Overview
Meninges
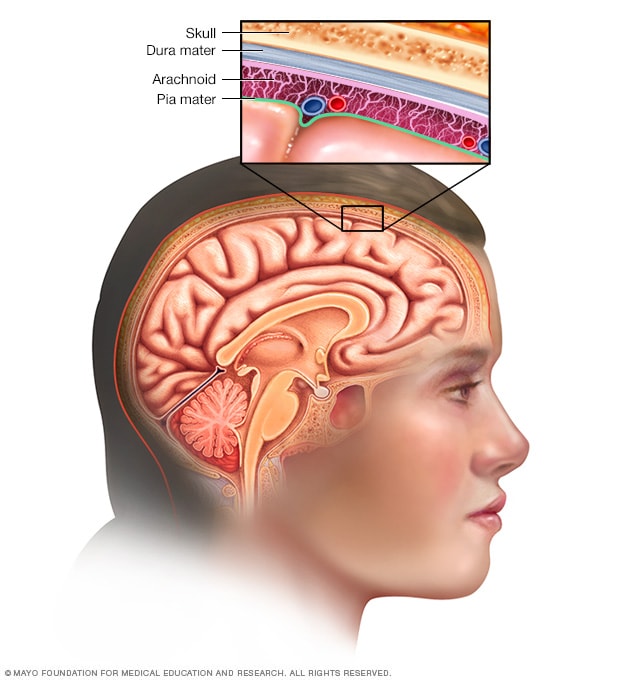
Meninges
Three layers of membranes known as meninges protect the brain and spinal cord. The delicate inner layer is the pia mater. The middle layer is the arachnoid, a web-like structure filled with fluid that cushions the brain. The tough outer layer is called the dura mater.
A meningioma is a tumor that grows from the membranes that surround the brain and spinal cord, called the meninges. A meningioma is not a brain tumor, but it may press on the nearby brain, nerves and vessels. Meningioma is the most common type of tumor that forms in the head.
Most meningiomas grow very slowly. They can grow over many years without causing symptoms. But sometimes, their effects on nearby brain tissue, nerves or vessels may cause serious disability.
Meningiomas occur more often in women. They're often found at older ages. But they can happen at any age.
Because most meningiomas grow slowly, often without symptoms, they do not always need treatment right away. Instead, they may be watched over time.
Products & Services
Symptoms
Symptoms of a meningioma most often begin slowly. They may be hard to notice at first. Symptoms may depend on where in the brain the meningioma is. Rarely, it can be in the spine.
Symptoms may include:
- Changes in vision, such as seeing double or blurring.
- Headaches that are worse in the morning.
- Hearing loss or ringing in the ears.
- Memory loss.
- Loss of smell.
- Seizures.
- Weakness in the arms or legs.
- Trouble speaking.
When to see a doctor
Most symptoms of a meningioma come on slowly. But sometimes a meningioma needs care right away.
Seek emergency care if you have:
- Sudden onset of seizures.
- Sudden changes in vision or memory.
Make an appointment to see your healthcare professional if you have lasting symptoms that worry you, such as headaches that get worse over time.
Often, because meningiomas do not cause any symptoms you notice, they are found only from imaging scans done for other reasons.
Causes
It isn't clear what causes a meningioma. Experts know that something changes some cells in the meninges. The changes makes them multiply out of control. This leads to a meningioma.
Being exposed to radiation as a child is the only known environmental risk factor for getting meningioma. There's no good evidence to show that meningiomas happen because of cellphone use.
Risk factors
Risk factors for a meningioma include:
- Radiation treatment. Radiation therapy that involves the head may increase the risk of a meningioma.
- Female hormones. Meningiomas are more common in women. This might mean that female hormones may play a role. Some studies also have suggested a link between breast cancer and meningioma risk related to the role of hormones. Some research suggests that the use of oral birth control and hormone replacement therapy could raise the risk of meningioma growth.
- An inherited nervous system condition. The rare condition neurofibromatosis 2 increases the risk of meningioma and other brain tumors.
- Obesity. A high body mass index (BMI) is a risk factor for many types of cancers. Several large studies have found that meningiomas happen more often in obese people. But the link between obesity and meningiomas is not clear.
Complications
A meningioma and its treatment can cause long-term complications. Treatment most often involves surgery and radiation therapy. Complications may include:
- Trouble focusing.
- Memory loss.
- Personality changes.
- Seizures.
- Weakness.
- Changes in the senses.
- Trouble with language.
Your healthcare professional can treat some complications and refer you to specialists to help you cope with other complications.