- Make a list of all medications. Also include vitamins or supplements that you're taking.
- Consider taking a family member or friend along. Sometimes it can be difficult to remember all the information provided during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your doctor.
Your time with your doctor is limited, so preparing a list of questions can help you make the most of your time together. Some basic questions to ask include:
- What is likely causing my symptoms or condition?
- What are other possible causes for my symptoms or condition?
- What kinds of tests do I need?
- Is my condition likely temporary or chronic?
- What is the best course of action?
- What are the alternatives to the primary approach that you're suggesting?
- I have other health conditions. How can I best manage them together?
- Are there any restrictions that I need to follow?
- Should I see a specialist? What will that cost, and will my insurance cover it?
- Are there brochures or other printed materials that I can take with me? What websites do you recommend?
- What will determine whether I should plan for a follow-up visit?
What to expect from your doctor
Your doctor may ask you questions about:
- The nature of the skin changes on your nipple
- Whether you also experience nipple discharge, bleeding, burning or itching
- Whether you have any other breast signs and symptoms, such as a breast lump or area of thickening
- Whether you have any breast pain
- How long you've experienced signs and symptoms
Your doctor may also ask questions about your personal and family medical history and other possible risk factors for breast cancer.