Diagnosis
During well-baby visits, healthcare professionals typically check for hip dysplasia by moving an infant's legs into a variety of positions that help indicate whether the hip joint fits together well. If hip dysplasia is suspected, a hip ultrasound might be ordered to check the hip joint for signs of dysplasia.
Mild cases of hip dysplasia can be difficult to diagnose and might not start causing problems until you're a young adult. If your healthcare team suspects hip dysplasia, they might suggest imaging tests, such as X-rays or magnetic resonance imaging (MRI).
Treatment
Pavlik harness
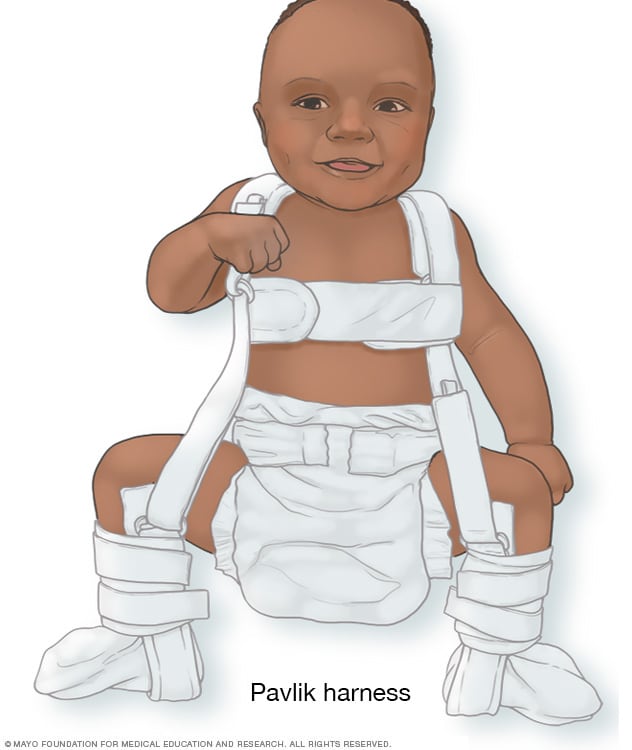
Pavlik harness
Infants are usually treated with a soft brace, called a Pavlik harness, that holds the ball portion of the joint firmly in its socket for several months. This helps the socket mold to the shape of the ball.
Spica cast
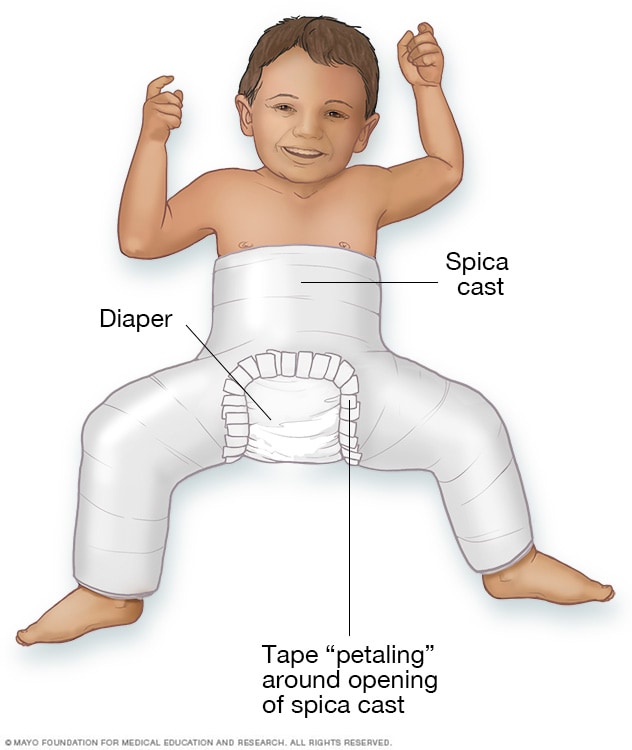
Spica cast
In some cases, the healthcare professional needs to move the hip joint bones into the proper position and then hold them there for several months with a body cast called a spica cast.
Periacetabular osteotomy
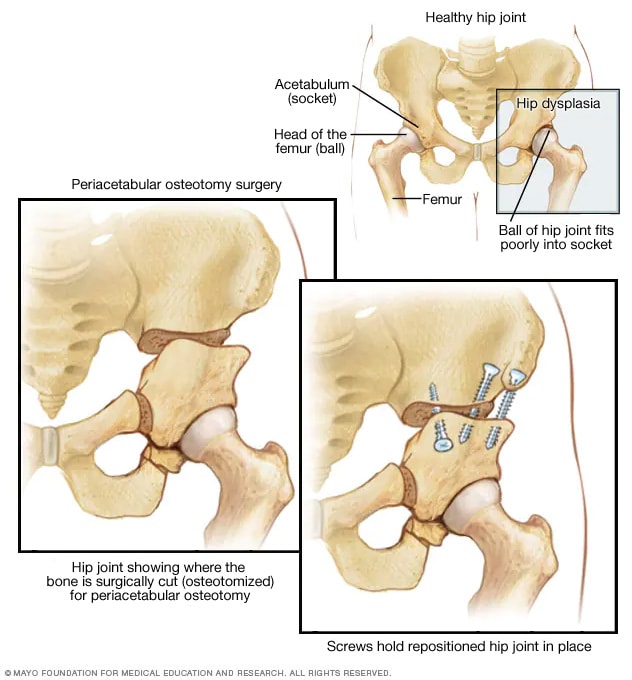
Periacetabular osteotomy
Hip dysplasia is the medical term for a hip socket that doesn't fully cover the ball portion of the upper thighbone. In periacetabular (per-e-as-uh-TAB-yoo-lur) osteotomy, the socket is repositioned in the pelvis so that it matches up better with the ball.
Hip dysplasia treatment depends on the age of the affected person and the extent of the hip damage. Infants are usually treated with a soft brace, such as a Pavlik harness, that holds the ball portion of the joint firmly in its socket for several months. This helps the socket mold to the shape of the ball.
The brace doesn't work as well for babies older than 6 months. Instead, the healthcare professional may move the bones into the proper position and then hold them there for several months with a full-body cast. Sometimes surgery is needed to fit the joint together properly.
If the dysplasia is more serious, the position of the hip socket also can be corrected. In a periacetabular (per-e-as-uh-TAB-yoo-lur) osteotomy, the socket is repositioned in the pelvis so that it matches up better with the ball.
Hip replacement surgery might be an option for older people whose dysplasia has severely damaged their hips over time, resulting in debilitating arthritis.
More Information
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Preparing for your appointment
You'll probably first bring your concerns to your family healthcare professional. They might refer you to an orthopedic surgeon.
What you can do
Before your appointment, you might want to:
- Write down any signs and symptoms you or your child are experiencing, including any that may seem unrelated to the reason for which you scheduled the appointment.
- Make a list of any medicines, vitamins or supplements that you or your child are taking.
- Consider taking a family member or friend along. Sometimes it can be difficult to remember all the information provided during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Request that a copy of previous medical records be forwarded to your current healthcare professional, if you're changing care teams.
- Write down questions to ask the healthcare team.
Your time with the healthcare professional is limited, so preparing a list of questions can help you make the most of your time together. Some basic questions to ask include:
- What's the most likely cause of the symptoms?
- What kinds of tests are needed? Do these tests require any special preparation?
- What treatments are available, and which do you recommend?
- What are the possible side effects from treatment?
- Are there any brochures or other printed material that I can take home with me?
- Can you recommend any websites for more information on hip dysplasia?
In addition to the questions that you've prepared to ask your healthcare team, don't hesitate to ask questions during your appointment at any time if you don't understand something.
What to expect from your doctor
Your healthcare professional is likely to ask you a number of questions. Being ready to answer them may reserve time to go over any points you want to spend more time on. Your doctor may ask:
- When did you or your child first begin experiencing symptoms?
- Have the symptoms been continuous or occasional?
- Does anything seem to improve the symptoms?
- What, if anything, appears to worsen the symptoms?
- If you or your child has already been diagnosed with hip dysplasia, when and where was the diagnosis made?