Overview
Nerve and damaged myelin sheath
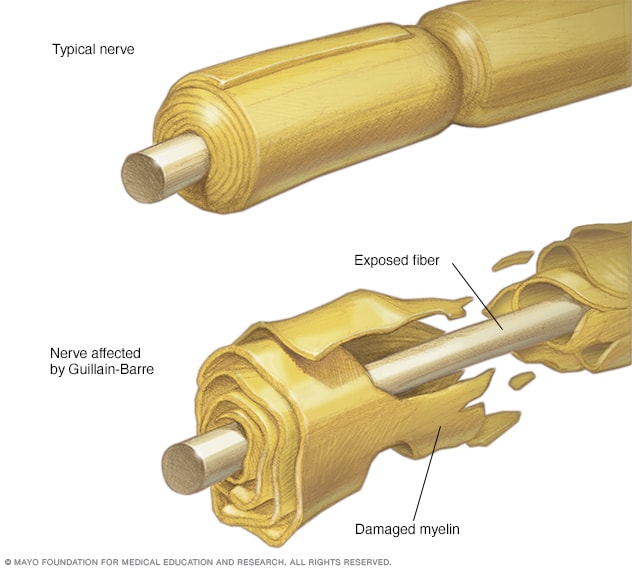
Nerve and damaged myelin sheath
The demyelinating form of Guillain-Barre syndrome destroys the protective covering of the peripheral nerves, known as the myelin sheath. This damage prevents the nerves from transmitting signals to the brain.
Guillain-Barre (gee-YAH-buh-RAY) syndrome is a condition in which the body's immune system attacks the nerves. It can cause weakness, numbness or paralysis.
Weakness and tingling in the hands and feet are usually the first symptoms. These sensations can quickly spread and may lead to paralysis. In its most serious form, Guillain-Barre syndrome is a medical emergency. Most people with the condition need treatment in a hospital.
Guillain-Barre syndrome is rare, and the exact cause is not known. But two-thirds of people have symptoms of an infection in the six weeks before Guillain-Barre symptoms begin. Infections can include a respiratory or a gastrointestinal infection, including COVID-19. Guillain-Barre also can be caused by the Zika virus.
There's no known cure for Guillain-Barre syndrome. Several treatment options can ease symptoms and help speed recovery. Most people recover completely from Guillain-Barre syndrome, but some serious illnesses can be fatal. While recovery may take up to several years, most people are able to walk again six months after symptoms first began. Some people may have lasting effects, such as weakness, numbness or fatigue.
Products & Services
Symptoms
Guillain-Barre syndrome often begins with tingling and weakness starting in the feet and legs and spreading to the upper body and arms. Some people notice the first symptoms in the arms or face. As Guillain-Barre syndrome progresses, muscle weakness can turn into paralysis.
Symptoms of Guillain-Barre syndrome may include:
- A pins and needles feeling in the fingers, toes, ankles or wrists.
- Weakness in the legs that spreads to the upper body.
- Unsteady walk or not being able to walk or climb stairs.
- Trouble with facial movements, including speaking, chewing or swallowing.
- Double vision or inability to move the eyes.
- Severe pain that may feel achy, shooting or cramplike and may be worse at night.
- Trouble with bladder control or bowel function.
- Rapid heart rate.
- Low or high blood pressure.
- Trouble breathing.
People with Guillain-Barre syndrome usually experience their most significant weakness within two weeks after symptoms begin.
Types
The symptoms of Guillain-Barre syndrome can vary based on the type. Guillain-Barre syndrome has several forms. The main types are:
- Acute inflammatory demyelinating polyradiculoneuropathy (AIDP), the most common form in North America and Europe. The most common sign of AIDP is muscle weakness that starts in the lower part of the body and spreads upward.
- Miller Fisher syndrome (MFS), in which paralysis starts in the eyes. MFS also is associated with an unsteady walk. MFS is less common in the U.S. but more common in Asia.
- Acute motor axonal neuropathy (AMAN) and acute motor-sensory axonal neuropathy (AMSAN) are less common in the U.S. But AMAN and AMSAN are more frequent in China, Japan and Mexico.
When to see a doctor
Call your healthcare professional if you have mild tingling in your toes or fingers that doesn't seem to be spreading or getting worse. Seek emergency medical help if you have any of these serious symptoms:
- Tingling that started in your feet or toes and is now moving up your body.
- Tingling or weakness that's spreading quickly.
- Trouble catching your breath or shortness of breath when lying flat.
- Choking on saliva.
Guillain-Barre syndrome is a serious condition that requires immediate hospitalization because it can worsen quickly. The sooner treatment is started, the better the chance of a complete recovery.
Causes
The exact cause of Guillain-Barre syndrome isn't known. It usually appears days or weeks after a respiratory or digestive tract infection. Rarely, recent surgery or vaccination can trigger Guillain-Barre syndrome.
In Guillain-Barre syndrome, your immune system — which usually attacks only invading organisms — begins attacking the nerves. In AIDP, the nerves' protective covering, known as the myelin sheath, is damaged. The damage prevents nerves from transmitting signals to your brain, causing weakness, numbness or paralysis.
Guillain-Barre syndrome may be triggered by:
- Most commonly, an infection with campylobacter, a type of bacteria often found in undercooked poultry.
- Influenza virus.
- Cytomegalovirus.
- Epstein-Barr virus.
- Zika virus.
- Hepatitis A, B, C and E.
- HIV, the virus that causes AIDS.
- Mycoplasma pneumonia.
- Surgery.
- Trauma.
- Hodgkin lymphoma.
- Rarely, influenza vaccinations or childhood vaccinations.
- COVID-19 virus.
Risk factors
Guillain-Barre syndrome can affect all age groups, but the risk increases as you age. It's also slightly more common in males than females.
Complications
Guillain-Barre syndrome affects your nerves. Because nerves control your movements and body functions, people with Guillain-Barre syndrome may experience:
- Trouble breathing. Weakness or paralysis can spread to the muscles that control your breathing. This can potentially be fatal. Up to 22% of people with Guillain-Barre syndrome need temporary help from a machine to breathe within the first week when they're hospitalized for treatment.
- Residual numbness or other sensations. Most people with Guillain-Barre syndrome recover completely or have only minor, residual weakness, numbness or tingling.
- Heart and blood pressure problems. Blood pressure fluctuations and irregular heart rhythms are common side effects of Guillain-Barre syndrome.
- Pain. One-third of people with Guillain-Barre syndrome experience nerve pain, which may be eased with medicine.
- Trouble with bowel and bladder function. Sluggish bowel function and urine retention may result from Guillain-Barre syndrome.
- Blood clots. People who are not mobile due to Guillain-Barre syndrome are at risk of developing blood clots. Until you're able to walk independently, you may need to take blood thinners and wear support stockings to improve blood flow.
- Pressure sores. You may be at risk of developing bedsores, also known as pressure sores, if you're not able to move. Changing your position often may help avoid this problem.
- Relapse. A small percentage of people with Guillain-Barre syndrome have a relapse. A relapse can cause muscle weakness even years after symptoms ended.
When early symptoms are worse, the risk of serious long-term complications goes up. Rarely, death may occur from complications such as respiratory distress syndrome and heart attacks.